소아에서 나타나는 흑색 착색에 대한 에센셜 오일 함유 가글액의 효과 : 증례 보고
Effects of Essential Oil Containing Mouth Rinse in Children with Black Staining : Two Case Reports
Article information
Abstract
소아 및 청소년의 치면의 흑색 착색은 통증이나 심각한 병적 상태를 유발하지 않지만 심미적인 단점으로 인해 환자가 사회적으로 위축되게 한다. 흑색 착색은 주기적인 전문가 치면세균막 관리 및 스케일링을 통해 쉽게 제거되나 수개월 이내에 재발하는 문제가 있다. 50%로 희석한 에센셜 오일 함유 가글액을 하루 2회씩 사용하는 것은 흑색 착색이 제거된 뒤에 재발하는 것을 예방할 수 있으며 이를 통해 처치의 빈도를 줄이면서 심미성을 개선할 수 있다.
Trans Abstract
Black staining of the teeth in children and adolescents does not cause pain or serious illness, but it can be socially debilitating for esthetic reasons. Black staining is easily removed through periodic professional mechanical tooth cleaning and ultrasonic scaling, but it can easily recur within few months. Using essential oil-containing mouth rinses diluted at 50% twice per day could prevent the black staining from returning after it is removed, reducing the need for mechanical treatments and improving esthetics.
Ⅰ. Introduction
Black staining (BS) can cause social problems. It can occur at any age, but it is most common in preschool-aged children[1]. BS is black and conspicuous, so children with BS have esthetic concerns when they smile or expose their teeth. It is hard to remove through tooth-brushing because of its sticky, hard and insoluble properties, and relatively frequent professional mechanical tooth cleaning (PMTC) or scaling by a dental professional is required because it easily recurs within few months.
The prevalence rate of BS is 6.17 - 14.8% and it varies by country and age[1]. It is extrinsic discoloration and occurs most frequently in prepubertal children. BS is different from intrinsic discoloration in that it accumulates on acquired pellicle. It appears mostly on the cervical third of the tooth’s smooth surface, parallel to the marginal gingiva and the proximal area[2]. It begins as black dots and becomes dotted lines or half-circles. Only rarely does it cover more than half of the tooth surface, but it always begins in the cervical area where dental plaque is easily accumulated.
The etiology of BS is still unclear, but iron consumption and bacterial colony from dental plaque are positively correlated with BS[3]. Iron in drinking water, medicines that contain ferric salts, and frequent consumption of iron-rich food are considered to be the main causes of BS[4]. Hydrogen sulfide from chromogenic gram-positive bacteria from dental plaque have an important etiological role in BS formation because they chemically react with iron in oral cavity[5]. Hypothesis that BS originates from dental plaque also can be accepted, because BS and dental plaque occur in the same areas.
The American Dental Association approved the use of essential oils to treat supragingival plaque[6]. Its anti-plaque effect was also proved through clinical study[7]. Thus, it was hypothesized that essential oils could be used to treat BS because BS forms on top of plaque. Assuming reduced plaque has positive relation with relief of symptoms, two patients with BS were prescribed with essential oil-containing mouth rinses to determine whether they could reduce BS. Past studies had focused on the etiology and microbial composition of BS rather than its solution. Its esthetic problems cause patient’s social problems, so there is a need for a simple in-home therapy.
Ⅱ. Case Reports
1. Case 1
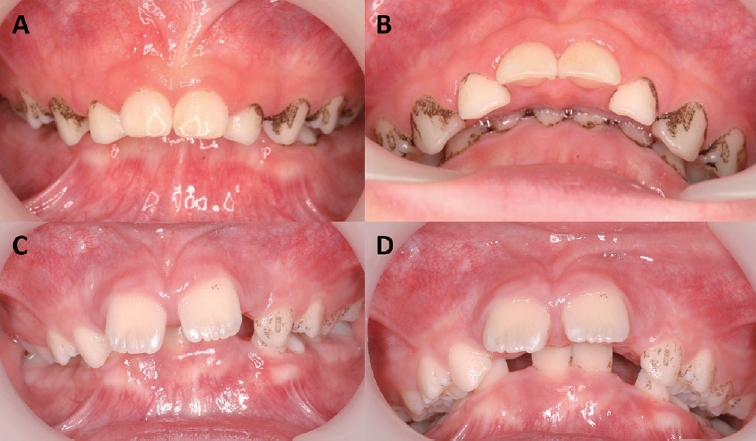
A four-year-old boy visited the Department of Pediatric Dentistry in Yonsei University Dental Hospital with the chief complaint of black staining. He had no remarkable medical or dental history. Clinical and radiological examinations did not reveal any problems requiring treatment except for BS. He had fully deciduous dentition and BS on all of his teeth. The cervical thirds of both the buccal and lingual sides were covered with BS. The proximal area near the gingival papilla were particularly severe (Fig. 1A). The patient did not have any dietary problems, oral hygiene problems, or halitosis. The patient was not in pain, but he had social problems due to the esthetics of his condition. The BS was difficult to remove with PMTC, so ultrasonic and hand scaling were conducted at the same time. After the BS was removed, his teeth were polished. The same process was repeated four months later, at his second visit because the BS had recurred during that time (Fig. 1B). Considering the patient’s characteristics, essential oil-containing mouth rinse (Listerine Total Care Mild, Pfizer, New York, NY, USA) was prescribed to the patient. Purified water was used to dilute the mouth rinse by 50%. The mouth rinse was prescribed to be used twice per day for 30 seconds in the morning and evening after thorough tooth brushing. The parents were trained to stop him using essential oil-containing gargle if he feels burning sensation or often swallows it unintentionally. Four months later, the patient came in for his third visit, and at this time, little BS had recurred such that mechanical removal was not required (Fig. 1C). The patient and his parents were satisfied with this result, so the same mouth rinse regimen was prescribed until another visit in four months. The BS had not progressed by the fourth visit and again no mechanical removal was required (Fig. 1D).
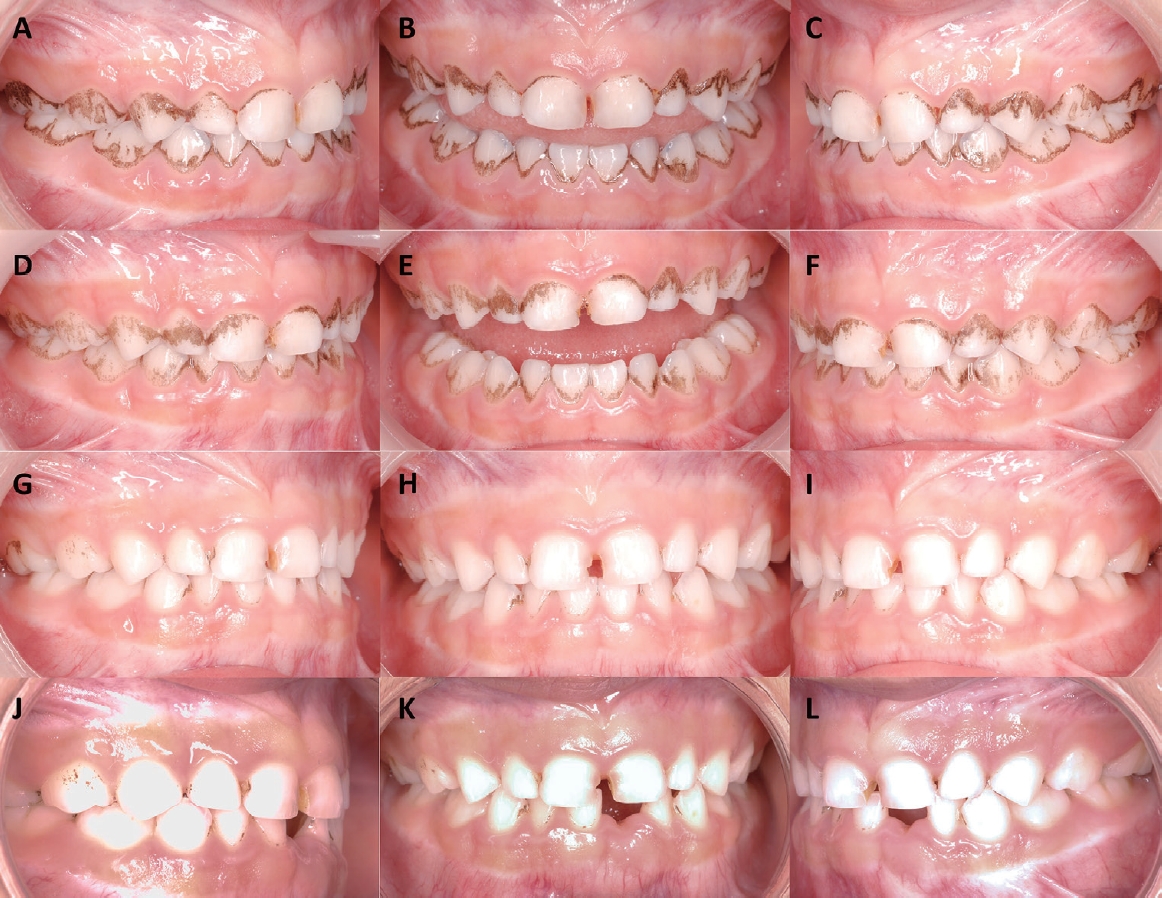
Clinical intra-oral photos of the patient in case 1. All photos were taken before BS removal. (A, B, C) Photos taken before PMTC at the first visit. (D, E, F) Photos taken before PMTC at the second visit, which occurred four months after the first visit. (G, H, I) Photos taken without PMTC at the third visit, which occurred four months after the second visit. (J, K, L) Photos taken without PMTC at the fourth visit, which occurred four months after the third visit.
2. Case 2
A six-year-old boy visited the Department of Pediatric Dentistry in Yonsei University Dental Hospital with the chief complaint of BS. He had no remarkable medical or dental history. Clinical and radiological examinations did not reveal any dental problems requiring treatment excluding BS. He had fully deciduous dentition and BS affected all of his teeth except for his upper central primary incisors. The cervical thirds of both the buccal and lingual sides were covered with BS (Fig. 2A). Both of his upper primary canines and first primary molars had more BS than the other teeth, covering almost half of the teeth’s smooth surfaces. The patient did not have a dietary problem or halitosis but did have an oral hygiene problem. The patient was indifferent about the importance of brushing teeth. After BS was removed, the patient was instructed on how to brush his teeth using Bass method, and it was recommended that he used a toothbrush with stiff bristles, and he was prescribed with essential oil-containing mouth rinse (Listerine Total Care Mild). Detailed instruction and precautions for using essential oil-containing mouth rinse was same with case 1. The patient returned after four months and the BS had only recurred to approximately 10% of its previous levels (Fig. 1B).
Ⅲ. Discussion
BS is black due to the ferric sulfide that form when hydrogen sulfide reacts with metal salts in the mouth[8]. Some Actinomyces strains produce hydrogen sulfide, which can form ferric sulfide in the presence of metal salts in the saliva or gingival exudates[3]. Actinomyces belongs to the resident oral microbiota of supra-gingival plaque and Actinomyces is abundant in plaque of BS patient so, Actinomyces is expected to be the cause of BS. Actinomyces may not be the only microorganism involved in BS formation[3,9], because BS patients’ dental plaque also contains more Cardiobacterium, Haemophilus, Corynebacterium, Tannerella, Treponema than those without BS. On the other side, bacterial diversity of BS is lower than those without BS[10]. Therefore, richness of Actinomyces as well as this ecological imbalance which is named dysbiosis can be considered starting point for BS[11]. Some researchers reported that BS is weakly positively correlated with the frequency of caries and strongly positively correlated with gingivitis[4,12], likely as a result of reduced levels of Streptococcus mutans, one of the main pathogens of dental caries[13]. These relationships may also be a product of the biofilm’s higher calcium and phosphate content[8] and the higher salivary buffer capacity of BS patients[9].
In these case reports, the essential oil-containing mouth rinse played an important role in slowing BS formation and pigmentation maturation in the dental plaque mass. Essential oils are combinations of phenolic compounds including eucalyptol, menthol, methyl salicylate, and thymol. Essential oils have antibacterial properties and do not have any adverse effects in this context. They do not impair dental material when directly exposed to, and their alcoholic solvents are not to associated with xerostomia or oropharyngeal cancer[7]. The following mechanisms support the bactericidal effects of essential oils. Essential oils cause protein denaturation and alter cell membranes, resulting in the leakage of intracellular contents, which leads to cell death. Especially, thymol perforates the cell membrane. Essential oils can also alter bacterial enzyme activity and inhibit prostaglandin synthetase formation, giving them anti-inflammatory properties. Even their anti-inflammatory properties are seen at lower concentrations than their anti-bacterial properties[7]. As a result, apoptosis occurs and cells cannot reproduce, resulting in lower bacterial mass and toxicity[14,15].
Essential oils can improve oral hygiene when used in combination with tooth brushing. Essential oils can penetrate deeply into interproximal dental plaque mass, reducing gingivitis severity[16-18]. Much of the bacteria that survive initial exposure to essential oils are later killed after coming into contact with essential oils remaining in the mouth[15]. It is not clear whether essential oils are more effective than fluoride or chlorhexidine gluconate (CHG) as a mouth rinse[19], but essential oils have more advantages than fluoride or CHG[20]. Essential oils kill a wide variety of both aerobic and anaerobic bacteria, such as Aggregatibacter actinomycetemcomitans, Actinomyces viscosus, Streptococcus mutans, Streptococcus sanguis, and Bacteroides[7]. Essential oils can also kill gram-positive bacteria, which can grow up colonies by adhering to acquired pellicle[12,21]. Although CHG is the golden standard antimicrobial mouth rinse, it is not often used on a daily basis due to its side effects, such as causing calculus formation, altering patients’ sense of taste, causing discoloration, and allowing opportunistic infection[22]. Furthermore, CHG’s effectiveness is reduced when it interacts with blood serum, other antimicrobial agents, and toothpaste. In contrast, essential oils have a neutral electrical charge, so they do not interact with charged ions found in blood serum, other antimicrobial agents, or toothpaste[7]. Thus, essential oil-containing mouth rinses can be used immediately after tooth brushing, whereas CHG-containing mouth rinse may be done at least 30 minutes after tooth brushing has been done. It is possible to dilute essential oils by up to 50%, because some patients want to reduce its bitter taste. Such dilution does reduce their antibacterial effectiveness. Essential oils diluted to 25% do not have any effect but, more than 50% is effective[7]. As long as essential oils have a concentration of at least 50% they can reduce initial colony formation[15]. Using a mouth rinse of 50% essential oils at least twice per day for 30 seconds at a time can improve oral health[7]. This is why the patients in this study may use 50% essential oil mouth rinse twice per day for 30 seconds at a time.
Recently, researchers have been trying to find alternative treatments for BS. It is a way to interfere with accumulation of dental plaque or prevent ferric sulfide formation by removing metal salts. Probiotics with Streptococcus salivarius M18 counteract BS by inhibiting plaque formation producing dextranase and urease. It has the additional ability to reduce the number of Actinomyces, which relieves BS[5]. Cinnamon, cranberry, and other herbal mouth rinses are also effective anti-plaque agents. Its anti-adhesion ability prevent reformation of BS[22]. Lactoferrin, in a different way, help treat BS by absorbing iron. Lactoferrin can modulate iron homeostasis in oral cavity through sequestration of ferric salts. Lowered ferric salts concentration decreases BS formation. It is additional that low ferric salts concentrations reduce reproduction of bacteria[23]. None of these alternatives are proved to outperform essential oil- or CHG-containing mouth rinses. In addition to these alternatives, diet can also have an effect. Consuming food with high iron content and high-pH water are all risk factors of BS[10]. Drinking tap water aggravates BS more than purified water [10]. If accompanied by a diet, treatment for BS prevention will be more effective.
This case report has two limitations. One is about absence of strict variable control. Methods of oral hygiene management except for mouth rinsing were not controlled. Repeated tooth brushing instruction, characteristic of toothbrushes and diet therapy can be no less associated with relief of BS than essential oil mouth rinse. Comparison of effect of each factor (essential oil, characteristics of toothbrushes, diet) was not considered. The other limitation is dependence on patient’s cooperation. Suggested therapies in this report except for PMTC were not treatments conducted directly by dentists, but types of prescription or patient education. Dentists can recommend, but not force the patient. Therefore, the dentists’ intention is reflected in the results differently depending on the patient’s level of cooperation. If these limitations are considered in subsequent clinical studies, the effectiveness and importance of essential oil to BS patients will be more detailed.
Ⅳ. Summary
Black staining is painless but can cause social problems. Conventional treatments like professional mechanical tooth cleaning and scaling must be repeated because black staining can recur. Antimicrobial medications and probiotics may be able to treat black staining but their side effects are unknown. This study proved the effectiveness of essential oil-containing mouth rinses in younger patients. Essential oils are derived from natural substances and they do not strongly react chemically with other medicines and intra-oral tissue, so they are thought to be a stable option. Essential oils disturb bacterial adherence to tooth surfaces, lengthen the bacterial reproduction cycle, and destroy bacterial cell walls. This study showed that accurate tooth brushing followed by the use of essential oil-containing mouth rinses is an effective way to prevent recurrence of black staining in children. It can be additive treatment option to patients with black staining.