|
 |
| J Korean Acad Pediatr Dent > Volume 44(4); 2017 > Article |
|
ņ┤łļĪØ
ņŖżĒŗ░ļĖÉ ņĪ┤ņŖ© ņ”ØĒøäĻĄ░(Stevens-Johnson syndrome, SJS)ņØĆ Ēö╝ļČĆņÖĆ ņĀÉļ¦ēņŚÉ Ļ┤æļ▓öņ£äĒĢ£ Ļ┤┤ņé¼ļź╝ ņ┤łļלĒĢśļŖö ļ¦żņÜ░ ņŗ¼Ļ░üĒĢ£ ĻĖēņä▒ Ļ│╝ļ»╝ļ░śņØæņØ┤ļŗż. SJSņØĆ ļ¬©ļōĀ ņŚ░ļĀ╣ļīĆņŚÉņä£ ļ░£ņāØĒĢĀ ņłś ņ׳ļŖö ņ¦łĒÖśņ£╝ļĪ£ ņøÉņØĖņØĆ ļ¬ģĒÖĢĒĢśņ¦ĆļŖö ņĢŖņ¦Ćļ¦ī ļīĆļČĆļČä ņĢĮļ¼╝ ņĢīļĀłļź┤ĻĖ░ņŚÉ ņØśĒĢ£ Ļ▓āņ£╝ļĪ£ ņĢīļĀżņĀĖ ņ׳ņ£╝ļ®░ ĻĘĖņÖĖņŚÉļÅä ņäĖĻĘĀĻ░ÉņŚ╝ņŚÉ ņØśĒĢ┤ ņ£Āļ░£ļÉśĻĖ░ļÅä ĒĢ£ļŗżĻ│Ā ņĢīļĀżņĀĖ ņ׳ļŗż. ņĀäņ▓┤ Ēæ£Ēö╝ļ®┤ņĀüņØś 10% ņØ┤ĒĢśņŚÉņä£ ļ│æļ│ĆņØ┤ ļ░£ņāØĒĢ£ Ļ▓ĮņÜ░ļź╝ SJSļØ╝ ĒĢśļ®░ 30% ņØ┤ņāüņŚÉņä£ ļ░£ņāØĒĢ£ Ļ▓ĮņÜ░ļź╝ ļÅģņä▒ Ēæ£Ēö╝ Ļ┤┤ņé¼ņ£ĄĒĢ┤ļØ╝ ņĀĢņØśĒĢ£ļŗż. SJSļŖö 1ļģäņŚÉ 100ļ¦īļ¬ģ ņØĖĻĄ¼ ļŗ╣ 1 - 2ļ¬ģ ļ»Ėļ¦īņŚÉņä£ ļō£ļ¼╝Ļ▓ī ļ░£ņāØĒĢśļéś, ņä▒ņןĻĖ░ ņ¢┤ļ”░ņĢäņØ┤ņŚÉĻ▓ī ļ░£ņāØĒĢĀ Ļ▓ĮņÜ░ ņ╣śņĢäļ░£ņ£Ī ļō▒ņŚÉ ļ»Ėņ╣śļŖö ņśüĒ¢źņØä ļ»Ėņ╣śĻ▓ī ļÉ£ļŗż.
6 - 7ņäĖĻ▓Į ņāüĒĢśņĢģ ņĀ£1ļīĆĻĄ¼ņ╣śņÖĆ ĒĢśņĢģņżæņĀłņ╣śņØś ļ¦╣ņČ£ņØ┤ ņŗ£ņ×æļÉśĻ│Ā ņØ┤ ņŗ£ĻĖ░ņŚÉ ņ╣śĻĘ╝ņØś ļ░£ņ£ĪņØ┤ ĒĢ©Ļ╗ś ņØ╝ņ¢┤ļé£ļŗż. ņØ┤ ņ╝ĆņØ┤ņŖżņØś ĒÖśņĢäņØś Ļ▓ĮņÜ░ 6ņäĖĻ▓Į SJSņØ┤ ļ░£ļ│æĒĢśņśĆļŗż. Ēśäņ×¼ ņÖäņ╣śļÉ£ ņāüĒā£ņØ┤ļéś ļ¬ćļ¬ć Ēøäņ£Āņ”ØņØ┤ ļé©ņĢäņ׳ļŖö ņāüĒā£ņØ┤ļŗż. ĒÖśņĢäļŖö ņØ┤ ņŗ£ĻĖ░ņŚÉ ļ░£ņ£ĪņØ┤ ņÖäņä▒ļÉśļŖö ņ╣śņĢäņŚÉ ĻĄŁĒĢ£ļÉśņ¢┤ ļ░£ņ£ĪņØ┤ņāüņØ┤ Ļ┤Ćņ░░ļÉśņŚłļŗż. ĻĄ¼Ļ░Ģļé┤ ĒŖ╣ņ¦Ģņ£╝ļĪ£ ņØ┤ļ¤¼ĒĢ£ ņĀäņŗĀņ¦łĒÖśņØä ņ¦äļŗ©ĒĢśĻ│Ā ņØ┤ļĪ£ ņØĖĒĢ£ ņ╣śņĢä ļ░£ņ£ĪņŚÉ ļīĆĒĢ£ ņśüĒ¢źņŚÉ ļīĆĒĢ£ ļ¼ĖņĀ£ņĀÉņØä ņØĖņŗØĒĢśĻ│Ā ĒĢ┤Ļ▓░ĒĢśĻ│Āņ×É ņØ┤ ļ│┤Ļ│Āņä£ļź╝ ņō░ļŖö ļ░öņØ┤ļŗż.
Abstract
Stevens-Johnson syndrome (SJS), an extremely severe acute hypersensitivity reaction, causes extensive necrosis on the skin and the mucous membrane. SJS is a disease of unknown cause that can occur in all age groups. It is thought to be caused by drug allergy or induced by bacterial infection. Epidermal surface invasion of less than 10 percent is called SJS, and invasion of more than 30 percent is called toxic epidermal necrolysis. Although it is rare with an incidence of 1 - 2 cases per million people per year, it has effects on tooth development and therefore on children who are in a growth phase. The purpose of this case report is to examine the effect of SJS on tooth development in children.
In general, eruption of the upper and lower 1st molars and lower central incisors starts at 6 - 7 years of age. Root development also occurs at this time. In the case reported here, SJS occurred in a 6-year-old patient. Although the patient's SJS was completely cured , he still suffers from aftereffects. Developmental abnormalities in the patientŌĆÖs teeth were observed only in teeth for which root development had been completed at the time. The purpose of this case report is to illustrate how to diagnose such systemic diseases by intra-oral features and to recognize and resolve tooth development problems associated with the disease.
Stevens-Johnson syndrome (SJS), an extremely severe acute hypersensitivity reaction, causes extensive necrosis on the skin and the mucous membrane. The normally accepted mechanism of SJS is a cytotoxic immune reaction in keratinocytes that leads to widespread keratinocyte apoptosis. With less than 10% epidermal surface invasion, the disease is called SJS, and with more than 30%, it is called toxic epidermal necrolysis (TEN) [1,2]. Although bacterial and viral infections can be a causative factor in the syndrome, medication is thought to be the major cause[3]. According to previous studies, the prevalence of SJS is fewer than 1 - 2 per 100 million population per year[4].
In the early stage of SJS, clinical symptoms are similar to those of a common cold. As time passes, the erythema symptom that starts on the body spreads radically to the face and lymph nodes with efferent propagation aspects. NikolskyŌĆÖs sign can be observed, and blister like lesions can also be detected on the eyes, lips, esophagus, mucosa of the genital organs, and even the internal organs[5-7]. Intra-oral findings in adults are limited to soft tissue, which can how ulcerative lesions and blisters[8]. However, intra-oral symptoms in growing children are not limited to soft tissue but also pose disadvantages to tooth development[8-13]. Currently, only a few foreign studies about developmental disturbance of the permanent teeth related on to SJS have been reported, and no domestic studies have been published so far.
In this study, an SJS patient with symptoms of developmental disturbance of the permanent teeth and intra-oral aftereffects will be introduced.
A 9-year-old male patient visited a pediatric dental clinic with a chief complaint of abnormal root development and tooth pain. Early in February 2012, the local clinic prescribed medication for the patient, who had fever, headache, and vesicles on the lips. On the next day, the patient visited emergency room in Chunnam National University Hospital, where he was diagnosed as SJS, complaining his acute erythema on entire body, bilateral conjunctiva with exudate, and swelling on left neck. After subsequent empirical antibiotics administration and follow up, he had recovered completely. The aftereffects appeared to include a symblepharon of the left eyeball, cicatrizing atrophia of the tongue surface, and stricture of the external genital urethra (Fig. 1).
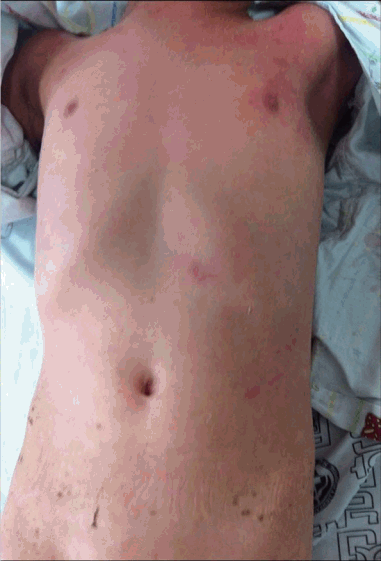
In the present case, the 5-year-old patient was given local medication for a common cold with fever and headache. After 2 days, vesicles appeared, and after 3 days, the patient went to the hospital emergency room with symptoms of mumps and pneumonia, along with spots over the entire body and swelling of the neck. On the fifth day, SJS worsened to TEN, with additional symptoms of NikolskyŌĆÖs sign and spots over the entire body, exudation in both eyes, lesions in the mouth and on the external genital organs, edema in the neck, and a drowsy state (Fig. 2). Continuos steroid therapy was initially conducted, and intravenous immune globulin injection was performed as required. The patient was prescribed a number of antibiotic agents to prevent secondary infection as well. On day 13, the progression of skin lesions stopped and, the patient's overall condition improved (Fig. 3). Finally, the patient was discharged from the hospital after a month. Although the patient's TEN was completely cured , he still suffers from aftereffects such as a symblepharon, cicatrizing atrophia of the tongue surface, and stricture of the external genital urethra.
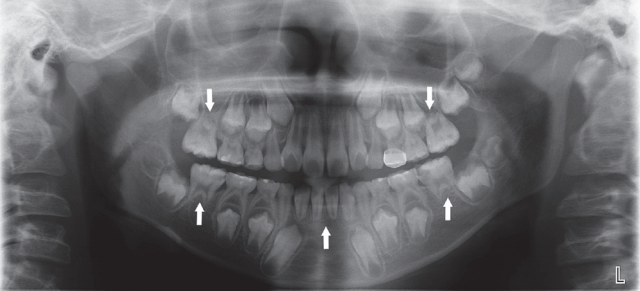
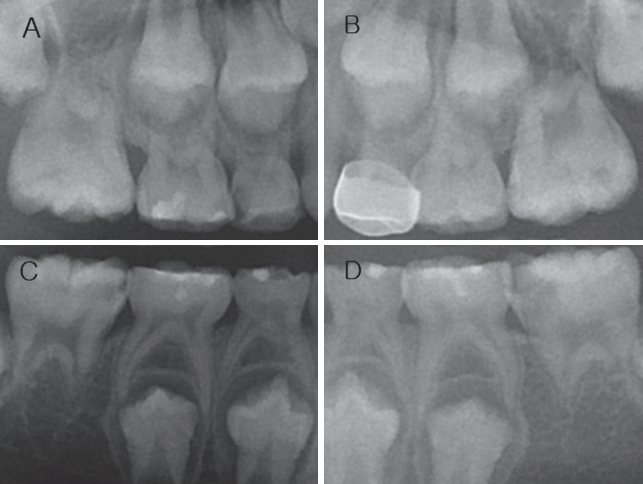
During oral examination, caries was detected on the occlusal surface of 1st molar of the maxilla and mandible and the mesial proximal surface of 1st primary molar of the right maxilla and central incisor of the right mandible. Additionally, a number of teeth were suspected of hypomineralization (Fig. 4). On radiologic examination, abnormal root development of the maxilla and mandibular 1st molars and lateral and central incisors of the mandible was detected (Fig. 5, 6). However, mobility and percussion inspections revealed no specific findings. Restorative treatment was used to treat the caries. The 1st molar of the left mandible, which had the most severe dental caries, was treated with caries removal and partial pulpectomy for maximal conservative treatment because root canal treatment would be hard to perform due to abnormal root development and the patientŌĆÖ s young age. Thereafter, composite resin restoration was performed above biodentine application. After removal of the remaining tooth caries, composite resin restoration was performed on each tooth. The maxillary right 1st primary molar was treated by preformed crown restoration after caries removal.
After all treatments were completed, regular follow-up was planned to observe the patientŌĆÖs prognosis (Fig. 7).
SJS and TEN, a form of acute severe mucocutaneous reaction, are rare diseases and the specific cause is still unknown. The best known putative causal agents are certain medications[1,2]. A cytotoxic immune reaction of keratinocytes leads to widespread keratinocyte apoptosis. At the beginning of SJS, erythematous spots appear on the skin, then the fused erythematous spots become blisters and cause widespread skin flakes. Finally, the erythematous spots invade mucous membrane[14]. The two diseases are thought to be sequential; the only difference is the degree of invasion[15-17]. As mentioned above, there is a high chance that both SJS and TEN are caused by certain medications such as commonly used antibiotics or NSAIDs[6,7,16]. Drugs prescribed to treat other diseases may cause the syndrome, and causative drugs can only be confirmed by medical history. Therefore, finding a causative drug is not easy. The causative drug is most likely one taken within 4 weeks prior to onset[7]. The lesions observed in these syndromes, purple spots or an atypical lesion with uncertain boundaries, start at the center of the body and gradually spreads to the limbs. The most affected parts of the body are the oral mucosa layer and the eye. Necrosis of the affected mucosa layer results in connective tissue exposure, followed by loss of electrolytes and infection[6,7].
The most important priority for control of SJS is prevention of early disease progression. Therefore, it is important for a patient to stop using the causative drug immediately. Additionally, local steroid therapy is generally used, and a combination of an antihistamine agent and an analgesic agent is also used in minor cases[6,7,18]. In severe cases, a systemic corticosteroid administration may be recommended[19,20]. Depending on the symptoms, a patient may need water and electrolyte control, prevention of secondary infection, and elimination of necrotic tissue under intensive care in a burn unit[6,7].
In this case, abnormal root development of 1st molars of the maxilla, 1st molars, central incisors, and lateral incisors of the mandible was observed. It is likely that abnormal root development of the teeth was caused by the onset of SJS, considering that root development is completed at around 7 year[8-13].
Abnormal root development can be assumed to occur as follows : 1) Keratinocytes found in Hertwig's epithelial root sheath cells play important roles in root developmet; 2) SJS provokes apoptosis of the keratinocytes. 3) this apoptosis event inhibits the differentiation of dental papilla cells to odontoblasts; 4) the limited number of odontoblasts induces malformation of the root dentin during root developmental. As a result, abnormal root development occurs[8,21].
From this case, the following issues arise related to the dental symptoms of this SJS patient (abnormal root development and dental caries). First, the abnormal root development reflects the age of onset in a given patient, so regular dental management is needed. Ranalli et al. reported that this abnormality most frequently occurred in premolars and the 2nd molars[22], so regular follow-up should be performed. Second, the functional examination should be conducted as well to manage aftereffects such as atrophic lesions on the tongue. Finally, this case points to two treatment limitations. First, the use of dental medications was limited, as the causative drug could not be defined at the time. Second, given that there was only a short period of time for follow-up, we could not observe the long-term outcomes. Therefore, long-term regular follow-up should be performed to observe the outcomes in immature premolars and the 2nd molar and preserve the teeth as long as possible.
In the case, the patient visited dental hospital with a chief complaint of dental caries treatment. As a result of clinical examination, the number of dental caries were found and the aftereffect appeared to include cicatrizing atrophia of the tongue surface. On radiographic examination, abnormal root development of the maxillary and mandibular 1st molars and mandibular incisors were observed. It is thought that the abnormalities were resulted by the onset of SJS at his age 5 when the teeth germs were developing. The patient is now in the mixed dentition. So it is necessary to observe the possibility of further morphologic deformities in (maxillary and mandibular) premolars and 2nd molars, and the long-term maintenance of teeth with root abnormalities.
Fig.┬Ā1.
One lasting effect of the disease in this patient (A) Symblepharon of the left eyeball, (B) Cicatrizing atrophia of the tongue surface.
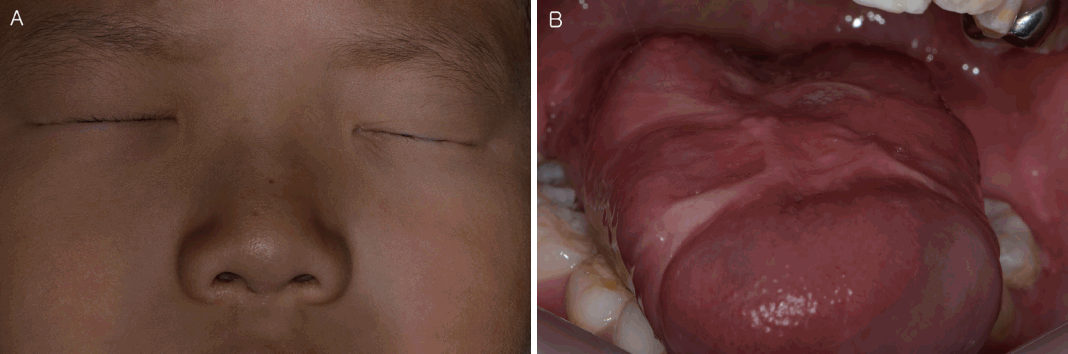
Fig.┬Ā2.
Clinical state on th fifth day. (A) Nikolsky's sign on the face and body, (B) Nikolsky's sign on the body.
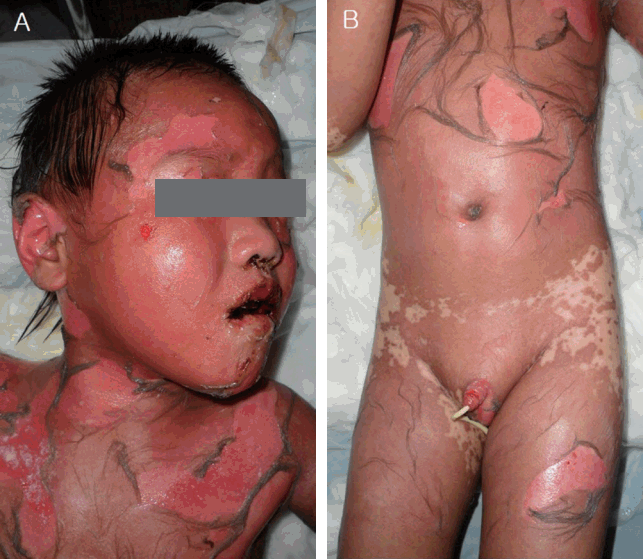
Fig.┬Ā4.
Pre-treatment intraoral view. Non specific finding without dental caries. (A) Facial view, (B) Maxillary occlusal view, (C) Mandibular occlusal view.
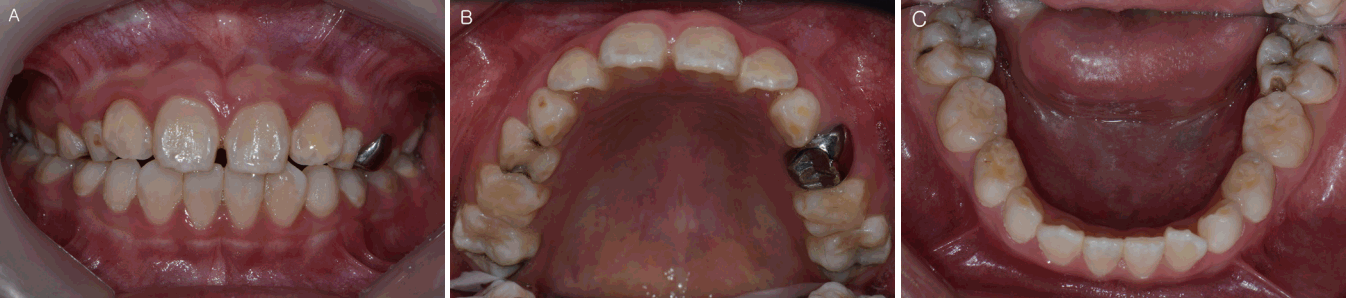
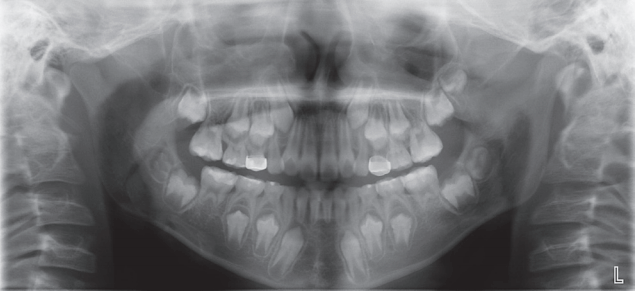
Fig.┬Ā5.
Panoramic radiographic view at the initial visit shows abnormal root development of the maxillary 1st molar, both mandibular 1st molars, and anterior mandibular teeth(arrowhead).
References
1. Borchers AT, Lee JL, Gershwin ME, et al. : Stevens-Johnson syndrome and toxic epidermal necrolysis. Autoimmun Rev, 7:598-605, 2008.


2. Łoboda J, Dudzik A, Chomyszyn-Gajewska M : Stevens-Johnson syndrome and toxic epidermal necrolysis-based on literature. Przegl Lek, 72:35-37, 2015.

3. Tristani-Firouzi P, Petersen MJ, Zone JJ, et al. : Treatment of toxic epidermal necrolysis with intravenous immunoglobulin in children. J Am Acad Dermatol, 47:548-552, 2002.


4. Prins C, Kerdel FA, French LE, et al. : Treatment of toxic epidermal necrolysis with high-dose intravenous immunoglobulins: multicenter retrospective analysis of 48 consecutive cases. Arch Dermatol, 139:26-32, 2003.


5. Auquier-Dunant A, Mockenhaupt M, Roujeau JC, et al. : Correlations between clinical patterns and causes of erythema multiforme majus, Stevens-Johnson syndrome, and toxic epidermal necrolysis: results of an international prospective study. Arch Dermatol, 138:1019-24, 2002.


6. Harr T, French LE : Stevens-Johnson syndrome and toxic epidermal necrolysis. Chem Immunol Allergy, 97:149-166, 2012.


7. KDA Textbook editing board : Dermatology. 5th ed. Ryomoongak, 221-227, 2008.
8. Bajaj N, Madan N, Rathnam A : Cessation in root development: ramifications of 'Stevens-Johnson' syndrome. J Indian Soc Pedod Prev Dent, 30:267-270, 2012.


9. De Man K : Abnormal root development, probably due to erythema multiforme (Stevens-Johnson syndrome). Int J Oral Surg, 8:381-385, 1997.

10. Brook U : Stevens-Johnson syndrome and abnormal root development: a case report. Int J Paediatr Dent, 4:101-103, 1994.


11. LIBRACH IM : Erythema multiforme bullosa (Stevens-Johnson Syndrome); some observations on pathogenesis and on treatment with cortisone and ACTH. Postgrad Med J, 31:570-574, 1995.

12. Shetty SR, Chatra L, Shenai P, Rao PK : Stevens-Johnson syndrome: a case report. J Oral Sci, 52:343-346, 2000.

13. Apajalahti S, H├Čltt├ż P, Turtola L, Pirinen S : Prevalence of short-root anomaly in healthy young adults. Acta Odontol Scand, 60:56-9, 2002.


14. Bachot N, Roujeau JC : Differential diagnosis of severe cutaneous drug eruptions. Am J Clin Dermatol, 4:561-572, 2003.


15. Fritsch PO, Sidoroff A : Drug-induced Stevens-Johnson syndrome/toxic epidermal necrolysis. Am J Clin Dermatol, 1:349-360, 2000.


16. Bastuji-Garin S, Rzany B, Roujeau JC, et al. : Clinical classification of cases of toxic epidermal necrolysis, Stevens-Johnson syndrome, and erythema multiforme. Arch Dermatol, 129:92-96, 1993.


17. Assier H, Bastuji-Garin S, Revuz J, Roujeau JC : Erythema multiforme with mucous membrane involvement and Stevens-Johnson syndrome are clinically different disorders with distinct causes. Arch Dermatol, 131:539-543, 1995.


18. Oliveira LR, Zucoloto S : Erythema Multiforme Minor: A Revision. American Journal of Infectious Disease, 4:224-231, 2008.


19. Del Pozzo-Magana BR, Lazo-Langner A, Rieder MJ, et al. : A systematic review of treatment of drug-induced Stevens-Johnson syndrome and toxic epidermal necrolysis in children. J Popul Ther Clin Pharmacol, 18:121-133, 2011.
20. Bachot N, Revuz J, Roujeau JC : Intravenous immunoglobulin treatment for Stevens-Johnson syndrome and toxic epidermal necrolysis: a prospective noncomparative study showing no benefit on mortality or progression. Arch Dermatol, 139:33-36, 2003.


- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 7,325 View
- 378 Download
- Related articles
-
Oral Features in a Child with Noonan Syndrome : A Case Report2018 February;45(1)
Dental Treatment of a Wolf-Hirschhorn Syndrome Patient: A Case Report2016 August;43(3)
Basal Cell Nevus Syndrome : A Case Report2014 May;41(2)
Nevoid Basal Cell Carcinoma Syndrome : A Case Report2014 February;41(1)



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print