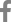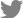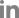|
 |
| J Korean Acad Pediatr Dent > Volume 43(3); 2016 > Article |
|
초록
틱이란 불수의적이고 갑작스러운 소리냄과 리듬이 없는 근육의 움직임을 말한다. 다수의 운동틱과 한 가지 이상의 음성틱이 모두 존재하는 경우 뚜렛 증후군으로 분류되며, 운동틱에 의한 자해 행위는 뚜렛 증후군 환자에서 흔히 나타나는 증상 중 하나이다.
본 증례에서 9세 소년이 혀의 심각한 궤양을 주소로 신경정신과로부터 의뢰되었다. 두 달 전부터 시작된 반복적인 혀 씹기에 의해 궤양은 빠르게 진행되었으며, 환아는 그로 인한 식이 및 연하의 어려움을 호소하였다. 우리는 부드러운 실리콘 재질을 이용하여 상, 하악이 분리된 가철성 장치를 제작하기로 결정하였다. 장치의 지속적 사용이 고통을 줄일 수 있는 방법임을 강조하였기 때문에, 환아는 장치 장착에 동의하였으며 잘 적응하였다. 3주 후 혀의 병소가 상당히 개선된 것을 확인할 수 있었다.
현재 구강 내 자해 행위를 치료하기 위한 표준화된 지침은 없다. 따라서 임상가는 약물 치료를 비롯하여 구강 내 장치 적용이나 관련 치아의 연마 등 다양한 접근 방법을 고려하여야 한다.
Abstract
Tourette’s syndrome is a chronic neuropsychiatric disorder characterized by the presence of vocal and multiple motor tics. Tics are defined as brief, intermittent, repetitive, unpredictable, purposeless, and stereotyped movements or sounds. Some patients experience physical pain from intense and complex tics. In addition, motor tics can result in self-injury which is a common feature of Tourette’s syndrome. A 9-year-old boy was referred by the department of neuropsychiatry because of a severe tongue laceration. His parents reported that he had been biting his tongue irregularly for 2 months before referral and suffered from an intense burning sensation. The repeated biting resulted in ulcers on the tongue, which quickly worsened and led to progressive difficulty chewing and swallowing food.
We offered to give him a two-piece removable appliance to limit tongue biting; it was made of soft silicone and fitted to both the maxillary and mandibular arches. As we emphasized that the device could help alleviate his pain, he agreed to accept it and adapted well. Just 3 weeks later, his tongue lesions had healed significantly.
A tic is characterized by involuntary, sudden, rapid, recurrent, non-rhythmic, stereotyped motor movements or vocalizations [1]. They typically wax and wane, and are usually preceded by a premonitory urge. Among tic disorders, combined vocal and multiple tic disorder is classified as Tourette’s syndrome (TS) [2]. For TS to be diagnosed, multiple motor tics and at least one vocal tic must be present over a period of a year without a break of more than 3 months.
TS develops during childhood between the ages of 2 to 13 and affects males about three to four times more often than females [1]. It can be a chronic disorder with symptoms lasting a lifetime; however, most patients experience their worst tic symptoms in their early teens, with improvement occurring in the late teens and continuing into adulthood.
More than 85% of patients with TS have common additional co-morbidities, which include attention deficit hyperactivity disorder (ADHD) and obsessive compulsive disorder (OCD). In addition, self-injurious behavior (SIB), resulted from motor tics, is commonly reported in TS patients and the estimated incidence ranges from 25% to 50% [3]. Motor tics in oral region, which can cause pain or injuries, include licking of the mouth or cheek, biting the lip or cheek, bruxism, and picking of the oral tissue using the fingernail [1].
SIB has been reported in genetic disorders such as Lesch-Nyhan syndrome, and psychiatric disorders as mental retardation, schizophrenia, borderline personality disorder, stereotypic movement disorder, and TS [4]. SIB can lead to serious complications including loss of tissue and infection [5,6], and 75% of these injuries are located in the head and neck region [7]. Many studies about oral SIB have reported intraoral appliance therapies to prevent SIB due to biting [8-13]. If all other treatments have failed or the trauma by SIB is too severe, teeth extraction can be considered.
In this report, we present a case of TS with SIB of the tongue, which rapidly worsened and resulted in wide ulceration of the tongue. We discuss the method of management to treat this patient using a removable appliance.
A 9-year-old boy was referred from the Neuropsychiatric Department with severe tongue ulceration. He had surgery at the age of 8 months for congenital heart disease, a ventricular septal defect. His psychopathological history revealed that he was diagnosed with ADHD and TS at age 8. There was no family history of either condition, but both of his parents had cerebral palsy at level II (Gross Motor Function Classification System, GMFCS).
His parents described that his behavioral and emotional development was normal until age 3, when he began to have increasingly hyperactive behavior and frequent eye blinking. By age 5, he began to exhibit obsessive-compulsive symptoms, including touching, head jerking, and limb twitching. In addition, vocal tics, humming, and sniffing appeared at age 7.
After diagnosis with ADHD and TS, pharmacological treatment including, aripipazole (antipsychotics), benztropine (anticholinergics), and escitalopram (antidepressants), and psychological therapy were started at the same time. And the antipsychotic drug was changed from aripipazole to risperidone at about 6 months ago. Despite continued therapy after diagnosis, he continued to show tics and then began biting his tongue, as an SIB limited in only tongue, which started 2 months before the referral to our clinic.
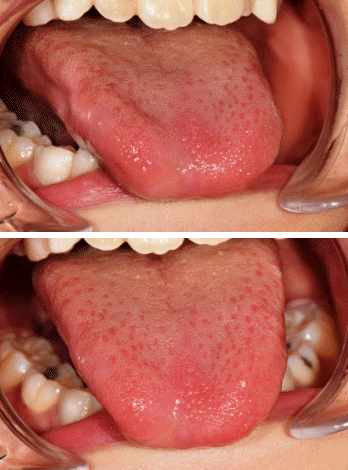
An intraoral examination revealed severe ulceration from the right side to the tip of the tongue (Fig. 1). Repeated biting quickly worsened the lesion and led to a sensation of intense burning and ultimately progressive difficulty chewing and swallowing food.
To limit SIB and prevent the possibility of severe infection, we considered conservative treatment using a removable intraoral appliance. However, according to his parents, an appliance to limit tongue biting was already tried at another clinic a month earlier, and that treatment failed because he would not use the device. The prior appliance was a one-piece splint, which the boy said was extremely uncomfortable and difficult to wear.
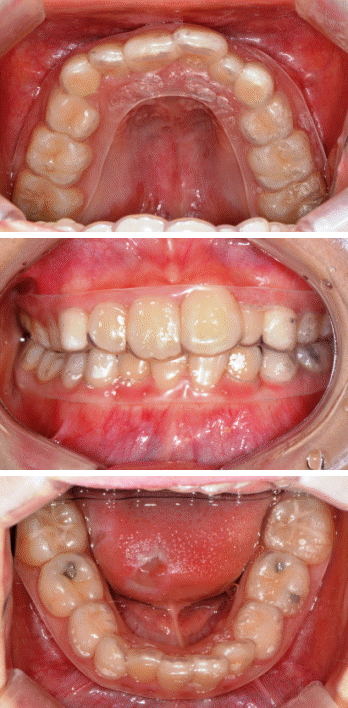
Thus, we decided to use a two-piece splint, with separate upper and lower parts. The removable appliance was made from a soft polyvinyl resilient material with about 3 mm thickness, enough to protect the tongue and reduce discomfort of patient. The appliance was applied to both the maxillary and mandibular arch (Fig. 2). In addition, we recommend application of a topical ointment and gargling with chlorohexidine.
Because we emphasized that the appliance would be more comfortable to use and would help to alleviate his pain, he agreed to accept it. He adapted well to the appliance without complaints. Just 3 weeks later, the tongue lesions had healed significantly (Fig. 3). Because the severe pain and burning sensation were reduced, his nutritional status also improved. We expected that the appliance would help to control the biting habit and emphasized that the appliance should be worn until the habit totally disappeared.
The patients did not show up for regular appointments, however, through the telephone interview after 3 months, his mother told he did not wear it during about a month and he had not bitten his tongue any more. Since the object of appliance is not to stop the habit of tongue biting, but to prevent the soft tissue damage from the tongue biting, promote healing and make him eat food more comportably, there is a possibility of recurrence for uncontolled neuropathic effect. Therefore, we explained that the appliance may have to be adjusted or remade at intervals of at least 6-12 months (recall intervals depend on the patient’s dental status) to allow for eruption of teeth and further growth, if the tongue biting is recurred.
SIBs related motor tics have commonly reported in patients with TS, and these are occurred in sudden and unpredictable condition. Thus, if the patient complains of pain due to an SIB, clinicians should consider interfering with or controlling the related tics. There are various ways to manage tics, including pharmacological and psychological approaches, and using appliances for protection. The drug therapy is considered as a treatment of choice for TS, and the neuroleptic agents, such as haloperidol and pimozide, and anxiolytics have been used [1]. Also, several psychological approaches to TS have been reported including relaxation training, massed negative practice, contingency management, self-monitoring and habit reversal [14]. However, although there has been much progress with respect to the medical treatment of TS, response rates to standard medications for TS, especially for more severe cases complicated by SIB, remain unsatisfactory [15].
Because there is no standard treatment for SIB, there have been many different approaches to prevent self-inflicted oral trauma. Dental appliances or grinding of related teeth with behavior modification techniques and pharmacological therapy can be applied for treatment of oral SIBs. Occasionally, teeth extraction has been recommended [16].
In this case, the 9-year-old patient with TS had suffered from tongue biting as an SIB for 2 months. He had already experienced failure of treatment with a one-piece splint to prevent tongue biting. According to his explanation, the major cause of failure was the inconvenience of using the previous one-piece device. As most SIBs are induced suddenly by unexpected stimuli, wearing a protective device as much as possible is important to protect one from sudden trauma. The instruction about wearing time should depend on when SIBs are developed [17-19]. Thus, if a patient with an oral SIB does not adapt to the appliance well, other types of appliance or other methods for treatment should be considered.
Previous reports have described many different approaches and appliances that prevent self-inflicted intraoral trauma [1,8,10,11,20-25]. The appliances for prevention of self-mutilation include bite blocks, oral shields, lip bumpers, and mouth guards [26]. The most commonly used oral device is a soft mouth guard [26]. The selection or design of an oral device depends on the severity and frequency of tics, the neurological status, and the prognosis [27]. The design of appliance should deflect the tissues most likely to be damaged by involuntary movements of the mandible away from the occlusal table. It must also permit full range of mandibular motion, allow for daily oral care, and withstand breakage and displacement forces [8]. In addition, it should have sufficient retention, but also can be quickly removed to facilitate airway management in the event of a respiratory emergency [11]. Although the decision for selecting fixed and removable appliances depends on the patient’s cooperation and characteristics of injuries, removable appliances are easier to insert and remove and are more hygienic compared to fixed devices [27]. The removable appliance to prevent SIB should be comfortable, because the success of the appliance depends completely on patient cooperation [8].
In this case, we chose a two-piece splint. If SIBs are associated with one side of dentition such as upper or lower lip biting, an upper or lower protective appliance can be available [1]. In this case, however, we determined that the appliance for upper and lower dentition could be more effective, since the biting lesion on tongue was developed by both. The major advantages of this two-piece appliance are that it is more convenient to wear and allowed him to eat, speak, yawn, and cough during use. The appliance was fabricated from a soft silicone material with 3 mm thickness for convenience of patient as well as protection of tongue [17,28,29], and it could provide total coverage to prevent the trauma [17]. The patient was comfortable with the appliance which was well accepted. In addition, there is no possibility of secondary injury by fracture of the appliance and it could be easily removed for oral hygiene. However, the clinician should consider the side effects for the wearing of appliance including not only temporary increase of saliva secretion and pronunciation problem, but periodontal problem by plaque retention and altered occlusion [30-32].
Early detection and intervention in patients with SIBs will favorably influence the outcome, enhancing the patients’quality of life [20]. To prevent SIB, a suitable oral appliance as a conservative method should be considered with behavioral and pharmacological therapy at the initial stages of treatment. The material and design of an appropriate appliance should be selected after careful consideration of the cause of the condition.
In addition, the most of medicines for TS patients including haloperidol and pimozide have anticholinergic properties that inhibit parasympathetic stimulation of the salivary glands, causing hyposalivation. Since the hyposalivation results in rapid progression of dental caries and periodontal disease, the dentists must concern about these potential problems [22].
In this case, the patient was referred from the neuropsychiatric department. However, as a patient with self-inflicted oral trauma may initially visit a dental clinic, dentists should keep in mind that the conditions occur in several psychiatric, behavioral, and developmental disorders. Also, the stress of dental treatment may exacerbate the tics and aberrant behaviors of patients with TS. The clinicians should recognize it and provide an accepting environment for the patients.
It is important to understand a self-inflicted oral trauma condition and develop effective methods to manage it, especially for pediatric dentists who treat patients with special needs as the patients with TS. The use of oral appliances is one useful and conservative approach to prevent SIBs. Because there are many types of appliances, clinicians should consider the situation causing the SIB and provide an appropriate appliance.
References
1. Shimoyama T, Horie N, Kato T, et al. : Tourette’s syndrome with rapid deterioration by self-mutilation of the upper lip. J Clin Pediatr Dent, 27:177-180, 2003.


2. Leksell E, Edvardson S : A case of Tourette syndrome presenting with oral self-injurious behaviour. Int J Paediatr Dent, 15:370-374, 2005.


3. Comings DE, Comings BG : Tourette syndrome: clinical and psychological aspects of 250 cases. Am J Hum Genet, 37:435-450, 1985.


4. Vito J, Jummani R, Coffey B : Advanced pediatric psychopharmacology. J Child Adolesc Psychopharmacol, 16:498-502, 2006.


5. Romer M, Dougherty N, Fruchter M : Alternative therapies in the treatment or oral self-injurious behavior: a case report. Spec Care Dentist, 18:66-69, 1998.


6. Kim MG, Yang KH, Choi NK, Kim SM : LESCHNYHAN SYNDROME: A CASE REPORT. J Korean Acad Pediatr Dent, 38:284-289, 2011.

7. Medina AC, Sogbe R, Gomez-Rey AM, Mata M : Factitial oral lesions in an autistic paediatric patient. Int J Paediatr Dent, 13:130-137, 2003.


8. Hanson GE, Ogle RG, Giron L : A tongue stent for prevention of oral trauma in the comatose patient. Crit Care Med, 3:200-203, 1975.


9. Freedman A, Sexton T, Reich D, Berkowitz RJ : Neuropathologic chewing in comatosed children: a case report. Pediatr Dent, 3:334-336, 1981.

10. Dawson LR, Hoffman JA : Treatment of a traumatic ulcer on handicapped individual: a case report. Spec Care Dentist, 2:207-208, 1982.


11. Fenton SJ : Management of oral self-mutilation in neurologically impaired children. Spec Care Dentist, 2:70-73, 1982.


12. Fabiano JA, Thines TJ, Margarone JE : Management of self-inflicted oral trauma: report of case. Spec Care Dentist, 4:214-215, 1984.


13. Sonnenberg EM : Treatment of self-induced trauma in a patient with cerebral palsy. Spec Care Dentist, 10:89-90, 1990.


14. Azrin NH, Peterson AL : Habit reversal for the treatment of Tourette syndrome. Behav Res Ther, 26:347-351, 1988.


15. Roessner V, Rothenberger A, Rickards H, Hoekstra PJ : European clinical guidelines for Tourette syndrome and other tic disorders. Eur Child Adolesc Psychiatry, 20:153-154, 2011.



16. Bowden DM, Rothenberg MB : Comprehensive care of a mentally retarded, adolescent hemophiliac with a tongue-biting tic. Pediatrics, 43:19-25, 1969.



17. Bhatia SK, Goyal A, Kapur A : Habitual biting of oral mucosa: A conservative treatment approach. Contemp Clin Dent, 4:386-389, 2013.



18. Pigno MA, Funk JJ : Prevention of tongue biting with a removable oral device: a clinical report. J Prosthet Dent, 83:508-510, 2000.


19. Hallett KB : Neuropathological chewing: a dental management protocol and treatment appliances for pediatric patients. Spec Care Dentist, 14:61-64, 1994.


20. Silva DR, da Fonseca MA : Self-injurious behavior as a challenge for the dental practice: a case report. Pediatr Dent, 25:62-66, 2003.

21. Romero M, Simon R, Garcia-Recuero JI, Romance A : Dental management of oral self-mutilation in neurological patients: a case of congenital insensitivity to pain with anhidrosis. Med Oral Patol Oral Cir Bucal, 13:E644-647, 2008.

22. Rover BC, Morgano SM : Prevention of self-inflicted trauma: dental intervention to prevent chronic lip chewing by a patient with a diagnosis of progressive bulbar palsy. Spec Care Dentist, 8:37-39, 1988.


23. Jackson MJ : The use of tongue-depressing stents for neuropathologic chewing. J Prosthet Dent, 40:309-311, 1978.


24. Park EK, Kim KC, Choi SC, Park JH : Application of the modified-mouthguard to prevent self-injurious behaviors in a child with cerebral palsy : a case report. J Korean Acad Pediatr Dent, 35:351-356, 2008.
25. Choi HI, Choi BJ, Choi HJ, et al. : Usefulness of mouth guard when the endotracheal intubation is indicated for Treacher Collins Syndrome patient. J Korean Acad Pediatr Dent, 41:40-46, 2014.

26. Jeong TS, Lee JH, Kim S, et al. : A preventive approach to oral self-mutilation in Lesch-Nyhan syndrome: a case report. Pediatr Dent, 28:341-344, 2006.

27. Kiat-Amnuay S, Koh SH, Powner DJ : An occlusal guard for preventing and treating self-inflicted tongue trauma in a comatose patient: a clinical report. J Prosthet Dent, 99:421-424, 2008.


28. Hayward JR, Trefz BR, Robert RC, Yellich GM : Soft plastic mouth guards for use in prevention of self-inflicted oral trauma. J Hosp Dent Pract, 13:36-37, 1979.

29. Croglio DP, Thines TJ, Fleischer MS, Anders PL : Self-inflicted oral trauma: report of case. Spec Care Dentist, 10:58-61, 1990.


30. Batoni G, Pardini M, Giannotti A, et al. : Effect of removable orthodontic appliances on oral colonisation by mutans streptococci in children. Eur J Oral Sci, 109:388-392, 2001.


31. Abbott DM, Bush FM : Occlusions altered by removable appliances. J Am Dent Assoc, 122:79-81, 1991.

32. Byun JS, Suh BJ : Alteration of Anaerobic Bacteria and S. mutans Count in Oral Cavity after Occlusal Stabilization Appliance Use. J Oral Med Pain, 32:375-381, 2007.
- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 9,109 View
- 149 Download
- Related articles
-
Dental Management in a Patient with Glanzmann’s Thrombasthenia : A Case Report2020 August;47(3)



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print