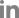|
 |
| J Korean Acad Pediatr Dent > Volume 44(3); 2017 > Article |
|
초록
본 연구는 Molar-incisor hypomineralization(MIH)에 이환된 제1대구치를 그 결손의 크기 별로 분류를 시행하고, 수복치료 후 수복재료에 따른 예후 평가를 목적으로 수행되었다.
MIH에 이환되어 맹출 후 치관 붕괴가 관찰된 제1대구치를 Class Ⅰ에서 Ⅲ까지 세 단계로 분류하고, 수복치료 이후 수행된 재치료 빈도를 Class와 수복재료별로 나누어 살펴보았다. MIH Class Ⅰ결손에서는 실런트, Class Ⅱ 결손에서는 복합레진이 가장 높은 유지율을 보였다. Class Ⅲ 결손에서는 기성금속관의 유지율이 가장 높게 나타났다.
Abstract
The objectives of this study were to classify the first permanent molars showing molar-incisor hypomineralization (MIH) on the basis of defect size and to assess differences in the prognoses of restorations performed with different materials.
The first permanent molars with MIH and posteruptive breakdown were categorized into MIH class I, II, and III. After performing restorations, retreatment frequencies were examined according to the defect class and initial restorative material used. Sealants, composite resins, and stainless steel crowns showed the highest survival rates in cases of MIH class I, II, and III defects, respectively.
Molar-incisor hypomineralization (MIH) is a clinical condition that was first defined in 2001. MIH is a defect with a systemic etiology that affects one or more first permanent molars or one-third of the occlusal surface or incisal edge of incisors, and is defined on the basis of the clinical appearance or presence of morphological defects[1]. MIH clinically presents as soft and porous tooth enamel with clearly demarcated opacities. Furthermore, tooth brushing or masticatory forces could induce structural defects, which can occur posteruptive breakdown and can increase the sensitivity of teeth to external stimuli[2,3].
It is thought that MIH is not caused by a single specific condition. The medical complications including respiratory disorders and fever may increase the risk of MIH occurence[4-7]. Although the causative factor of MIH has not been clearly identified, genetic factors and correlation with hypomineralization of the second primary molar have been recently implicated[8,9].
The prevalence of MIH has been reported to range from 2.4% to 40.2%[10-12]. This variation of MIH prevalence may be attributed to differences in subject inclusion criteria, diagnostic categories for the disease, and methodologies.
Depending on the patient’s age, cooperation, eruption status and severity of structural defect, the treatment of MIH can range from preventive treatment to restoration and extraction[6]. However, the treatment of MIH is characteristically associated with several clinical difficulties, including the hypersensitivity caused by MIH, rapid caries progression due to tooth structure breakdown and poor cooperation from young pediatric patients. Furthermore, achieving adequate anesthesia is a challenge, and tooth fracture repeatedly recurs even after restoration[13].
The range and severity of MIH may influence the choice of restorative material and prognosis of treatment. Thus, the classification of MIH to mild, moderate, and severe stages of severity was suggested by Mathu-Muju and Wright[14]. In this classification, previous studies suggested that for mild MIH, preventive treatment should be performed or composite resins (CRs) should be used to restore the defects. For moderate/severe MIH, restorations should be performed with glass ionomer cement (GIC) for partially erupted teeth and CRs for teeth with three or fewer affected surfaces. Restorations with a stainless steel crown (SSCr) or extraction should be performed for more severe defects[15-19]. It was showed that the treatment of MIH-affected first molars could involve various restorative materials depending on the severity and range of the defect, patient cooperation and eruption stages of the teeth. Therefore, restorative materials should be differentially chosen according to the extension and severity of the defects. However, only few studies have been reported and for this reason, there are limited prognostic information regarding degrees of MIH defect with restorative materials.
Therefore, this present study attempted to classify the range of defects of MIH-affected first molars and examines the prognoses of restorative treatment with different restorative materials in order to provide clinically useful information for treating MIH-affected first molar.
Pediatric patients who had been diagnosed as having MIH via clinical examination and radiography, received treatment for MIH between 2007 and 2015 at Department of Pediatric Dentistry, Kyungpook National University Dental Hospital, and were followed-up for a minimum of 12 months were recruited for this study. Among these patients, 53 who met the inclusion criteria (Table 1) were finally selected for this study. The mean age of the patients was 6.6 years. Assessments of the severity of structural defects, treatment methods, and prognosis of the restorations over time were performed for 158 MIH-affected first molars by analyzing the patients’ electronic dental records, radiographs, and clinical photographs.
The MIH-affected first molars were assessed using radiographs and clinical photographs, and were classified according to the severity and location of the defect (Fig. 1). The defects were classified into one of the following 3 classes, with reference to the method suggested by Mathu-Muju and Wright[14]: (1) MIH class I (mild MIH), opacities with clearly demarcated non-stress-bearing areas and no cavities or enamel defects; (2) MIH class II (moderate MIH), disintegration of hypomineralized enamel or cavity limited to 1 or 2 tooth surfaces excluding the cusps; (3) MIH class III (severe MIH), posteruptive enamel breakdown occurring simultaneously with tooth eruption and an extensive cavity or crown fracture involving the pulp.
The ages of the subjects who were followed up for at least 12 months and the restorative materials used for first molar restorations were surveyed. In addition, the number of retreatments after the initial restoration and the prognosis was investigated to examine the differences in prognoses according to the restorative materials used.
Restorative material-specific survival rates depending on the classification of tooth defects were assessed by using the log-rank test. The Kaplan-Meier test was performed to assess the 24-month survival rate of restorations prepared with each restorative material. All statistical analyses were performed using SPSS for Windows Version 12.0 (SPSS Inc., Chicago, IL, USA), and the results were assessed at a significance level of p < 0.05.
The MIH-affected first molars were classified as the MIH classification method. Of the 158 MIH-affected teeth, 24 (15.2%) were classified as MIH class I; 54 (34.2%), MIH class II; and 80 (50.6%), MIH class III (Table 2). No significant differences were found in the prevalence of MIH between the left or right sides, or between the maxillary or mandibular first molars.
The restorative materials chosen for the initial restoration of MIH-affected teeth were investigated according to MIH class. Among the 24 teeth with MIH class I defects, 14 (58.3%) received preventive treatment with sealants, while 2 (8.3%) were followed-up with fluoride application. In addition, 2 (8.3%) and 6 (25.0%) teeth were restored with CR and GIC, respectively, after the removal of weak tooth structures. Among the 54 teeth with MIH class II defects, 19 (35.2%) were restored with CR, while 33 (61.1%) were restored with GIC. Sealants were applied in 1 (1.8%) case, and defects were restored with SSCr in another (1.8%). Among the 80 teeth with MIH class III defects, restoration was performed with CR, GIC, and SSCr in 19 (23.8%), 56 (70.0%), and 5 (6.5%) teeth, respectively (Table 3).
The retreatments performed after the initial restorative treatment of the MIH-affected teeth were examined, and the following features were assessed: MIH class, number of teeth subjected to retreatment, material-specific 24-month survival rate, material used for retreatment, average period until retreatment, presence of pulp morbidity, and length of follow-up (Table 4).
Among the teeth with MIH class I defects, 2 were followed up with fluoride application only, and both were restored with CR or GIC within 21 months. Sealants were applied in 14 teeth, of which 12 (85.7%) were maintained during the study period, while 2 (14.3%) required restorative treatment. CR and GIC were used for the initial restoration in 2 and 6 teeth, respectively. Retreatment was performed in both the teeth initially restored with CR and in 4 of the 6 (66.6%) teeth initially restored with GIC. The Kaplan-Meier test revealed that the 24-month survival rate was 74.3% for sealants, 50% for CR, and 40% for GIC. The log-rank test verified statistically significant differences in survival rate for the restorative materials chosen for the teeth with MIH class I defects (p= 0.046).
Among the 18 teeth with MIH class II defects, 5 (27.8%) of those restored with CR were retreated at an average of 19.2 months. The 4 of these retreated teeth were restored with CR, while one of them was restored with SSCr. The 19 (57.6%) of the 33 teeth initially restored with GIC were retreated at an average of 11.8 months, and all of them except 1 tooth were restored with GIC again. One tooth was initially restored with SSCr and was not retreated. The 24-month survival rates for CR and GIC were 76.6% and 47.8%, respectively, and the difference was statistically significant (p= 0.036). One tooth that was initially treated with sealants was restored with GIC within 8 months.
Among the teeth with MIH class III defects initially restored with CR, GIC, and SSCr, retreatment was performed in 12 or 19 (63.2%), 37 of 56 (66.1%), and 1 of 5 (20%), respectively, within an average of 16.2 months, 12.4 months, and 1 month, respectively. Retreatment was performed for the tooth restored with SSCr because the patient had bite discomfort. The 24-month survival rate was 54.1% for CR, 40.2% for GIC, and 75.0% for SSCr, but the differences were not statistically significant (p= 0.2). In terms of the materials chosen for retreatment, the trend was towards choosing the same material used for the initial restoration.
The 6 teeth with MIH class III defects were subjected to root canal treatment for pulp morbidity that occurred after restorative treatment for MIH-affected first molars. Of these teeth, 5 were initially restored with GIC.
The retreatment rate, average retreatment frequency of each retreatment case, mean and median survival rates, and 24-month survival rate were assessed for each restorative material. All the restorative materials initially required retreatment. Restoration was performed in the 2 teeth that were followed-up with fluoride application. The 3 of the 15 teeth that were treated with sealants were also retreated, showing a 24-month survival rate of 86.7%. The most frequently chosen materials for the initial restoration were CR and GIC, and their mean retreatment frequencies were 0.75 and 1.20, respectively. The median 24-month survival rates with CR and GIC were 34.0 and 18.0 months, respectively. The 24-month survival rates were highest with 86.7% for sealants and 83.3% for SSCr, followed by 57.1% for CR and 46.6% for GIC, all of which were statistically significant (Table 5).
The present study classified the MIH-affected first permanent molars into different classes of severity and assessed the prognoses of restorations.
The selection and long-term stability of restorative material is a subject of controversy for MIH-affected first molars. Some previous studies have been reported that CR shows satisfactory treatment results[17-19], but showed limitation of not assesses the prognoses in accordance with the severity of defects.
The severity of MIH has been classified in a previous study[20]. However, because the severity index was only divided into 2 classes, the effectiveness of assessing retreatment and the correlation between the severity of the defect and the choice of restorative material have been limited. In contrast, Mathu-Muju and Wright[14] classified MIH into the mild, moderate, and severe classes depending on the severity of the defect, and recommended treatment modalities for each MIH class. However, the prognoses of the suggested treatment modalities were not assessed. Therefore, the present study assessed the prognoses of restorations in accordance with the severity of MIH-affected first molars into class I, II, or III, and investigated the survival rates of restorations as well as the retreatment frequency (Table 2, Fig. 1).
Results of the present study is consistent with those of the previous study which CR restorations had a significantly high survival rate and low risk of retreatment when used for MIH class I and II defects. However, CR restorations were associated with an increased risk of retreatment when used for MIH class III defects, but it was not statistically significant.
The 24 teeth were classified into MIH class I, for which the initial treatment included fluoride application, sealants, CR and GIC restoration as shown in Table 4. Sealants were chosen most with class I defects, and 85.7% of the restorations survived during the study period. Furthermore, sealants showed the highest statistically significant survival rate with MIH class I defects, indicating that sealant resulted in a good prognosis for MIH class I defects. However, some MIH class I teeth required restorative treatment because of the breakdown of hypomineralized areas, and retreatment was performed with alternative material. Therefore, the teeth classified into the MIH class I required continuous follow-up, as it is necessary with other classes of defects.
The majority of MIH class II defects were treated by using CR, GIC, and SSCr. The CR had a significantly lower risk of retreatment and a higher 24-month survival rates. Furthermore, the average periods until first retreatment were 19.2 and 11.8 months for CR and GIC, respectively. Overall results showed that CR restoration had the best prognosis for MIH class II.
In MIH class III defects, the retreatment ratio for CR restorations increased to 63.2%, and the 24-month survival rate decreased to 54.1%. In contrast, the retreatment ratio and 24-month survival rate for GIC restorations did not differ significantly from those of the MIH class II. These results imply that the range of the defect is a greater impact factor on the prognosis of the restoration than does the choice of restorative material for MIH class III defects. Although restorations with SSCr were performed on a relatively fewer number of teeth, it showed the best prognosis, with a 24-month survival rate of 75% in MIH class III. Furthermore, 5 teeth were retreated with SSCr, and these required no additional retreatments. This finding supported the recommendations to use SSCr for defects that affect 3 or more tooth surfaces[15,16].
The frequency of retreatment was assessed with each material (Table 5). The proportion of cases requiring retreatment was 47.5% for CR, 63% for GIC, and 16.7% for SSCr. In addition, the frequency of retreatment was greatest in restorations with GIC, with an average of 1.20 retreatments in each tooth. The median survival time was 34 months for CR and 18 months for GIC, showing that CR were retained longer than GIC. CR had a significantly high the median survival time and 83.3% of SSCr survived for 24-months. These results supported the findings of previous studies that consistently suggested better prognosis with CR and SSCr.
Interestingly, root canal treatment was performed for postrestoration pulpal complications in 6 teeth with class III defects (Table 4). However, no correlation was found between retreatment frequency and pulpal involvement (data not shown). Thus, it could be speculated that the proximity of the defect to the pulp has a greater impact than retreatment frequency, but additional studies would be needed to substantiate this.
A distinct finding of this study was the numerous choices of GIC for MIH-affected first permanent molars, influenced by the personal preferences of dental clinicians. The preference of GIC could be affected by several factors, including partial eruption, low patient cooperation, uncertain adhesiveness of CR, short treatment time, and tooth sensitivity, treatment cost and etc. Notwithstanding the high choice of GIC, CR showed a greater survival rate in all classes of defects. These findings once again showed the similarity to the validity of Mathu-Muju and Wright’s[14] recommendation of the use of CR for the treatment of MIH-affected first permanent molars.
In conclusion, Fig. 2 illustrates a treatment protocol that takes into account the range of defects, symptoms and patient cooperation during the treatment of the first permanent molars affected by MIH. First, the MIH-affected first permanent are identified. For firm hypomineralized enamel without enamel defects, sealants are applied, while for soft hypomineralized enamel, restoration after the removal of the hypomineralized area is recommended. CR restoration is performed for defects limited to less than 2 tooth surfaces; this restoration is also recommended if the defects are observed on more than 2 tooth surfaces, provided the eruption of the first permanent molar is complete, and the removal of the entire hypomineralized enamel area is possible. However, if the removal of the entire hypomineralized enamel is not possible because of extensive structural defects, SSCr is recommended as the initial restoration. If defects are present on more than 2 tooth surfaces and the tooth is partially erupted, GIC restoration, which is later replaced with SSCr or CR restoration, may be considered depending on the pediatric patient’s ability to cooperate. For cooperative pediatric patients, SSCr or CR is recommended for the initial restoration. Higher treatment success rates may be achieved by following this protocol.
Although many previous studies have recommended SSCr for restoring class III defects, only limited data on the long-term prognoses of SSCr restorations are available, thus the need for further long-term studies essential on this subject. Furthermore, limitations of this study includes that the range of defects classified as MIH class III is broad in a measure. Though future studies, further clinical implications of various restorative materials could be revealed by assessing the prognosis of restorations in accordance with subdivided the MIH class III.
This study classified the MIH-affected first permanent molars into classes I, II, and III, and assessed the prognoses of restorations performed in each group. Sealants showed the highest survival rate for teeth with MIH class I defects, CR restorations for teeth with MIH class II defects, and SSCr restorations for teeth with MIH class III defects. However, as SSCr restorations cannot be performed immediately for partially erupted teeth even when indicated, provisional GIC restorations should be performed first and replaced with SSCr restorations.
Fig. 1.
Classification of teeth affected with MIH. (A, B) Periapical and clinical views representing MIH class I defects, showing opacities with clearly demarcated non-stress-bearing areas and no cavities or enamel defects. (C, D) MIH class II defects, showing the disintegration of hypomineralized enamel or cavity limited to 1 or 2 tooth surfaces excluding the cusps. (E, F, G, H) MIH class Ⅲ defects, showing posteruptive enamel breakdown occurring simultaneously with tooth eruption and an extensive cavity or crown fracture involving the pulp.
Fig. 2.
Treatment protocol for MIH-affected teeth. Sealant = resin sealant; CR = composite resin; GIC = resin-reinforced glass ionomer cement; SSCr = stainless steel crown.
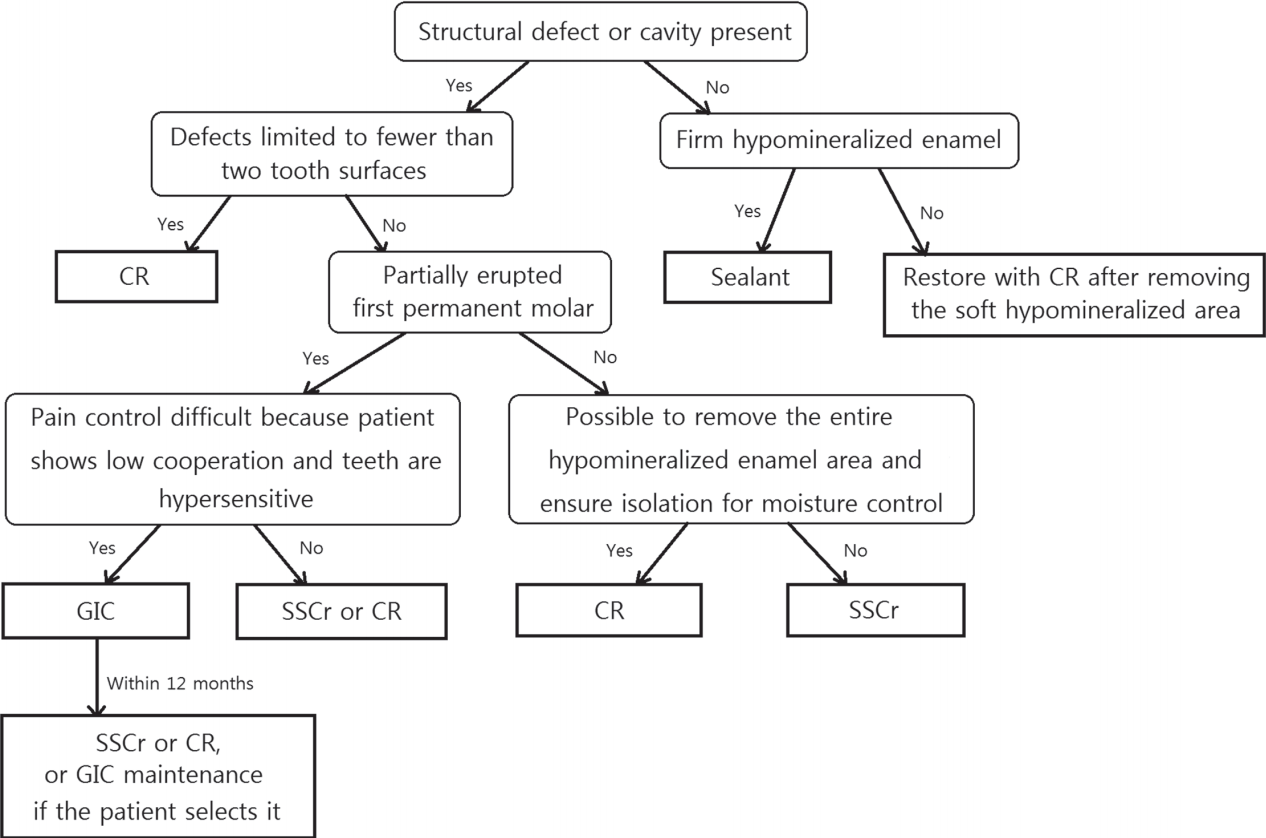
Table 1.
Patients diagnosed with MIH by age and sex
| Age (yr) | Male | Female | Total |
|---|---|---|---|
| 5 | 3 | 1 | 4 |
| 6 | 8 | 11 | 19 |
| 7 | 12 | 6 | 18 |
| 8 | 6 | 2 | 8 |
| 9 | 1 | 1 | 2 |
| 10 | 1 | 1 | 2 |
|
|
|||
| Total | 31 | 22 | 53 |
Table 2.
Class distribution of the MIH-affected first permanent molar
| MIH Class | |||||
|---|---|---|---|---|---|
| Ⅰ | Ⅱ | Ⅲ | Total n (%) | ||
| Maxilla | Right | 11 | 9 | 18 | 38 (24.1) |
| Left | 7 | 13 | 18 | 38 (24.1) | |
| Mandible | Right | 3 | 15 | 24 | 42 (26.6) |
| Left | 3 | 17 | 20 | 40 (25.2) | |
|
|
|||||
| Total, n (%) | 24 (15.2) | 54 (34.2) | 80 (50.6) | 158 (100) | |
Table 3.
Association between MIH classes and the initial restorative material
Table 4.
Frequency of retreatment in each MIH class after restoration
| MIH Classes | Initial Restorative Materials, n | Retreatment not Required n (%) |
Retreatment Required |
Follow-up Time, Average Month | Retreatment Frequency, (SD) | |||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Total n (%) | † 24-Month Survival Rate | ‡ p value | Retreatment Material | n | Root Canal Treatment Involved, n | Duration to First Retreatment | ||||||
| Class Ⅰ | Fluoride | 2 | 0 | 2 (100) | 0 | 0.046* | CR | 1 | 0 | 21 | 37.1 | 0.67 (0.87) |
| GIC | 1 | |||||||||||
|
|
|
|||||||||||
| Sealant | 14 | 12 (85.7) | 2 (14.3) | 74.3 | CR | 1 | 0 | 16 | ||||
| GIC | 1 | |||||||||||
|
|
|
|||||||||||
| CR | 2 | 0 | 2 (100) | 50 | CR | 1 | 0 | 9.5 | ||||
| GIC | 1 | |||||||||||
|
|
|
|||||||||||
| GIC | 6 | 2 (33.3) | 4 (66.6) | 40 | CR | 1 | 0 | 13.5 | ||||
| GIC | 3 | |||||||||||
|
|
||||||||||||
| Class Ⅱ | Sealant | 1 | 0 | 1 (100) | 0 | 0.036* | GIC | 1 | 0 | 8 | 33.6 | 0.72 (1.05) |
|
|
|
|||||||||||
| CR | 18 | 13 (72.2) | 5 (27.8) | 76.6 | CR | 4 | 0 | 19.2 | ||||
| SSCr | 1 | |||||||||||
|
|
|
|||||||||||
| GIC | 33 | 14 (42.4) | 19 (57.6) | 47.8 | CR | 1 | 0 | 11.8 | ||||
| GIC | 18 | |||||||||||
|
|
|
|||||||||||
| SSCr | 1 | 1 (100) | 0 | 100 | 0 | |||||||
|
|
||||||||||||
| Class Ⅲ | CR | 19 | 7 (36.8) | 12 (63.2) | 54.1 | 0.2 | CR | 6 | 1 | 16.2 | 31.6 | 1.22 (1.35) |
| GIC | 2 | |||||||||||
| SSCr | 2 | |||||||||||
|
|
|
|||||||||||
| GIC | 56 | 19 (33.9) | 37 (66.1) | 40.2 | CR | 7 | 5 | 12.4 | ||||
| GIC | 26 | |||||||||||
| SSCr | 3 | |||||||||||
|
|
|
|||||||||||
| SSCr | 5 | 4 (80.0) | 1 (20) | 75.0 | SSCr | 1 | 0 | 1 | ||||
Table 5.
Pattern of retreatment with each restorative material
| Restorative Material | Total, n | Retreatment, n (%) | Retreatment Frequency | Mean Survival Time | Median Survival Time | † 24-month Survival Rate | ‡ p value | ||
|---|---|---|---|---|---|---|---|---|---|
| Estimate | Standard Error | Estimate | Standard Error | ||||||
| Fluoride | 2 | 2 (100) | 2 | 21.00 | 9.00 | 12.00 | . | 50.0 | 0.02* |
| Sealant | 15 | 3 (20.0) | 0.27 | 50.35 | 6.92 | . | . | 86.7 | |
| CR | 40 | 19 (47.5) | 0.75 | 38.72 | 5.01 | 34.00 | 6.25 | 57.1 | |
| GIC | 95 | 60 (63.2) | 1.20 | 36.12 | 4.90 | 18.00 | 4.14 | 46.6 | |
| SSCr | 6 | 1 (16.7) | 0.17 | 37.67 | 6.69 | . | . | 83.3 | |
|
|
|||||||||
| Total | 158 | 85 | 0.97 | 43.07 | 4.53 | 26.00 | 3.38 | ||
References
1. Weerheijm KL, Jälevik B, Alaluusua S : Molar-Incisor Hypomineralisation. Caries Res, 35:390-391, 2001.


3. Allazzam SM, Alaki SM, Meligy OA : Molar Incisor Hypomineralization, Prevalence, and Etiology. Int J Dent, 2014:1-8, 2014.


4. Lygidakis NA, Dimou G, Marinou D : Molar-Incisor Hypomineralisation (MIH). A retrospective clinical study in Greek children. Ⅱ. Possible medical aetiological factors. Eur Arch Paediatr Dent, 9:207-217, 2008.


5. Laisi S, Ess A, Alaluusua S, et al. : Amoxicillin may cause molar incisor hypomineralization. J Dent Res, 88:132-136, 2009.


6. Lygidakis NA, Wong F, Espelid I, et al. : Best clinical practice guidance for clinicians dealing with children presenting with molar-incisor-hypomineralisation (MIH). Eur Arch Paediatr Dent, 11:75-81, 2010.


7. Tourino LF, Corrêa-Faria P, Vale MP, et al. : Association between Molar Incisor Hypomineralization in Schoolchildren and Both Prenatal and Postnatal Factors: A Population-Based Study. PLoS One, 9:11-22, 2016.

8. Mittal R, Chandak S, Pimpale J, et al. : Assessment of association between molar incisor hypomineralization and hypomineralized second primary molar. J Int Soc Prev Community Dent, 6:34-39, 2016.



9. Oyedele TA, Folayan MO, Oziegbe EO : Hypomineralised second primary molars: prevalence, pattern and associated co morbidities in 8- to 10-year-old children in Ile-Ife, Nigeria. BMC Oral Health, 16:65-71, 2016.



10. Koch G, Hallonsten AL, Ullbro C, et al . : Epidemiologic study of idiopathic enamel hypomineralization in permanent teeth of Swedish children. Community Dent Oral Epidemiol, 15:279-285, 1987.


11. Jälevik B, Klingberg G, Barregård L, Norén JG : The prevalence of demarcated opacities in permanent first molars in a group of Swedish children. Acta Odontol Scand, 59:255-260, 2001.


12. Shin JH, An UJ, Kim S, Jeong TS : The prevalence of molar incisor hypomineralization and status of first molars in primary school children. J Korean Acad Pediatr Dent, 37:179-185, 2010.
13. William V, Messer LB, Burrow MF : Molar Incisor Hypomineralization: review and recommendations for clinical management. Pediatr Dent, 28:224-232, 2006.

14. Mathu-Muju K, Wright JT : Diagnosis and treatment of molar incisor hypomineralisation. Compend Contin Educ Dent, 27:604-610, 2006.

15. Lygidakis NA : Treatment modalities in children with teeth affected by molar-incisor enamel hypomineralisation (MIH): A systemic review. Eur Arch Paediatr Dent, 11:65-74, 2010.


16. Zagdwon AM, Fayle SA, Pollard MA : A prospective clinical trial comparing preformed metal crowns and cast restorations for defective first permanent molars. Eur Arch Paediatr Dent, 4:138-142, 2003.
17. Lygidakis NA, Chaliasou A, Siounas G : Evaluation of composite restorations in hypomineralised permanent molars: a four-year clinical trial. Eur Arch Paediatr Dent, 4:143-148, 2003.
18. Mejare I, Bergman E, Grindefjord M : Hypomineralized molars and incisors of unknown origin: treatment outcome at age 18 years. Int J Paediatr Dent, 15:20-28, 2005.


19. Kotsanos N, Kaklamanos EG, Arapostathis K : Treatement management of first permanent molars in children with Molar-incisor Hypomineralisation. Eur Arch Paediatr Dent, 6:179-184, 2005.
- TOOLS
-
METRICS

-
- 4 Crossref
- 0 Scopus
- 4,716 View
- 187 Download
- Related articles



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print