국소적 치아이형성증의 임상적 방사선학적 연구: 5년 추적관찰
A Clinical and Radiological Study of Regional Odontodysplasia: Five-year Follow-up
Article information
Abstract
국소적 치아이형성증(Regional Odontodysplasia)은 드물게 발생하는 발육성 장애로, 이환된 치아는 임상적, 방사선학적, 조직학적으로 특징적인 소견을 보인다. 국소적 치아이형성증은 유치열과 영구치열에 모두 영향을 미치며, 임상적으로 정상치아보다 크기가 작거나, 거칠고 불규칙한 치면을 가지는 등 형성부전, 석회화부전의 양상을 보인다. 방사선학적으로는 법랑질과 상아질이 얇고, 경계가 뚜렷하지 않아 방사선불투과성이 명확하지 않으며,“ ghost-like appearance”와 같은 특징적인 소견을 보인다. 조직학적으로는 저석회화된 법랑질이 보이며, 법랑소주가 불규칙한 방향을 나타내고, 상아세관의 수가 감소되어 있다.
국소적 치아이형성증의 원인은 정확히 밝혀지지 않았으며, 상악 좌측에서 호발하고, 인종간의 유병률 차이는 존재하지 않으며, 남성에 비해 여성에서 더 호발하는 것으로 알려져 있다.
이 증례는 4세 6개월의 환아에서 임상적, 방사선학적 검사 결과 상악 우측 악궁에 발생한 국소적 치아이형성증으로 진단하고, 5년간의 주기적인 관찰을 시행하였다. 국소적 치아이형성증에 이환된 치아는 취약한 치면과 미성숙한 치근 때문에 예후가 불량할 수 있으므로 개개치아에 대한 주의깊은 임상적, 방사선학적 관찰을 통한 시기적절한 치료계획 수립이 중요할 것이다.
Trans Abstract
Regional odontodysplasia (RO) is a rare and nonhereditary dental malformation. It is a dental alteration of unknown etiology, involving both mesodermal and ectodermal dental components, which is characterized by clinical, radiographic, and histologic features.
The maxilla is more often involved than the mandible (especially the left side), and there is no racial predilection, but females are affected twice as often as males. The affected teeth are clinically hypoplastic and hypocalcified, presenting a“ ghost-like”appearance radiographically.
The present case features a male patient aged 4 years and 6 months who was diagnosed with regional odontodysplasia in the maxilla on the right side, confirmed by clinical and radiographic examination, with a follow up of 5 years.
Since teeth affected by RO have a poor prognosis due to the fragile tooth surface and open apices, the longterm treatment strategy depends on periodic clinical and radiological observations.
Ⅰ. Introduction
Regional odontodysplasia (RO) is an uncommon and nonhereditary developmental disorder affecting dental tissues derived from both the mesoderm and ectoderm [1,2].
The condition can affect both the primary and the permanent dentition and can occur in the maxilla, the mandible, or both. The maxilla is involved twice as often as the mandible, with the maxillary central and lateral incisors and canines more affected than the posterior teeth [3]. RO is usually unilateral and rarely crosses the midline [1]. The criteria for diagnosis of RO are primarily clinical and radiographic findings, supported by histologic features [4,5].
Clinically, a tooth affected by RO appears hypoplastic and hypocalcified with an abnormal morphology and an irregular surface [6]. Radiographically, there is a lack of contrast between the enamel and dentin, both of which are less radiopaque than the unaffected region. Additionally, enamel and dentin layers are thin, which gives the teeth a “ghost-like”appearance [7]. The dental follicles and pulp chambers are usually enlarged and the root apices are open [5].
This paper reports a case of RO on the maxillary right arch associated with early exfoliation of the affected deciduous teeth and delayed eruption of the affected permanent teeth with typical clinical and radiographic features over 5 years of follow up.
Ⅱ. Case Report
A 4-year-old male presented to the Department of Pediatric Dentistry at the Daejeon Dental Hospital of Wonkwang University, with a chief complaint of unerupted permanent right maxillary teeth after losing the maxillary primary incisors in 2009. Both parents reported no significant history of prenatal anomalies on either side of the family. His prenatal, natal, and medical history was unremarkable.
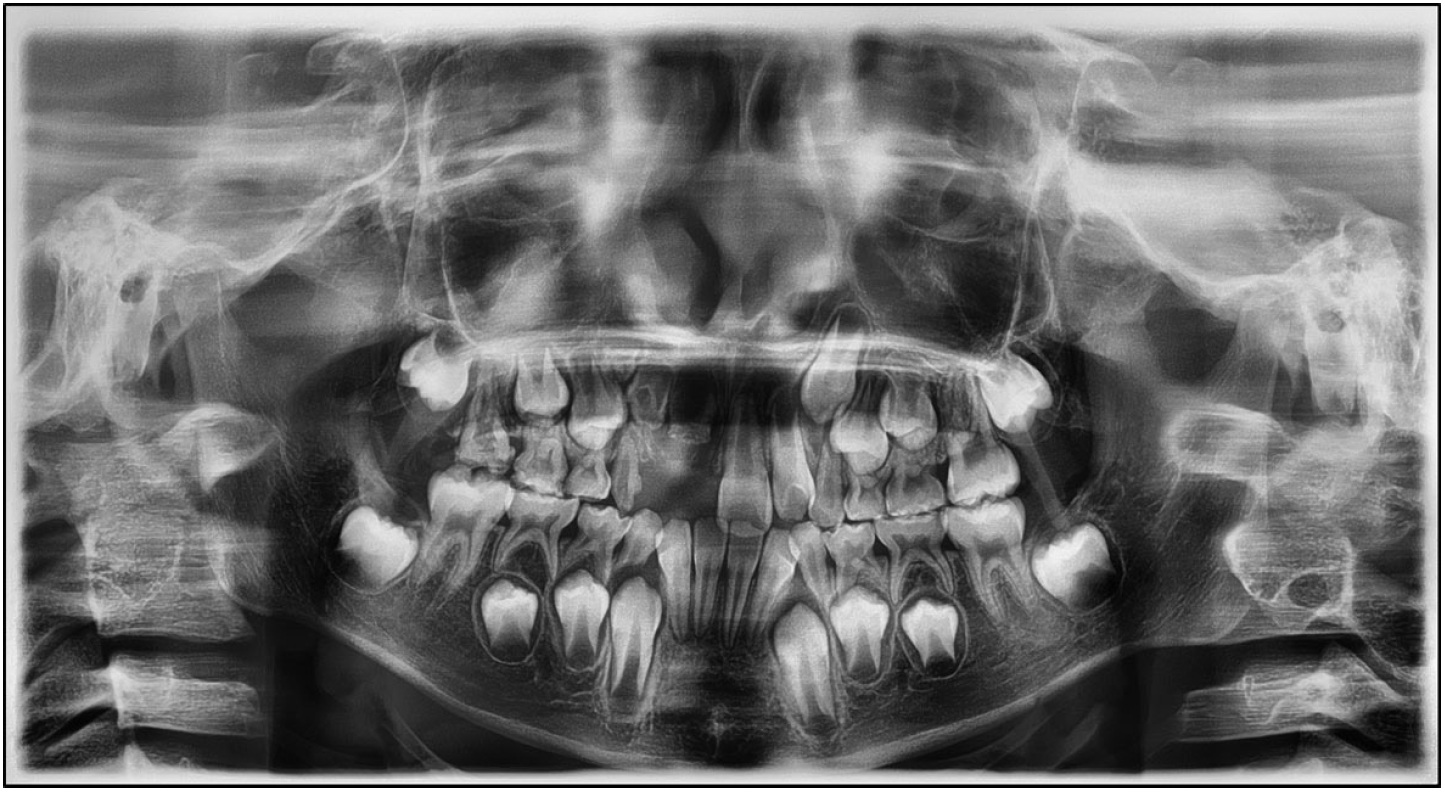
On intraoral examination, the deciduous central incisor and lateral incisor of the maxillary arch on the right side were exfoliated and the rest of the teeth in the right quadrant of the maxilla had abnormal crowns, with hypoplastic enamel, especially the deciduous canine. All other primary teeth of the other quadrants were normal. Radiographically, the maxillary right deciduous canine tooth and the germs of the maxillary right permanent central incisor, lateral incisor, canine, and the first molar were all reduced in radiodensity and were immature compared to the unaffected teeth (Fig. 1A). Periapical radiographs of the deciduous canine demonstrated very thin dentin and enamel layers. A demarcation between them was not observed, and pulp chambers were noticeably enlarged (Fig. 1B). Thus, the affected regions demonstrated a characteristic“ ghost-like”appearance.

On Initial radiographic view. (A) Panoramic view. The maxillary right deciduous and permanent teeth were reduced in radiodensity in comparison to the unaffected teeth. (B) Periapical view. The affected deciduous canine tooth demonstrated very thin dentin and enamel layers. A demarcation between them was not observed, and pulp chambers were wide.
On the basis of our clinical and radiological findings, a diagnosis of RO of the right maxilla was proposed.
The affected edentulous quadrant was rehabilitated with a removable anterior aesthetic appliance (Fig. 2). The patient has been placed on periodic recall to observe the progress of eruption of the maxillary right teeth and to monitor the growth and development of the maxillary and mandibular dental arches for the next 5 years.
On recent examination, the maxillary right first molar had erupted in the oral cavity, although it showed abnormal morphology with an irregular yellowish-brown surface (Fig. 3). Radiographically, the root formation of the maxillary first molar seems to have proceeded somewhat, but with thin dentin and enamel layers as previously and the enamel layer was mostly absent (Fig. 4A). The maxillary right permanent central incisor and lateral incisor had not erupted yet, and on radiographic findings, slow growth of the dental root was observed, while still showing a“ ghost-like”appearance (Fig. 4B, 5). The root of the deciduous canine had matured and the size of the pulp chamber had decreased over 5 years despite an unclear demarcation between the enamel and dentin (Fig. 4B). Radiographic findings of the first and second premolars of the affected quadrant were nearly normal, and the deciduous canine and premolars are currently well maintained without signs of pain or abscess.

The maxillary right first molar was erupted, although it showed abnormal morphology with an irregular yellowish-brown surface and the maxillary right permanent central incisor and lateral incisor had not erupted.
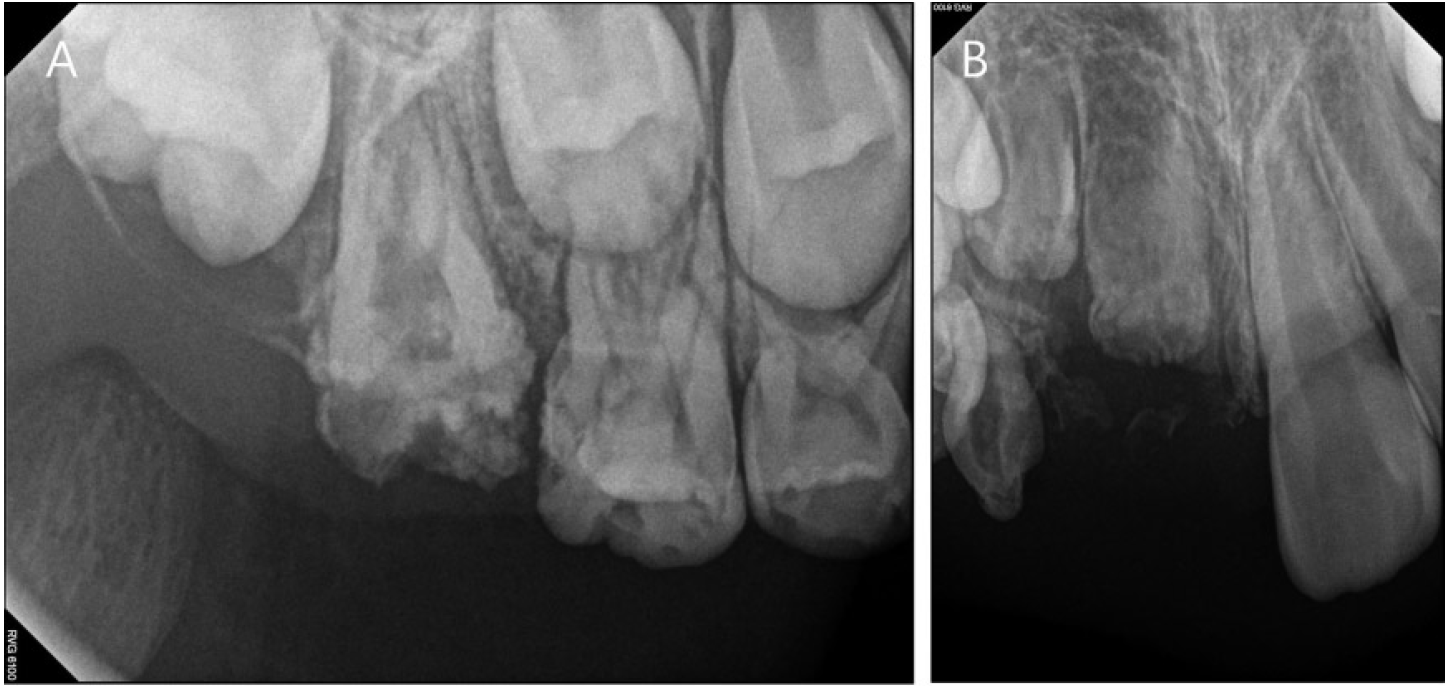
Periapical view at 5 years follow-up. (A) The root formation of the maxillary first molar seems to have proceeded somewhat, but with thin dentin and enamel layers as before. (B) The maxillary right permanent central incisor and lateral incisor had not erupted yet, and on radiographic findings, slow growth of the dental root was observed.
Ⅲ. Discussion
RO is a relatively rare, localized developmental anomaly that affects both the dentin and enamel of a group of adjacent teeth. It occurs in both deciduous and permanent dentition [4]. RO has no racial predilection and affects females more often than males [2]. This condition mostly affects one quadrant, especially the left maxilla [8-10]. The condition was first described by Hitchin [11] in 1934, although the first report was published by McCall et al. [12] in 1947.
The etiology of RO is unclear. However, many theories have been proposed, such as nutritional deficiencies, local trauma, infection, ischemia or neural damage, vascular defects, hyperpyrexia, teratogenic medications, and facial nevi [12]. In this case, however, no apparent etiology for RO was identified.
The criteria for diagnosis of RO are generally clinical and radiographic features, sometimes supported by histological findings [1]. Clinically affected teeth have an abnormal morphology with an irregular contour. The teeth are hypoplastic and hypocalcified, discolored to a yellowish or yellowish-brown [12,13]. The thin enamel is comparatively soft and susceptible to caries, and is highly susceptible to even mild trauma [13]. Tooth eruption is delayed or does not occur [12]. The most frequent clinical symptoms after eruption of teeth with RO are gingival swelling, periapical infection, or abscess formation without caries [4]. In the present case, the patient is currently showing early exfoliation of the right maxillary primary incisors, and delayed eruption of permanent incisors and the first molar. The patient has been followed-up periodically for the past 5 years. The right maxillary first molar has erupted into the oral cavity, and the surface is irregular and rough with yellowish-brown discoloration and hypoplastic and hypocalcified. Radiographically, there is no demarcation between the enamel and dentin on the affected side. The affected teeth show a“ ghostlike”appearance due to reduced thickness and radiodensity of the enamel and dentin [14,15]. The maxillary right central incisor and lateral incisor have short roots with wide-open apices which indicate delayed root development, whereas the root growth of the maxillary first molar is ongoing. Histopathological examination could not be performed in the present case because no teeth were extracted in our clinic. Histologically in RO, the enamel layer is typically hypoplastic and hypocalcified, with diverse thickness and the enamel prisms appear irregular in directions. Also, the dentin layer is diminished and usually contains a decreased quantity of tubules that are irregularly distributed, with broad interglobular and amorphous dentin areas, predentin layer enlargement, and clefts that can communicate between the pulp and oral cavity [16].
Other disorders that show some similarities to RO include amelogenesis imperfecta, dentinogenesis imperfecta, dentinal dysplasia types I and II, shell teeth, and hypophosphatasia. All of these anomalies tend to affect the entire dentition rather than showing only segmental involvement [17,18].
There has been controversy surrounding treatment of odontodysplasia. This condition is challenging and management usually requires a prolonged multidisciplinary approach. Consultations between pediatric, orthodontic, prosthodontic, and surgical specialists are necessary. Many clinicians suggest extracting the affected teeth as soon as possible and inserting a prosthetic appliance in their place, because the longer the affected teeth are retained, the higher the risk of development of pathologies like follicular cysts or odontogenic tumors [19,20]. On the other hand, some clinicians prefer to retain and conservatively manage these teeth until skeletal growth is complete as long as no infection is present. The non-infected teeth help maintain the alveolar bone, avert the use of a prosthesis, and eliminate the psychological stress of premature tooth loss [14,15]. However, the prognosis of the affected permanent teeth is usually poor. Because of this, in the future, extraction of permanent teeth and rehabilitation with dental implants or other types of prosthetic must be considered [12,13].
In the present case, the right maxillary first molar was treated preventively using topical fluoride, and stainless steel crown restoration is planned if necessary. The author, however, forewarned the parents of potential failure of root canal treatment, periapical infection, and the prospect of tooth extraction of the first molar due to a wide pulp cavity and hypoplastic enamel and dentin. The extraction of the right maxillary incisors, which show disrupted eruption, is being impeded by maintenance of alveolar bone, but the parents were notified of the possible need for extraction if pathologies such as follicular cysts or odontogenic tumors developed.
In the present case, the author confirmed the diagnosis of RO of the right maxillary dentition on the basis of the clinical and radiographic findings. The patient is currently under periodic recall to monitor the development of the affected teeth and dental arches and to preserve the affected teeth conservatively to minimize complications.
Ⅳ. Summary
This case report describes rarely reported features of RO, including involvement of teeth in the right maxilla in a male patient.
Since the teeth affected by RO are prone to developing periapical abscesses due to fragile tooth surfaces and open apices, preventive restoration therapy may aid in preserving the affected teeth, thereby maintaining the original shape of the alveolar bone. If extraction of the involved teeth is inevitable, a space maintainer should be implemented for functional and aesthetic purposes. Individual treatment plans are necessary, as treatment depends on whether teeth have erupted and the condition of the affected permanent successors. Therefore, long-term treatment strategies must be formulated after assessment of the status of the affected teeth through periodic clinical and radiological examinations.