|
 |
| J Korean Acad Pediatr Dent > Volume 46(2); 2019 > Article |
|
초록
본 연구는 7세부터 15세사이의 소아청소년을 대상으로 촬영하여 획득한 Cone beam computed tomography(CBCT) 영상을 이용하여 정중구개봉합의 성숙도를 평가하고 골 성숙도 및 연령과의 연관성을 분석하여 Rapid maxillary expansion(RME) 적용 시 적절한 치료계획 수립의 참고자료로 활용하고자 하였다. 남아 240명, 여아 240명, 총 480명의 CBCT 수평면 영상에서 정중구개봉합의 성숙도를 5단계로 평가하였고 수집된 자료를 경추골 성숙도 측정법에 의해 평가된 골 성숙도 및 연령에 따라 통계분석을 시행하였다.
정중구개봉합 성숙도와 골 성숙도는 0.602의 강한 상관관계를 보였으며, 특히 정중구개봉합 성숙도 A - C단계의 예측을 위한 경추골 성숙도 1 - 3단계의 양성 검정우도비는 44.79로서 예측을 위한 타당한 지표임을 나타내었다. 정중구개봉합 성숙도와 연령의 상관관계는 남아에서 0.499, 여아에서 0.560으로 나타나 경추골 성숙도 보다는 낮으나 비교적 높은 상관관계를 보였다. 따라서 경추골 성숙도 측정법은 정중구개봉합의 성숙도 예측을 위한 신뢰할 만한 지표라고 할 수 있으며, 연령은 경추골 성숙도 측정이 어려운 경우에 한하여 임상에서 간편하고 직관적인 지표로 쓰일 수 있다.
연구 결과를 종합해보면 RME 사용 시 골격성 효과를 충분히 얻을 수 있는 것으로 기대 할 수 있는 시기는 경추골 성숙도 1 - 3단계, 남녀 모두 연령 12세 이하이며 경추골 성숙도 4단계 혹은 여아 연령 13세 및 남아 연령 15세까지는 conventional RME의 사용은 가능하나 골격성 효과는 감소하고 치성 효과가 증가할 것으로 예상된다. 경추골 성숙도 5, 6단계 혹은 여아 연령 14세 이상에서는 RME 필요 시 사용 형태를 결정하기 위해 정중구개봉합 성숙 단계 평가 시 CBCT 촬영이 고려되어야 한다.
Abstract
This study aimed to analyze the association of midpalatal suture (MPS) maturation stages with skeletal maturation and age and to obtain references for establishing a treatment plan for rapid maxillary expansion (RME).
Cone-Beam Computed Tomography (CBCT) images from 480 children (240 boys, 240 girls) aged 7 - 15 years were obtained. MPS maturation stages and cervical vertebral maturation indicator (CVMI) were evaluated, and the correlations between MPS maturation stages, CVMI, and age were determined using the Spearman’s correlation test. The positive likelihood ratio (LHR) of CVMI for MPS maturation stages was calculated.
MPS maturation stages and CVMI showed a strong correlation. Especially, CVMI 1 - 3 showed positive LHR greater than 10 for the diagnosis of stages A - C. MPS maturation stages and age were correlated strongly in girls and moderately in boys.
Conventional RME produces the most favorable skeletal effect at CVMI 1 - 3 or those up to 12 years of age and fewer skeletal effects at CVMI 4 or at 13 years of age in girls and 13 - 15 years in boys. It is recommended to evaluate MPS maturation stages using CBCT before RME application at CVMI 5, 6 or at 14, 15 years of age in girls.
Rapid maxillary expansion (RME) has been used to expand the transverse dimension and correct the transverse discrepancy[1,2]. The therapeutic effect of RME is manifested by skeletal and dentoalveolar effects. Skeletal expansion is the widening of the maxilla by opening the midpalatal suture (MPS), whereas dentoalveolar expansion involves dental tipping and bending of the alveolar process[3]. RME is aimed at maximizing the skeletal effect and reducing the dentoalveolar effect, which may be accompanied by side effects, such as loss of periodontal attachment level, fenestration of buccal cortical bone, root resorption, and palatal tissue necrosis[4-11].
However, as the MPS matures and interdigitation increases, the skeletal effect of RME decreases and dentoalveolar effect increases[12]. To evaluate the maturation of MPS and predict the effect of RME, Angelieri et al.[13] proposed a classification method for the assessment of MPS morphology using Cone-Beam Computed Tomography (CBCT) images. However, routine CBCT in all children and adolescents may entail unnecessary radiation exposure. The use of a reliable indicator to predict MPS maturity can reduce radiation exposure in pediatric patients.
Furthermore, other studies investigated the association between MPS maturation stages and skeletal development and distribution of these maturation stages according to chronological age[13-15]. Among the methods evaluating skeletal development, cervical vertebral maturation indicator (CVMI) has been proven to be statistically and clinically reliable[16]. Although chronological age does not reflect individual variation, it is the most intuitive and easy to use parameter because it does not need additional examination for evaluation. In this study, we evaluated single racial children and adolescents, Asians only, and tried to obtain more reliable data by increasing the population size unlike previous similar studies which included western children and adults with fewer sample sizes[13-15].
This study aimed to analyze the association of MPS maturation stages with CVMI and chronological age by evaluating the MPS morphology using CBCT images in children and adolescents and to obtain references for establishing a treatment plan for RME.
This retrospective study was conducted at the Ewha Womans University Mokdong Hospital. The Institutional Review Board (IRB) of the hospital (IRB No.: 2017-11-021) approved the study prior to conducting the research.
A total of 480 patients (240 boys, 240 girls) aged 7 - 15 years who underwent CBCT (Dinnova, Willmed, Seoul, Korea) for various diagnostic purposes such as trauma, cyst, supernumerary tooth, malocclusion were included in this retrospective study. All CBCT images were obtained with the following specifications: dose, 9 mA; tube voltage, 80 kV; scanning time, 24 s; and field of view, 20 × 15 cm. Patients who had undergone orthodontic treatment previously or had congenital malformations affecting the observation of MPS morphology were excluded.
The MPS maturation stages were evaluated in the axial plane according to the method of Angelieri et al.[13], which is based on the shape of the intermaxillary bone (Fig. 1). CVMI proposed by Baccetti et al.[16] was assessed on the sagittal plane to evaluate skeletal maturation. All images were observed, without patient information, on a picture archiving and communication system (INFINITT Healthcare, Seoul, Korea) and classified by two pediatric dentists to evaluate the interexaminer reliability. The same examiners reclassified 30 randomly selected images 2 weeks later to determine the intra-examiner reliability.
The data were recorded and subjected to statistical analysis (SPSS 22.0, SPSS Inc., Chicago, IL, USA). The Spearman’s correlation test was used to investigate the correlations of MPS maturation stages with CVMI and chronological age. The association between CVMI and MPS maturation stages was evaluated using the positive likelihood ratio (LHR). The kappa coefficient was calculated to evaluate inter- and intra-examiner reliability.
The kappa coefficients for the evaluation of intra-examiner agreement for CVMI and MPS maturation stage were 0.976 and 0.974, respectively. The interexaminer reliability analysis also showed almost perfect agreement between CVMI and MPS maturation stage, with kappa coefficients of 0.969 and 0.952, respectively.
Fig. 2 and Table 1 show the distribution of MPS maturation stages according to CVMI. At higher CVMI, the incidence of MPS fusion (stages D and E) was higher. The correlation coefficient between MPS maturation stage and CVMI was 0.602 (p < 0.001), indicating a strongly positive correlation. CVMI 1 - 3 showed high positive LHR value, 44.79, for the diagnosis of stages A - C.
As shown in Table 2 and 3, MPS maturation stage and chronological age showed positively significant (p < 0.001) correlations in boys and girls (0.499 and 0.560, respectively). MPS maturation stage A was observed in boys aged up to 14 years and in girls aged up to 12 years. Stages B and C were observed for all ages. Stage D was observed in boys aged ≥ 13 years and in girls aged ≥ 11 years. Stage E was not observed in the boys included in this study (Fig. 3 and 4).
The assessment used in this study includes the classification of MPS maturation into five stages in the axial plane of CBCT images[13]. The evaluation is easier and more reproducible with CBCT than with occlusal radiographs; radiological interpretation of MPS morphology can be complicated by overlapping of anatomical structures, such as the vomer, nasal septum, and anterior nasal spine[17].
Conventional RME can be performed with less resistant forces and could have more skeletal effects at MPS maturation stages A and B than those at stage C, in which many initial ossification areas are present along MPS[18,19]. Conventional RME is still possible but may have fewer skeletal effects at stage C, limited skeletal expansion (confined to the anterior region of the maxilla) at stage D, and only dentoalveolar effects at stage E[14]. Therefore, when maxillary expansion is necessary, treatment should begin during stage A or B.
The method proposed by Baccetti et al.[16] was used to assess CVMI. According to the results of previous research, cervical vertebral maturity assessment with CBCT is reliable, showing very strong correlation with the results obtained using lateral cephalography[20]. Therefore, in this study, CVMI assessment was conducted with CBCT images in the sagittal plane.
The correlation coefficient between CVMI and MPS maturation stage was 0.602, indicating a strong correlation. In addition, positive LHR was calculated to test the validity of CVMI for predicting the MPS maturation stage. Positive LHR for CVMI 1 - 3 for the identification of the MPS maturation stages A - C was 44.79, suggesting that the prepubertal status of cervical vertebrae is a reliable indicator for MPS nonfusion (stages A - C). Therefore, when the treatment plan includes maxillary expansion in patients with CVMI 1 - 3, CBCT is not necessary to confirm the MPS fusion.
Although most subjects (87.1%) with CVMI 4, which is immediately after the pubertal growth spurt, exhibited unfused MPS, more than half of these subjects had MPS maturation stage C. These results confirmed the findings of previous studies that the skeletal effect decreases and dentoalveolar effect increases when RME is applied after the growth spurt[21].
More than half of the subjects with CVMI 5 and 6 exhibited MPS fusion (stage D and E). If MPS shows partial or complete fusion, miniscrew or surgically assisted RME should be considered, because conventional RME may result in adverse effects[22]. However, such an RME without further evaluation is excessively invasive, because almost half of the subjects with CVMI stages 5 and 6 (48.3% and 40.6%, respectively) exhibited unfused MPS. This result corresponds to previous findings that the periods of initiation and completion of MPS maturation vary widely among individuals, especially in young adolescents[17-19,23,24]. Therefore, to minimize the adverse effects of dental expansion and avoid unnecessary invasive procedures for patients with CVMI 5 and 6, CBCT should be performed for determining the appropriate type of RME.
Although some researchers have claimed that ossification of MPS is not significantly related to chronological age[12,17,18,24], the correlation between MPS maturation stage and chronological age in this study was considerably high; the correlation coefficients were 0.499 in boys and 0.560 in girls. Angelieri et al.[14] reported similar results, stating that for adolescent and young adult patients, chronological age is almost as equally accurate as skeletal maturity in predicting the MPS maturation stages and could be used as an alternative to CVMI. In boys, the stages of MPS fusion were not observed until the age of 12 years, which suggested that the skeletal effect obtained with conventional RME could be sufficient. Stage D (characterized by fusion of the palatal region) was observed in 14.8 - 26.9% of subjects aged 13 - 15 years, whereas stage E was not observed at any age. In girls, the stages of MPS fusion were rarely observed until the age of 12 years, except one case in subjects aged 11 - 12 years. Therefore, the use of conventional RME could be recommended up to the age of 12 years in girls. At the age of 13 years, 29.6% of subjects demonstrated MPS fusion, and 70.4% still exhibited an unfused MPS, thus the use of conventional RME could be possible and the expected skeletal effects are fewer than those observed at younger ages. At 14 and 15 years of age, 65.4% and 57.2% of girls, respectively, demonstrated MPS fusion.
In a study on the growth rate of maxillary suture, Björk[25] reported that the suture fusion exhibited a pubertal spurt, similar to skeletal growth, after several months than the height growth spurt. The pubertal growth spurt in girls is generally approximately 2 years earlier than that in boys; in this study, MPS fusion stages also appeared 2 years earlier in girls than in boys.
The results of this study indicated that CVMI can be reliably used to predict the maturity of MPS. However, the evaluation by chronological age alone is limited because initiation and period of maximum growth spurt vary by races, genders, and individuals[26,27]. Nevertheless, because the chronological age was also correlated relatively highly (0.499 - 0.560) with the stages of MPS maturation, it would be used as a simple and fundamental parameter when it is difficult to evaluate skeletal maturity.
The significance of this study is that it focused on Asian children and included a large population to obtain reliable references for establishing the plan of treatment for RME. However, it was limited by the fact that the number of patients exhibiting the last stage of MPS fusion was less because this study included only children and adolescents aged 7 - 15 years. Therefore, further studies complementing these findings may yield clinically useful data.
Based on our findings, conventional RME may produce the most favorable skeletal effect in patients with CVMI 1 - 3 or those up to 12 years of age. Conventional RME may be performed, in spite of fewer skeletal effects, in patients with CVMI 4 or at the age of 13 years in girls and 13 - 15 years in boys. It is recommended that MPS maturation stage be evaluated with CBCT before RME in patients with CVMI 5, 6 or at the age of 14, 15 years in girls.
Fig 1.
Schematic illustration of midpalatal suture maturation stages. (A) Schematic drawing of the maturation stages of midpalatal suture observed in axial plane of cone-beam computed tomography, (B) Decision tree for classification of the maturation stages of midpalatal suture.

Fig 2.
Distribution of midpalatal suture maturation stages according to cervical vertebral maturation indicators. CVMI = cervical vertebral maturation indicator, MPS = midpalatal suture.
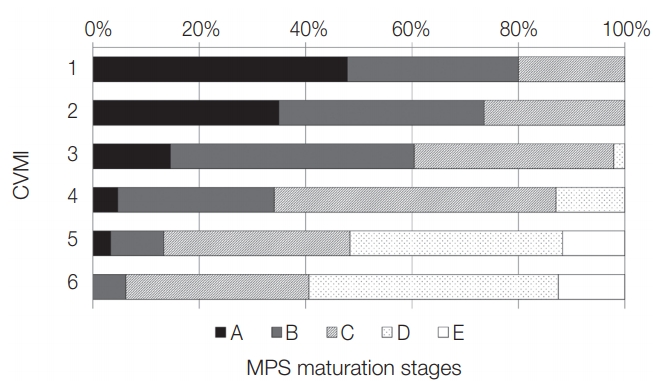
Fig 3.
Distribution of midpalatal suture maturation stages according to chronological age in boys. MPS = midpalatal suture.
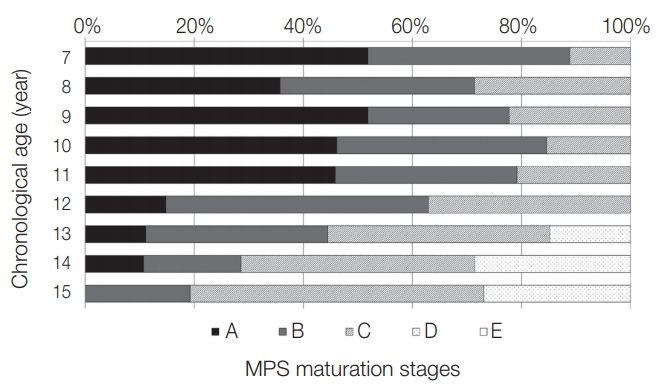
Fig 4.
Distribution of midpalatal suture maturation stages according to chronological age in girls. MPS = midpalatal suture.

Table 1.
Distribution of midpalatal suture maturation stages according to cervical vertebral maturation stages
Table 2.
Distribution of midpalatal suture maturation stages according to chronological age in boys
Table 3.
Distribution of midpalatal suture maturation stages according to chronological age in girls
References
1. Bishara SE, Staley RN : Maxillary expansion: clinical implications. Am J Orthod Dentofacial Orthop, 91:3-14, 1987.


2. Zuccati G, Casci S, Doldo T, Clauser C : Expansion of maxillary arches with crossbite: a systematic review of RCTs in the last 12 years. Eur J Orthod, 35:29-37, 2013.



3. Jacobson A : Orthodontic and orthopedic treatment in the mixed dentition. Am J Orthod Dentofacial Orthop. 104:206-207, 1993.

4. Northway WM, Meade JB : Surgically assisted rapid maxillary expansion: a comparison of technique, response, and stability. Angle Orthod, 67:309-320, 1997.

5. Timms DJ, Moss JP : An histological investigation into the effects of rapid maxillary expansion on the teeth and their supporting tissues. Trans Eur Orthod Soc. 263-271, 1971.

6. Moss JP : Rapid expansion of the maxillary arch. II. Indications for rapid expansion. JPO J Pract Orthod, 2:215-223, 1968.

7. Shetty V, Caridad JM, Caputo AA, Chaconas SJ, et al. : Biomechanical rationale for surgical-orthodontic expansion of the adult maxilla. J Oral Maxillofac Surg, 52:742-749, 1994.


8. Baysal A, Karadede I, Uysal T, et al. : Evaluation of root resorption following rapid maxillary expansion using cone-beam computed tomography. Angle Orthod, 82:488-494, 2012.


9. Barber AF, Sims M : Rapid maxillary expansion and external root resorption in man: a scanning electron microscope study. Am J Orthod, 79:630-652, 1981.


10. Langford SR, Sims MR : Root surface resorption, repair, and periodontal attachment following rapid maxillary expansion in man. Am J Orthod, 81:108-115, 1982.


11. Alpern MC, Yurosko JJ : Rapid palatal expansion in adults: with and without surgery. Angle Orthod, 57:245-263, 1987.

12. Melsen B : Palatal growth studied on human autopsy material. A histologic microradiographic study. Am J Orthod, 68:42-54, 1975.


13. Angelieri F, Cevidanes LH, McNamara JA Jr, et al. : Midpalatal suture maturation: classification method for individual assessment before rapid maxillary expansion. Am J Orthod Dentofacial Orthop. 144:759-769, 2013.



14. Angelieri F, Franchi L, Cevidanes LH, McNamara JA Jr, et al. : Diagnostic performance of skeletal maturity for the assessment of midpalatal suture maturation. Am J Orthod Dentofacial Orthop, 148:1010-1016, 2015.


15. Tonello DL, Ladewig VM, Capelozza-Filho L, et al. : Midpalatal suture maturation in 11-to 15-year-olds: A cone-beam computed tomographic study. Am J Orthod Dentofacial Orthop, 152:42-48, 2017.


16. Baccetti T, Franchi L, McNamara JA Jr : The cervical vertebral maturation (CVM) method for the assessment of optimal treatment timing in dentofacial orthopedics. Semin Orthod, 11:119-129, 2005.

17. Wehrbein H, Yildizhan F : The mid-palatal suture in young adults. A radiological-histological investigation. Eur J Orthod, 23:105-114, 2001.



18. Persson M, Thilander B : Palatal suture closure in man from 15 to 35 years of age. Am J Orthod, 72:42-52, 1977.


19. Cohen MM Jr : Sutural biology and the correlates of craniosynostosis. Am J Med Genet, 47:581-616, 1993.


20. Joshi V, Yamaguchi T, Okano T, et al. : Skeletal maturity assessment with the use of cone-beam computerized tomography. Oral Surg Oral Med Oral Pathol Oral Radiol, 113:841-849, 2012.


21. Baccetti T, Franchi L, Cameron CG, McNamara JA Jr : Treatment timing for rapid maxillary expansion. Angle Orthod, 71:343-350, 2001.

22. Suri L, Taneja P : Surgically assisted rapid palatal expansion: a literature review. Am J Orthod Dentofacial Orthop, 133:290-302, 2008.


23. Korbmacher H, Schilling A, Kahl-Nieke B, et al. : Age-dependent three-dimensional microcomputed tomography analysis of the human midpalatal suture. J Orofac Orthop, 68:364-376, 2007.



24. Knaup B, Yildizhan F, Wehrbein H : Age-related changes in the midpalatal suture. A histomorphometric study. J Orofac Orthop, 65:467-474, 2004.



25. Björk A : Sutural growth of the upper face studied by the implant method. Acta Odontol Scand, 24:109-127, 1966.


- TOOLS
-
METRICS

-
- 1 Crossref
- 0 Scopus
- 2,863 View
- 215 Download
- Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print