|
 |
| J Korean Acad Pediatr Dent > Volume 42(3); 2015 > Article |
|
초록
매복치는 유치열기보다 영구치열기에서 더 높은 빈도로 발생한다. 가장 흔하게 이환되는 치아는 상하악 제3대구치들이며, 하악 제1대구치의 매복은 비교적 드문 편이다.
매복치의 치료방법은 자발적 맹출을 위한 지속적인 검사, 외과적 노출술, 외과적 노출 후 아탈구, 교정적 견인, 그리고 외과적 재위치술 등이 있으며 이 모든 치료가 실패한다면 치아를 발거하는 것을 고려할 수 있다.
첫 번째 증례는 8세 남아로서 매복된 하악 제1대구치에 폐쇄장치를 이용한 감압술을 시행하였으며, 정기적인 검진을 통해 치아의 맹출이 관찰되었다. 두 번째 증례는 12세 남아로서 매복된 하악 제1대구치의 외과적 노출술을 시행 후 치아의 맹출이 관찰되지 않아 가철성 장치를 이용한 교정적 정출술을 시행하였으며 이 후 정상적인 치아의 맹출이 관찰되었다.
Abstract
Impacted teeth occur at higher frequencies in permanent than primary dentition. The most frequently affected teeth are the maxillary and mandibular third molars, whereas it is quite uncommon for the mandibular first molar to be impacted.
Treatment methods for impacted teeth include continuous examination for independent eruption, surgical exposure, subluxation after surgical exposure, orthodontic traction, and surgical repositioning. If all of these treatments fail, tooth extraction may be considered.
In the first case study, an 8-year-old boy was treated with surgical exposure, after which he was fitted with an obturator. His mandibular first molar then erupted successfully. In the second case, we treated a 12 year-old boy using orthodontic traction.
This study describes children with tooth eruption disorders of the mandibular first molar in mixed dentition, and reports acceptable results regarding treatment of the impacted teeth.
An impacted tooth is defined pathologically as a tooth with a crown below the oral mucosa or the bone, although the period when it was supposed to have erupted has passed. It is also defined clinically as a tooth that is not expected to erupt normally, considering the morphology, location, and direction of the tooth. The most commonly affected teeth are the maxillomandibular third molars, and impaction of the mandibular first molar is rare [1].
The treatment method of an impacted tooth in cases of potential eruption without abnormal findings is simply a periodic check-up. Treatment methods to induce eruption include surgical exposure, subluxation after surgical exposure, orthodontic traction and eruption guidance after surgical exposure, and surgical repositioning. If all of these treatments fail, surgical extraction can be an alternative [2].
Considerations about determining treatment method regarding impacted teeth include the age of the patient, the development level of the root, and factors regarding eruption disturbance. The younger the patient and the more immature the tooth, the higher the possibility of spontaneous tooth eruption. Removing the physical disturbance associated with eruption may also increase the possibility of spontaneous eruption.
In this report, two patients with mandibular first molar impaction were taken. Satisfactory results with eruption guidance to normal occlusion using surgical exposure and orthodontic traction after surgical exposure were described.
An 8-year-old boy was referred to the Department of Pediatric Dentistry, Chosun University Dental Hospital with the chief complaint of an unerupted left mandibular tooth. There was no family history or relevant medical history. In an intra-oral view, the left mandibular first molar had not erupted, whereas the right mandibular first molar had erupted normally (Fig. 1-A). In a panoramic view, the crown of the left mandibular first molar was surrounded by a well-defined radiolucent lesion (Fig. 1-B). Next, a cone beam computed tomography (CBCT) scan was performed to more specifically observe the relative locations of the tooth and lesion (CB Mercury, Hitachi, Tokyo, Japan; Fig. 1-C).
The boy was treated with surgical exposure, and then was fitted with an obturator. His mandibular first molar then erupted successfully. The radiolucent material was considered to be a/the cause of the tooth eruption disorder of the left mandibular first molar. Because tooth shape was normal and the root apex was not closed, a decompression method and surgical exposure using an obturator were intended to carry out.
After an excisional biopsy was performed, a surgical approach involving the removal of the gingiva and bony tissue above the left impacted mandibular first molar was used (Fig. 2-A). After surgical exposure, an impression for the obturator was taken, and the obturator was delivered at the next day (Fig. 2-B,C). A steel wire included in the obturator induce the obturator locating on the eruption path in panoramic radiographs. The radiolucent material was identified as a dentigerous cyst, based on the results of the biopsy.
Regular clinical and radiological check-ups were performed monthly after delivery of obturator. Part of the obturator position on its eruption path was trimmed whenever the obturator needed to be altered due to the degree of tooth development. 8 months after insertion, the appliance was removed. After 14 months, the mandibular first molar reached the normal occlusal level (Fig. 3).
A 12-year-old boy was referred to the Department of Pediatric Dentistry, Chosun University Dental Hospital with the chief complaint of an unerupted right mandibular tooth from the local dental hospital (L/C). Before referral, the patient was treated with surgical exposure at L/C for spontaneous eruption of the right mandibular first molar, but this treatment failed. There was no family history or relevant medical history. In an intra-oral view, the right mandibular first molar was unerupted, whereas the left mandibular first molar erupted normally (Fig. 4-A). A radiographic assessment showed that the impacted right mandibular first molar was apparently affected by a follicular cyst, but the tooth shape was normal and its root was substantially developed (Fig. 4-B). A CBCT scan was performed for better observation the precise relationship between the tooth and surrounding tissue (Fig. 4-C).
Considering of previous failure of eruption guidance using surgical exposure, it planned orthodontic traction after surgical exposure. After surgical removal of the gingiva and bony tissue above the right mandibular first molar, a lingual button (Tomy, Japan) connected with a ligature wire was attached on the buccal surface of the crown (Fig. 5-A). Then, equipping the removable appliance with a hook on the maxilla, the impacted right mandibular first molar was pulled using an orthodontic 3/16 inch 5 ounce intermaxillary rubber band between the maxillary removable appliance and the ligature wire. ‘Spare’space for traction in a bite plate was provided in the removable appliance (Fig. 5-B). The patient was informed to clasp and replace the orthodontic intermaxillary rubber band between the hook of the removable appliance and the ligature wire of the lingual button. Clinical and radiological check-ups were performed monthly. 11 months after insertion, the appliance was removed. After 15 months, the impacted tooth had erupted completely and surrounding tissues had developed normally (Fig. 6).
The impacted tooth is far more common in permanent than primary teeth. The impacted mandibular first molar accounts for only < 0.01% of the population, so it is a rare occurrence [3]. Proffit and Vig [4] reported that the rate of impacted teeth was higher for posterior teeth than anterior teeth. Andreasen et al. [5] described that failure of eruption can be caused by displacement of the tooth germ, a physical disturbance interrupting normal eruption, and a failure of genesis.
In a study of eruption times of mandibular first molars, Kim et al. [6] and Shin [7] reported that the mandibular first molar erupted through the alveolar bone in a half to a quarter of the time of root formation. This is consistent with the reports of Johnsen et al. [8] and Palmaetal et al. [3]. Moslemiet al indicated that tooth eruption occurred in 97% of boys in 8 years and 3 months, and in 97% of girl in 7 years and 11 months; the average eruption time was 6 years and 10 months in boys, and 6 years and 6 months in girls. Thus, clinicians should suspect impaction in cases of unerupted teeth based on these eruption times according to gender, whether there is only unilateral impaction, and whether teeth are positioned under the alveolar bone despite formation of more than half of the root.
Unlike impacted anterior teeth that are readily identifiable by family members or the patient, the impaction of the mandibular first molar is not readily detectable. For this reason, it often took a long time to notice such impacted teeth, and their advanced stage required complex treatments and was associated with a poor prognosis. Indeed, impaction of the mandibular first molar is typically found in dental check-ups, so it is important for the dentist to check carefully [2,3].
Eruption failure due to impaction delays functional occlusion, and consequently leads to malocclusion [3]. That can be caused not only by functional problems, but also by esthetic issues, such as loss of space due to the inclination of adjacent teeth, and pathological problems, such as cysts, infection, and referral pain [1]. According to Wali [10], referred pain accompanied by swelling can occur when the size of a dentigerous cyst associated with the impacted tooth is bigger than 2 cm. Especially for the first molar, this is very important because it plays a key role in mastication and the vertical occlusal relationship [2,11]. Frank [12] described the complex decisions dividing the treatment of impaction, case by case, into four types: observation, intervention, relocation, and extraction. Surgical exposure is considered a high priority for the treatment of impaction; this was supported by Nielsen et al. [13], who reported that the first molar was more likely to erupt when treated at an early stage, following early detection. Nielsen et al. [13] stated that the tooth was more likely to erupt spontaneously when the crown was uncovered and tissues interfering with its eruption path were removed surgically in cases of eruption disorders of unilateral mandibular first molars with an open apex. There are even reports that surgical exposure can induce spontaneous eruption in cases which the tooth has almost completed root development, although it is difficult to expect spontaneous eruption where there is an ankylotic impacted tooth or an unusually shaped root [14,15].
In the first case in this study, the impeding material of the dentigerous cyst was likely the cause of the tooth eruption disorder. The patient was only 8 years old, so the root of the tooth stands a good chance of developing. Thus, we could induce eruption of the tooth by surgical exposure alone, in addition to marsupializing using an obturator. Spontaneous eruption using surgical exposure can be difficult; however, here the patient was so young that the root has the potential to develop, without the dentigerous cyst causing the eruption disorder.
Decompression using a Penrose drain was considered. The Penrose drain is inexpensive and causes little discomfort. Also, it can lead to the same effect as decompression method using an obturator. However, there are also problems in that the frequent changing of the drain can produce discomfort and the number of visits to the clinic is increased. In the first case, a young patient had difficulties in visiting our hospital frequently because of distance. Thus, use of a Penrose drain was excluded.
An alternative method can be considered if spontaneous eruption by surgical exposure fails. One method is orthodontic traction of the impacted tooth, which can be divided into two types. One is a closed technique in which the tooth is exposed surgically, and then covered again after attaching a hook on it. The other is an open technique, where the exposed tooth is pulled without recovering [1]. While the prognosis of the impacted tooth is better using the closed technique, impaction right under the gingiva or mucosa is then subjected to the open technique.
In the second case in this study, orthodontic traction of the impacted molar was indicated when surgical exposure did not lead to spontaneous eruption, and no specific reason was observed. In this case, we used removable orthodontic appliances on pediatric patient’s upper and lower jaws. There was a possibility that this method could not lead to a desired result because the appliances cause the patient considerable discomfort and break her/his will to receive treatment. Therefore, this method has shortcomings such that compliance assessment is necessary before the treatment, since there is a high possibility of failure in many low-compliant patients. But, we had enough consultation before planning a treatment method and it was judged that her/his treatment compliance was good. So, we could carry out orthodontic traction therapy using removable appliances. Possible problems during orthodontic traction of impacted mandibular posterior teeth are that the elastic is not held in place with the removable maxillary appliance, and that most of the force is applied to the jawbone alone during functional movement. Thus, in this study, enough space for traction of the impacted tooth was available in the included bite plate of the removable appliance. Accordingly, it was possible to provide continuous force to it, and increase its stability.
A posterior bite plane not only made a traction space but also prevented the extrusion of the right maxillary first molar, which could have helped in resisting movement of the appliance during occlusion. However, it is difficult to use with mixed dentition and elimination, depending on the extrusion of a tooth, may be necessary.
In the second case treatment, after failure of surgical exposure carried out at a private dental clinic, orthodontic traction therapy was immediately carried out at this clinic. This case remains regrets such as spontaneous eruption could be possible though root apex formation finished and considering possibility of disturbed tooth eruption caused by unsatisfactorily removal of upper soft tissue or osseous tissue at a private dental clinic, attempting to carry out surgical exposure first could have been more conservative treatment method. Repeating the same treatment was severely unacceptable to protector and he wanted the teeth to erupt in a short time, so orthodontic traction therapy was immediately carried out.
An impacted tooth can erupt spontaneously if no specific cause disturbing the eruption is present, in cases of surgical exposure removing hard and soft tissue above the occlusal surface on the eruption path [3,15,16]. However, it is certain that an impacted tooth is less likely to erupt when there is a physical problem, such as a supernumerary tooth, odontoma, or dental follicle.
An impacted tooth may erupt spontaneously when treated surgically to remove hard and soft tissues interrupting the eruption path. Especially, spontaneous eruption may occur in cases of impacted unilateral immature mandibular first molars without complete closure of the root apex. Orthodontic traction can be recommended in cases where surgical exposure alone fails. We obtained successful results by surgical exposure in the first case and by orthodontic traction in the second case, according to the features of our patients and their teeth. On treating impacted mandibular first molars, the age of the patient, the growth level of the root, and factors causing the eruptive disturbance should be considered.
Fig. 1.
Case 1, an 8-year-old boy. On his first visit, the non-erupted state of the left mandibular first molar. (A) Intraoral view: the left mandibular first molar had not erupted, whereas the right mandibular first molar erupted normally. (B) Panoramic view. (C) Cone beam computed tomography view: the crown of the left mandibular first molar is surrounded by a well-defined radiolucent lesion.
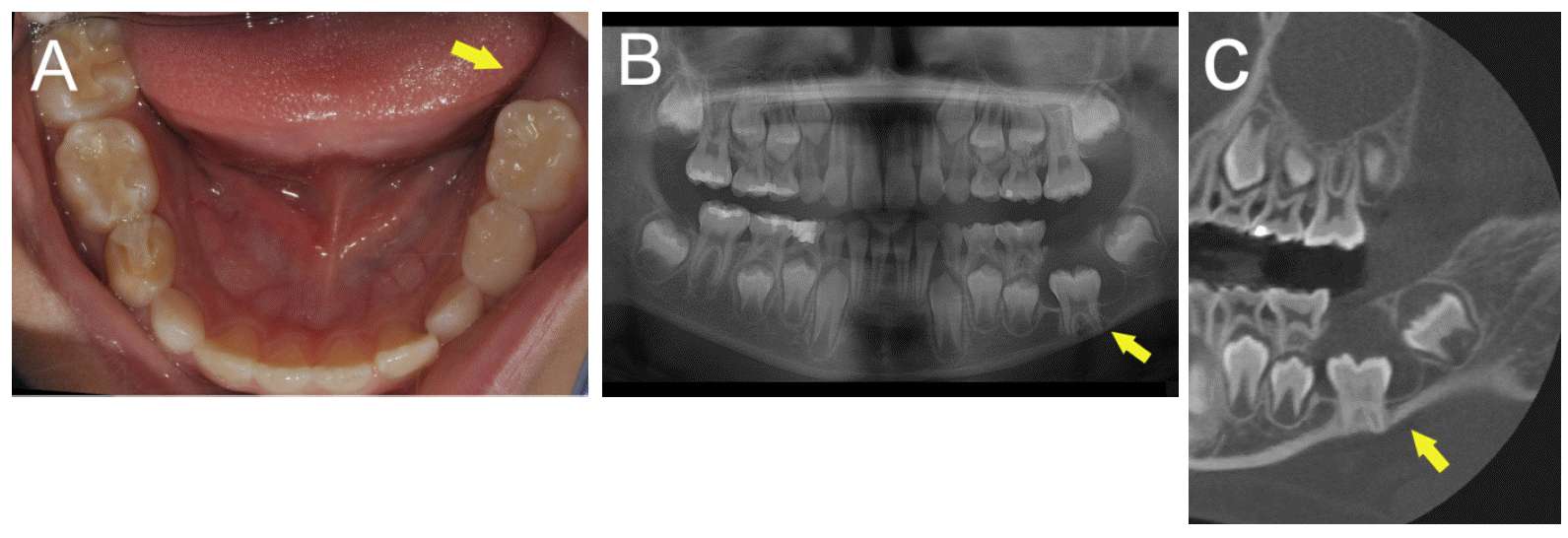
Fig. 2.
Case 1. Treatment procedure (A) A surgical approach, removing the gingiva and alveolar bone above the impacted left mandibular first molar was used to induce eruption of the impacted left mandibular first molar. (B) Obturator appliance. (C) After surgical exposure, the obturator was applied.
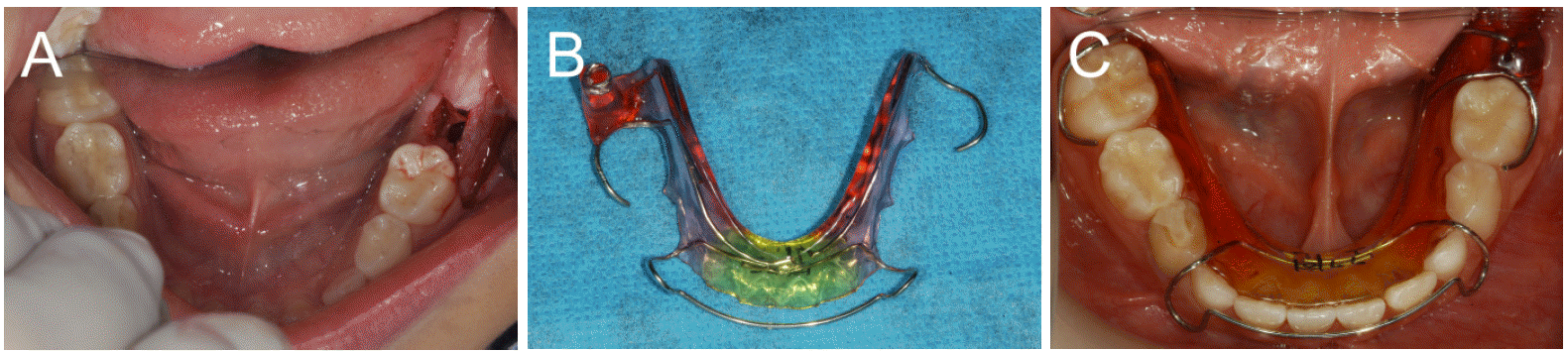
Fig. 3.
Case 1. After 14 months, the tooth had reached to the normal occlusal level. (A) Intra-oral view. (B) Panoramic view.
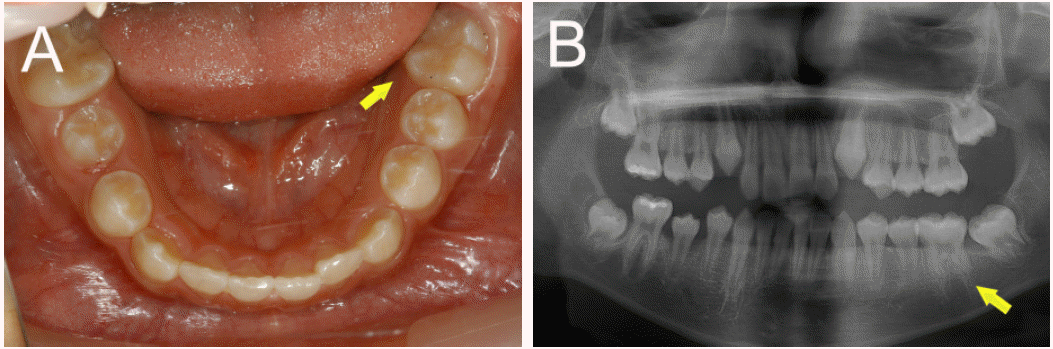
Fig. 4.
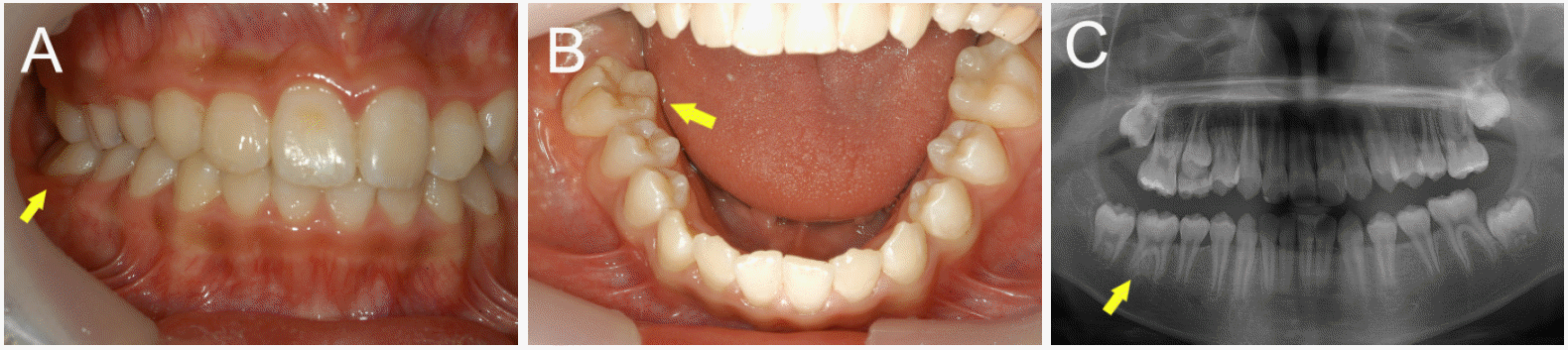
Case 2. A 12-year-old boy. On his first visit, the non-erupted state of the right mandibular first molar. (A) Intra-oral view of the patient: the right mandibular first molar had not erupted whereas the left mandibular first molar had erupted normally. (B) Panoramic view. (C) Cone beam computed tomography view: the crown and roots of the right mandibular first molar were in a normal formation.
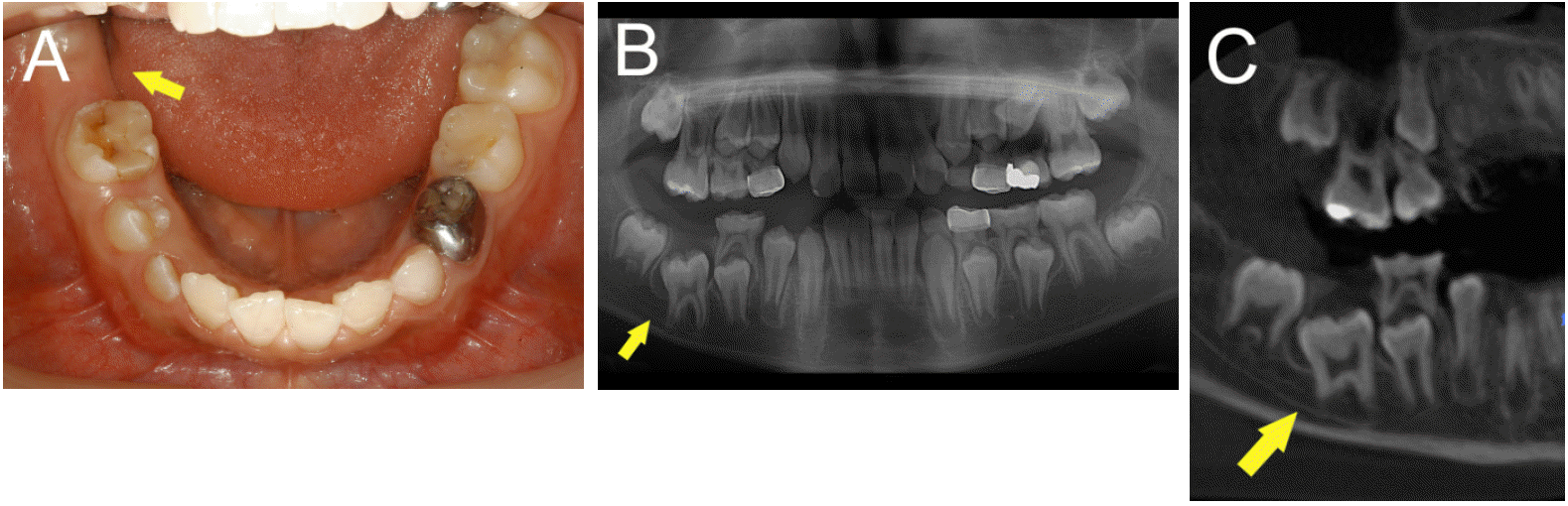
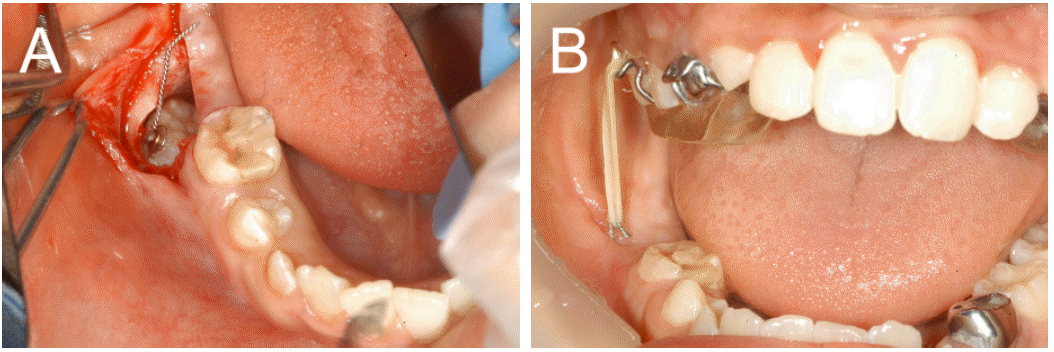
Fig. 5.
Case 2. Treatment procedure (A) Following surgical removal of the gingiva on the buccal surface, a lingual button was attached to it. (B) After 2 weeks, the removable appliance with a hook for right mandibular first molar traction was applied. Sufficient space for traction of the impacted tooth was available by including a bite plate in the removable appliance.
References
1. Korean Academy of Pediatric dentistry : Pediatric dentistry. 5th ed. Shinhung international, Inc, Seoul, 537, 2014.
2. Raghoebar GM, Boering G, Vissink A, Stegenga B : Eruption disturbances of permanent molars: a review. J Oral Pathol Med, 20:159-66, 1991.


3. Palma C, Coelho A, Gonalez Y, Cahuana A : Failure of eruption of first and second permanent molars. J Clin Pediatr Dent, 27:239-246, 2003.


4. Proffit WR, Vig KW : Primary failure of eruption: a possible cause of posterior open-bite. Am J Orthod, 80:173-90, 1981.


5. Andreasen JO, Petersen JK, Laskin DM : Textbook and color atlas of tooth impactions. Munksgaard, Copenhagen, Denmark, 199-208, 1997.
6. Kim HM, Yang SD, Nam SH, et al. : Relationship between the developmental stage and chronological age, and the changes of tooth position in relation to the tooth development on mandibular permanent teeth. J Korean Acad Pediatr Dent, 29:607-617, 2002.
7. Shin JK, Kim JG, Jeong JW, et al. : Eruption pattern of the mandibular first molar using the cone beam CT. J Korean Acad Pediatr Dent, 36:325-336, 2009.
8. Johnsen DC : Prevalence of delayed emergence of permanent teeth as a result of lacal factors. J Am Dent Assoc, 94:100-106, 1977.


9. Moslemi M : An epidemiological survey of the time and sequence of eruption of permanent teeth in 4-15-year-olds in Tehran, Iran. Int J Paediatr Dent, 14:432-438, 2004.


10. Wali GG, Sridhar V, Shyla HN : A study on dentigerous cystic changes with radiographically normal impacted mandibular third molars. J Maxillofac Oral Surg, 11:458-465, 2012.



11. Hegde S, Munshi AK : Management of an impacted, dilacerated mandibular left permanent first molar: a case report. Quintessence Int, 32:235-237, 2001.

13. Nielsen SH, Becktor KB, Kjaer I : Primary retention of first permanent mandibular molars in 29 subjects. Eur J Orthod, 28:529-534, 2006.


14. Kim EJ, Kim NJ, Nam SH, et al. : Eruption guidance of impacted mandibular first molar by surgical exposure. J Korean Acad Pediatr Dent, 31:598-604, 2004.
15. Ohman I, Ohman A : The eruption tendency and changes of direction of impacted teeth following surgical exposure. Oral Surg Oral Med Oral Pathol, 49:383-389, 1980.


16. Goho C : Delayed eruption due to overlying fibrous connective tissue. ASDC J Den Child, 54:359-360, 1987.
- TOOLS
-
METRICS

-
- 2 Crossref
- 0 Scopus
- 6,605 View
- 137 Download
- Related articles
-
Abberant Root Morphology in the Permanent First Molars : Case Reports2015 May;42(2)
Management of Eruption Disturbances of the Mandibular First Molar : A Case Report2013 November;40(4)



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print