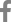Ⅰ. Introduction
Several systemic diseases involve congenitally missing teeth, such as ectodermal dysplasia, cleft, Rieger syndrome, Down’s syndrome and incontinentia pigmenti (IP). As both ectodermal dysplasia and IP arise from mutations in the NF-kappa-B essential modulator (NEMO) gene, they share similar congenital symptomatic clinical and dental manifestations such as missing or deformed teeth.
IP is a rare X-linked dominant disorder expressed in 1 in 40,000 females [1]. This genodermatosis affects females, but causes spontaneous abortion of prenatal males [2-5]. IP involves tissues and organs that originate from the ectoderm and mesoderm, including cutaneous tissue, hair, eyes, central nervous system and teeth [6,7].
Cutaneous manifestations of IP are common and occur in four phases. In addition to cutaneous manifestations, dental manifestation in patients with IP can be found with frequency, affecting both primary and permanent dentition [8]. Hypodontia is the most frequent dental abnormality and occurs in 43% of patients, followed by conical and pegged teeth [9-11].
This report described the dental treatment in three patients with IP based on clinical and radiological findings. We suggest that a valid treatment plan for patients with IP should be based on precise diagnosis by evaluating clinical and radiographic symptoms.
Ⅱ. Case Reports
1. Case 1
A 3-year-old female with IP visited the pediatric dentistry clinic due to lack of eruption. The patient’s 5-year-old sister (Case 2) also showed multiple congenitally missing teeth. Both of them were diagnosed as IP at the pediatric dentistry of Kyungpook National University Hospital. The patient had sparse hair and eyebrows as extraoral manifestations (Fig. 1). However, neither specific cutaneous manifestations nor systemic symptoms were apparent.
Oral examination revealed marginal alveolar resorption with congenitally missing teeth in the right maxillary first primary molar position and the right and left mandibular first and second primary molar positions. In addition, the patient had conically shaped primary canines in all four quadrants (Fig. 2). Radiographic examination showed that a total of 12 permanent teeth were missing, including the second molar and the first and second premolars in all four quadrants in the panoramic view (Fig. 3). Therefore, to resolve mastication and esthetic problems caused by multiple congenitally missing teeth, we applied removable space maintainer containing pontics of the missing primary molars (Fig. 4). After fitting the removable space maintainer, the patient received regular check-ups every 6 months for fluoride application and oral hygiene instruction for prevention of caries.
2. Case 2
A 5-year-old female (the sister of Case 1) visited the pediatric dentistry clinic because of unerupted teeth. Similar to Case 1, this patient was diagnosed with IP and had sparse hair and negligible eyebrows, but had no signs of systemic illness (Fig. 5).
Oral examination revealed marginal alveolar resorption and congenitally missing teeth in the positions of lateral primary incisors in all four quadrants, the left maxillary first primary molar, and the right and left mandibular first primary molars. In addition, the patient had conical-shaped primary canines (Fig. 6).
A panoramic radiograph confirmed the absence of multiple congenital permanent teeth. The patient had a total of 17 missing teeth: the lateral incisors and second molars in all four quadrants, the right maxillary first molar and canine, the left maxillary canine and first and second premolars, the left mandibular first molar and second premolar, and the right and left mandibular first premolars (Fig. 7).
As Case 2 had more missing primary teeth than Case 1, Case 2 had greater problems with mastication using primary molars and esthetic appearance. To restore masticatory and esthetic functions, removable space maintainers including pontics were applied on both the maxillary and mandibular primary molar areas (Fig. 8). After treatment using removable space maintainers, the patient received regular check-ups every 6 months for fluoride application and oral hygiene management. Prosthetic rehabilitation was planned upon completion of growth.
3. Case 3
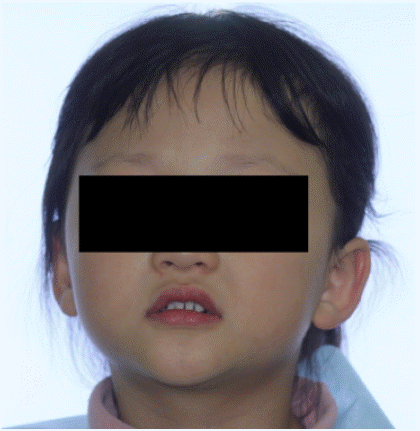
A 4-year-old female was seen at the pediatric dentistry clinic due to anterior cross bite and congenitally missing teeth. The patient was diagnosed with IP at the pediatric dentistry of Kyungpook National University Hospital and extraoral examination revealed features such as thin hair, scant eyebrows and mandibular prognathism (Fig. 9).
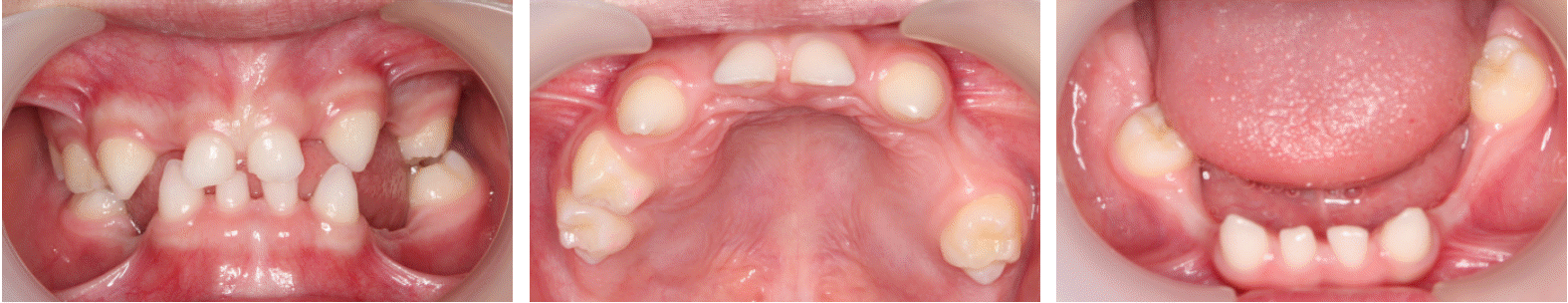
Oral examination revealed missing teeth in the right and left maxillary lateral incisors, left maxillary second primary molars, and left mandibular first and second primary molar positions. In addition, peg-shaped anterior teeth and enamel defects in the distal area of the left maxillary incisor were noted along with extrusion tendency of the left maxillary first primary molar due to the absence of an antagonistic mandibular primary molar(Fig. 10). Prosthetic restoration was expected to be complicated by the missing succedaneous permanent teeth that caused alveolar bone resorption in the left mandibular area. In addition, the patient had an esthetic issue due to an anterior cross bite.
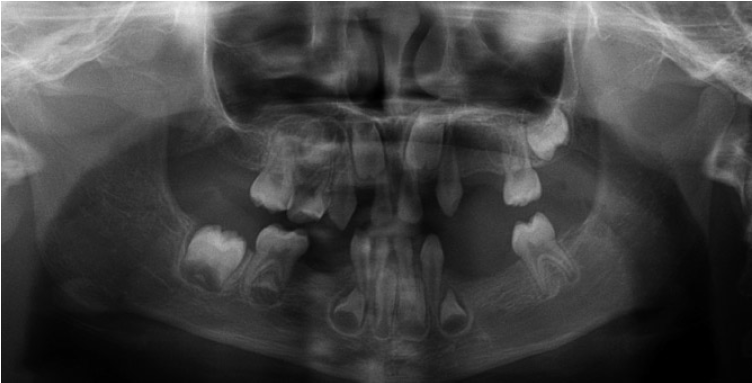
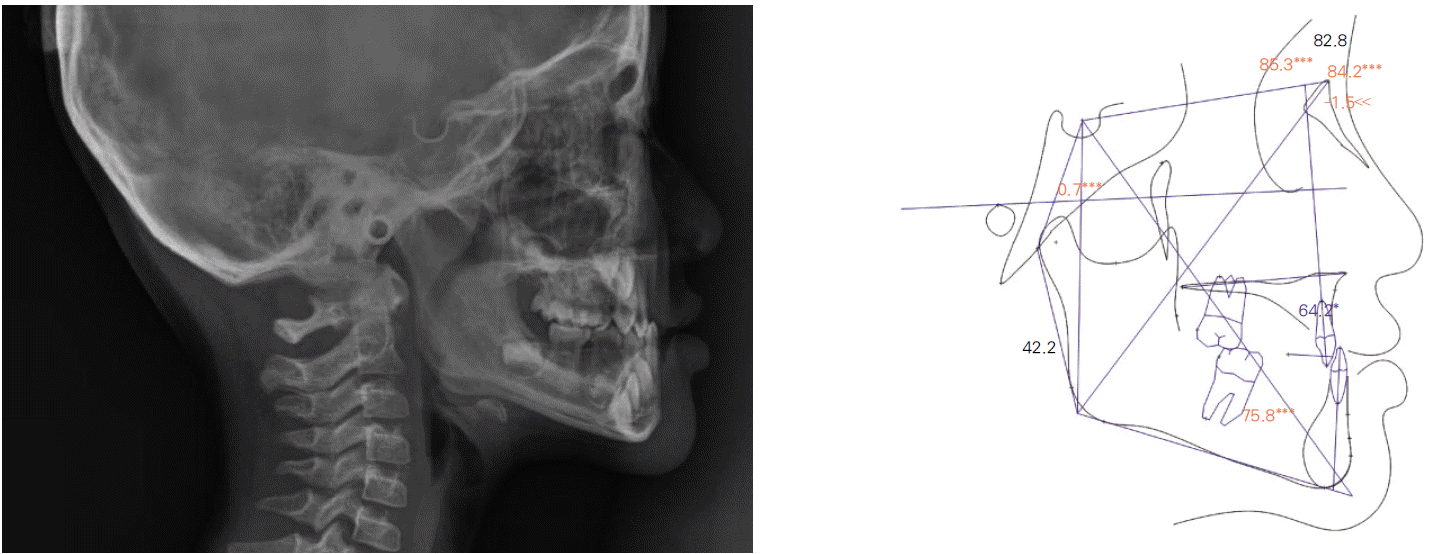
Panoramic radiograph revealed a total of 14 congenitally missing teeth: right and left maxillary second molars, first and second premolars, lateral incisors, right and left mandibular second molars and second premolars, and right mandibular first molar and first premolar teeth (Fig. 11). Lateral cephalogram and cephalometric analysis indicated anterior crossbite and mandibular prognathism (Table 1, Fig. 12).
In addition to esthetic issues, the patient required treatment for unilateral occlusion caused by congenitally missing teeth. To restore masticatory function, we applied a removable space maintainer with pontics. The design of the partial denture to restore occlusion was complicated by the fact that the patient suffered from an anterior crossbite and abnormal condition of the primary molars (Fig. 13). The patient received regular check-ups every 3 months.
Ⅲ. Discussion
IP, or Bloch-Sulzberger syndrome, was first reported by Garrod [12] in 1906. IP usually affects females, but causes spontaneous abortion of prenatal males.
IP is a disorder usually caused by a single gene mutation in the NEMO/IKK-γ gene [13,14] that results in a deletion of exons 4-10 in 60-88% of patients [15]. NEMO encodes a key regulator for growth factors such as cytokines, chemokines and adhesion molecules.
Cutaneous manifestation is a common IP symptom, which is classified into four stages: stage 1 (vesicles or inflammatory blisters), stage 2 (hyperkeratotic or verrucous lesions), stage 3 (brown and greyish blue hyperpigmentation) and stage 4 (cutaneous atrophy or hypopigmentation) [15-17].
Extracutaneous manifestations are expressed in 70-80% of patients with IP. Strabismus and cataracts are the most frequent manifestations in patients with ophthalmologic alteration [18-20] and may be accompanied by neurologic (cerebral atrophy, leukomalacia, mental retardation) and musculoskeletal (hemiatrophy, supernumerary ribs, short limbs) manifestations [21]. Dental manifestation is a typical noncutaneous manifestation of IP. In addition, patients with IP exhibit thin hair and nail dystrophy [22]. This study described three cases of IP with multiple congenitally missing or deformed teeth.
Both ectodermal dysplasia and IP arise by mutation in the NEMO gene and share similar symptomatic and dental manifestations, such as congenitally missing and deformed teeth. However, IP is caused by amorphic mutations in the NEMO gene that suppress protein synthesis, whereas ectodermal dysplasia results from hypomorphic mutations in NEMO that do not remove its entire function. The majority of ectodermal dysplasia cases are autosomal recessive disorders that occur more frequently in males. On the other hand, IP is an X-linked dominant disease that affects females. The dental manifestations of IP and ectodermal dysplasia are similar, and a thorough differential diagnosis is required.
Patients with ectodermal dysplasia have fine dry skin due to sweat gland deficiency, while patients with IP have cutaneous manifestations and other systemic symptoms. Genetic analysis is considered essential for accuracy in differential diagnosis [23]. When patients with multiple congenitally missing teeth visit the clinic, the possibility of various systemic diseases must be considered with respect to the specific medical history.
Multiple congenitally missing teeth in IP may cause psychological problems from an esthetic viewpoint in addition to causing problems in mastication and occlusion.
Teeth stimulate local bone growth by working as a functional unit. Thus, patients with congenitally missing teeth show underdevelopment in jaw growth, which is more severe in the maxilla compared to the mandible. Moreover, when congenitally missing teeth occur in the molar area, the lower face can suffer from underdevelopment due to the lack of occlusal support and crossbite caused by lower jaw prognathism.
The influence on jaw growth is greater when teeth are missing from posterior vs. anterior regions. In IP patients, growth may accompany mandibular prognathism and crossbite. In previous reports, oral hygiene management and space maintainers were applied to IP patients to resolve spacing problems. Whenever pediatric dentists observe facial skeletal growth and commensurate profile changes, congenitally missing teeth should be considered, with space-maintaining and prosthetic treatment applied using regular extraoral photographs and cepholgrams. Cenk et al. [24] studied an IP patient with multiple missing and malpositioned teeth. A rapid palatal expansion (RPE) was initially applied, with prosthetic restoration following the alignment of malpositioned residual teeth. Yamashiro et al. [25] reported on an IP patient suffering from a Class III malocclusion and malpositioned teeth; excessive preparation was avoided by applying orthodontic treatment prior to prosthetic restoration.
Therefore, in addition to regular check-ups, maintenance of proper spacing and occlusion restoration are required for recovery of both occlusion and esthetic function. Upon completion of growth, permanent restoration should be considered by applying prosthodontic and orthodontic treatment.
Ⅳ. Summary
IP is accompanied commonly by cutaneous and dental manifestations, such as congenitally missing teeth, tooth-shape deformities, and delayed eruption. Patients in this study showed multiple congenitally missing teeth in both primary and permanent dentition and conically shaped supernumerary cusps in the anterior and posterior areas. The patients in this study were treated by applying a removable space-maintaining device in the vacant areas to maintain proper spacing and restore masticatory function. The patients received regular post-operative check-ups and oral hygiene management. Prosthodontic and orthodontic treatment should be considered upon completion of permanent dentition.











 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print