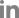|
 |
| J Korean Acad Pediatr Dent > Volume 44(2); 2017 > Article |
|
žīąŽ°Ě
Ž≥ł žóįÍĶ¨žĚė Ž™©ž†ĀžĚÄ ŪÉąÍĶ¨žĄĪ žÜźžÉĀžĚĄ ŽįõžĚÄ žú†žĻėžóź žčúŪĖČŪēú Í≥†ž†ēžą†žĚė žĻėŽ£Ć Í≤įÍ≥ľŽ•ľ Ž∂ĄžĄĚŪēėŽäĒ Í≤ÉžĚīŽč§. Ž≥ł žóįÍĶ¨ŽäĒ 2010ŽÖĄŽ∂ÄŪĄį 2015ŽÖĄÍĻĆžßÄ ŪÉąÍĶ¨žĄĪ žÜźžÉĀžúľŽ°ú Ž≥łÍ≥ľžóź ŽāīžõźŪēėžó¨ žú†žĻėžóź Í≥†ž†ēžą†žĚĄ žčúŪĖČŪēú 92Ž™ÖžĚė ŪôėžēĄŽď§žĚĄ ŪõĄŪĖ•ž†ĀžúľŽ°ú Ž∂ĄžĄĚŪēėžėÄŽč§. žĚīŽď§ ž§ĎžóźžĄú 6ÍįúžõĒ žĚīžÉĀ ž∂Ēž†Ā Í≤Äžā¨žóź žįłžó¨Ūēú ŪôėžēĄŽď§žĚĄ ŽĆÄžÉĀžúľŽ°ú žĻėŽ£Ć Í≤įÍ≥ľŽ•ľ Ž∂ĄžĄĚŪēėžėÄŽč§. žĻėŽ£Ć Í≤įÍ≥ľŽäĒ Í≤Ğߥ ÍłįÍįĄŽŹôžēą žěĄžÉĀ ŽįŹ Žį©žā¨žĄ† Í≤Äžā¨žóźžĄú Ūē©Ž≥Ďž¶ĚžĚė ž°īžě¨žóź ŽĒįŽĚľ Ž∂ĄžĄĚŽźėžóąŽč§.
ŪŹČÍ∑† ŽāėžĚīŽäĒ 42.1ÍįúžõĒžĚīžóąžúľŽ©į 67.4%ÍįÄ Žā®žēĄžėÄŽč§. ŽĄėžĖīžßźžĚī ÍįÄžě• ŽĻąŽ≤ąŪēú žõźžĚłžĚīžóąžúľŽ©į, ŪŹČÍ∑† Í≥†ž†ē ÍłįÍįĄžĚÄ 2.4ž£ľžĚīžóąŽč§. Í≥†ž†ēžą†žĚė žĄĪÍ≥ĶŽ•†žĚÄ 58.9%žĚīžóąŽč§. žēĄŪÉąÍĶ¨ÍįÄ ÍįÄžě• ŽÜížĚÄ žĄĪÍ≥ĶŽ•†žĚĄ Ž≥īžėÄžúľŽ©į, žł°Žį© ŪÉąÍĶ¨žóźžĄú ž†ēŽ≥Ķ ŪõĄ Í≥†ž†ēžą†žĚĄ žčúŪĖČŪēú Í≤Ĺžöį ÍįÄžě• ŽāģžĚÄ žĄĪÍ≥ĶŽ•†žĚĄ Ž≥īžėÄŽč§. ŪÉąÍĶ¨žĄĪ žÜźžÉĀžóźžĄú žĻėžąėÍīīžā¨ÍįÄ ÍįÄžě• ŽĻąŽ≤ąŪěą ŽįúžÉĚŪēú ŽĻĄŪėłžĚėž†Ā žĻėŽ£Ć Í≤įÍ≥ľžĚīžóąŽč§.
Ž≥ł žóįÍĶ¨Í≤įÍ≥ľ, žú†žĻėžĚė ŪÉąÍĶ¨žĄĪ žÜźžÉĀžóźžĄú Í≥†ž†ēžą†žĚÄ ŽįõžēĄŽď§žĚľ ŽßĆŪēėžėÄžúľŽ©į, Í≥†ž†ēžą†žĚÄ žú†žĻėžĚė ŪÉąÍĶ¨žĄĪ žÜźžÉĀžčú žĻėŽ£ĆŽ≤ēžúľŽ°ú Í≥†Ž†§Žź† žąė žěąŽč§.
Abstract
This study investigated the prognosis of luxation injuries in primary teeth treated with splinting. This study retrospectively analyzed 92 children with luxation injuries to their primary teeth who were treated with splints between 2010 and 2015. Prognoses were analyzed in patients who had been followed for more than 6 months. The prognoses with splinting were based on clinical and radiographic evaluations performed during the follow-up examinations.
The mean patient age was 42.1 months, and 67.4% were male. The most common cause of luxation injury was falling, and the mean splint duration was 2.4 weeks. The success rate of splinting was 58.9%. The highest rate of success was achieved following subluxation, while repositioning and splinting of lateral luxation had the lowest rate of success. Pulp necrosis was the most common unfavorable prognosis in the luxation injuries.
Depending upon the type of luxation, splint therapy had acceptable prognoses and might be a feasible treatment option.
Luxation injuries comprise a large proportion of traumatic dental injuries (TDIs) in primary teeth, due to the resilience of alveolar bone [1]. Various luxation injuries are possible depending upon the force and direction of impact. Treatment methods vary according to the type of injury [1].
One of the treatments for stabilizing traumatized teeth is splinting, which allows periodontal tissue regeneration while providing protection from further injury. Flexible or semi-rigid fixation is sufficient for healing pulp and periodontium in most TDIs, and rigid fixation is recommended for cervical root fractures [1-3]. When ankylosis is not a significant risk, a fixation period of 2 - 3 weeks is recommended [1]. Following injuries to the bone, however, 1 - 2 additional weeks are required [4].
The International Association for Dental Traumatology (IADT) guidelines recommend splinting of the primary teeth only for alveolar bone fractures and root fractures [5]. Moreover, repositioning and splinting of traumatized primary teeth requires caution regarding the permanent successors [1].
Despite the significance of primary tooth injuries, few studies have examined this topic. Recently, however, trials have examined the splinting of traumatized primary teeth following alveolar process fracture, horizontal root fracture, and lateral luxation [6-9]. To advance our knowledge of TDIs, such trials are important, and should be continued. The purpose of this study was to evaluate the prognoses of luxation injuries following the splinting of primary teeth.
This study was performed in the Department of Pediatric Dentistry, School of Dentistry, Kyung Hee University, Seoul, Korea. The study proposal was reviewed and approved by the Ethics Committee (KHD IRB 1606-4). This study retrospectively analyzed the medical records of children who were treated using splints on their primary teeth between 2010 and 2015. A total of 838 patients (1534 teeth) visited our department for treatment of luxation injuries of their primary teeth. Of these, 92 patients (202 teeth) were treated using splints and selected for reevaluation. Among the 92 patients, 79 patients were treated with flexible round stainless steel wire (SS-GFS; Ormco, Orange, CA, USA) and flowable composite resin. Nine patients were treated with monofilament nylon fishing line (FL-GFS; HL-1553, HDF, Busan, Korea) and flowable composite resin. In two patients, the teeth were splinted with flexible tri-flex stainless steel wire (TF-RS; RMO, Denver, CO, USA) and flowable composite resin. In the others, the teeth were fixed with flowable composite resin.
Clinical records, intraoral photographs, and radiographs were assessed. Radiographic data were collected to evaluate the prognoses with splinting. Data were analyzed according to age, gender, cause of injury, type of TDI, splinting method, and fixation period. Patients with incomplete records or radiographic examinations were excluded.
Luxation injuries were classified into concussion, subluxation, intrusive luxation, extrusive luxation, lateral luxation, and avulsion [1,10]. Treatment prognoses were analyzed in 57 patients (124 teeth), with a follow-up period exceeding 6 months. Prognoses were categorized based on the presence of associated complications in the clinical and radiographic examinations. Favorable prognoses had total or partial pulp canal obliteration, without complications [5]. Unfavorable prognoses included pulp necrosis, pathological root resorption, loss of teeth, ankylosis, and pathological bone resorption [1]. Success rates were calculated as the ratio of teeth with favorable prognoses to the total number of traumatized teeth in each group.
The study population consisted of 62 boys and 30 girls (sex ratio 2.07 : 1). The average age was 42.1 ¬Ī 17.4 months, and the most prevalent age was 4 - 5 years, followed by 2 - 3 years. Table 1 shows the distribution of splinting in primary teeth by age and gender.
The main cause of injury was falling (53.3%; Fig. 1); the most common place of injury was in the home (42.4%). All teeth treated by splinting were anterior teeth; the primary maxillary central incisor (67.7%) was the most commonly injured tooth. Table 2 shows the rates of splinting among the primary teeth. The highest rate of splinting was in extrusive luxation (28.9%), followed by lateral luxation (22.2%). The mean duration of splinting was 2.4 weeks (Table 2).
The total number of teeth analyzed was 124, and complications were diagnosed within an average follow-up period of 22.1 ¬Ī 14.5 months. The success rate of splinting was 58.9%; subluxation injuries had the highest success rate. Conversely, repositioning and splinting of lateral luxation injuries resulted in the lowest success rate (Fig. 2).
Pulp necrosis (16.1%) was the most common complication. The distribution of complications is shown in Table 3.
Traumatic dental injuries of primary teeth have a prevalence of approximately 30 - 40% [11-13]. In addition, luxation injuries are more frequent in primary teeth than are fractures [1,14]. Despite the prevalence of TDIs, few studies have examined splinting treatment in primary teeth. Therefore, this study focused on luxation injuries in primary teeth treated using splinting.
The predominant age group in this study was 4 - 5 years (Table 1). This was in agreement with studies that found an increased incidence of TDIs in children between the ages of 3 and 5 years [15-17]. However, this finding disagreed with other studies reporting that the peak age of TDI incidence in children is 2 - 4 years [1,15,18,19].
Boys had a higher incidence of injury than girls (2.07 : 1), which was consistent with other studies [11,18,20,21] and may reflect the observation that boys are more energetic and more likely to take part in outdoor activities than girls are [22]. The predominant age of boys in the series was 4 - 5 years, while that of girls was 2 - 3 years. This was in agreement with study that found the predominant age of boys was older than that of girls [17].
The most common cause of the injuries was accidental falls (Fig. 1). Falls and collisions accounted for 90% of cases, consistent with previous reports [18,21,23-25]. The most common location for TDIs to occur was the home, followed by the kindergarten classroom. This was also consistent with previous studies [18,23,24].
The rate of splinting of luxation injuries was 13.2% (Table 2). One study reported that 9% of luxated primary teeth were treated using splinting [26]. Splinting can decrease the initial mobility of teeth and related pain, and may prevent children from touching their mobile teeth [8].
The current guidelines recommend splinting of traumatized primary teeth only following root displacement and alveolar bone fractures [5]. Andreasen et al. [1] recommended a splint for 2 - 3 weeks in the case of luxation with occlusal interference. In agreement with this suggestion, the rates of splinting in extrusive and lateral luxation injuries were higher than those in other luxation injuries.
Traumatic dental injuries in the primary teeth can cause clinical complications, including color changes, pulp necrosis, pulp canal obliteration, external root resorption, and internal root resorption [1]. Favorable and unfavorable prognoses were identified based on the literature [5,19]. The frequency of secondary pulp necrosis among teeth with pulp canal obliterations is low [1,14,27-29]. Consequently, partial or total pulp canal obliteration was considered a clinical success. Unfavorable prognoses included pulp necrosis, pathologic root resorption, loss of tooth, and pathologic bone resorption.
The average success rate for splinting was 58.9% (Table 3, Fig. 2). As reported, severe periodontal tissue injuries resulted in complications [19,30]. Lateral, intrusive, and extrusive luxation injuries had lower success rates than other injuries. The replantation of avulsed primary teeth is usually not recommended based on the potential damage to permanent successors [1,5]. However, the success rate with avulsed teeth was high in this study, although this finding may have been biased due to the small sample size.
In this study, the highest rate of splinting following luxation injuries occurred in cases of extrusive luxation. The success rate of splinting luxated primary teeth was 58.9%, with subluxations having the highest success rates. This was the first study to investigate the clinical prognoses of splinting in luxated primary teeth, and could be the basis for additional studies investigating TDIs in primary teeth.
Table 1.
Distribution of splinting in primary teeth by age and gender
Table 2.
Rate of splinting in luxation injuries and mean splint durations
References
1. Andreasen JO, Andreasen FM, Andersson L : Textbook and Color Atlas of Traumatic Injuries to the Teeth. 4th ed. Blackwell Munksgaard, Copenhagen, 516-538, 2007.
2. Liu X, Huang J, Bai Y, et al. : Conservation of root-fractured primary teeth-report of a case. Dent Traumatol, 29:498-501, 2013.


3. Filippi A, Pohl Y, Kirschner H : Replantation of avulsed primary anterior teeth: treatment and limitations. ASDC J Dent Child, 64:272-275, 1997.

4. Oikarinen K : Tooth splinting : a review of the literature and consideration of the versatility of a wire-composite splint. Endod Dent Traumatol, 6:237-250, 1990.


5. Malmgren B, Andreasen JO, Flores MT, et al. : International Association of Dental Traumatology guidelines for the management of traumatic dental injuries: 3. Injuries in the primary dentition. Dent Traumatol, 28:174-182, 2012.


6. Akin A, Uysal S, Cehreli ZC : Segmental alveolar process fracture involving primary incisors: treatment and 24-month follow up. Dent Traumatol, 27:63-66, 2011.


7. Bonanato K, Sardenberg F, Santos ER, et al. : Horizontal root fracture with displacement in the primary dentition. Gen Dent, 57:31-34, 2009.
8. Kim GT, Sohn M, Ahn HJ, et al. : Intra-alveolar root fracture in primary teeth. Pediatr Dent, 34:215-218, 2012.
9. Holan G : Conservative treatment of severely luxated maxillary primary central incisors: case report. Pediatr Dent, 21:459-462, 1999.

10. Application of the International Classification of Diseases to Dentistry and Stomatology (ICD-DA). Available from URL: http://www.who.int/classifications/icd/en/(Accessed on
February 9, 2016)
11. Bastone EB, Freer TJ, McNamara JR : Epidemiology of dental trauma: a review of the literature. Aust Dent J, 45:2-9, 2000.


13. Oliveira LB, Marcenes W, Ardenghi TM, et al. : Traumatic dental injuries and associated factors among Brazilian preschool children. Dent Traumatol, 23:76-81, 2007.


14. Boorum MK, Andreasen JO : Sequelae of trauma to primary maxillary incisors. I. Complications in the primary dentition. Dent Traumatol, 14:31-44, 1998.

15. Kramer PF, Zembruski C, Ferreira SH, Feldens CA : Traumatic dental injuries in Brazilian preschool children. Dent Traumatol, 19:299-303, 2003.


16. Granville-Garcia AF, De Menezes VA, De Lira PIC : Dental trauma and associated factors in Brazilian preschoolers. Dent Traumatol, 22:318-322, 2006.


17. Skaare AB, Jacobsen I : Primary tooth injuries in Norwegian children (1-8 years). Dent Traumatol, 21:315-319, 2005.


18. Choi SC, Park JH, Pae A, Kim JR : Retrospective study on traumatic dental injuries in preschool children at Kyung Hee Dental Hospital, Seoul, South Korea. Dent Traumatol, 26:70-75, 2010.


19. Ritwik P, Massey C, Hagan J : Epidemiology and outcomes of dental trauma cases from an urban pediatric emergency department. Dent Traumatol, 31:97-102, 2015.


20. Bae JH, Kim YK, Choi YH : Clinical characteristics of dental emergencies and prevalence of dental trauma at a university hospital emergency center in Korea. Dent Traumatol, 27:374-378, 2011.


21. Kim Y, Kim S, Choi N : A retrospective study of the pattern and treatment of traumatic dental injury to primary and permanent teeth. J Korean Acad Pediatr Dent, 41:314-321, 2014.

22. Rajab LD : Traumatic dental injuries in children presenting for treatment at the Department of Pediatric Dentistry, Faculty of Dentistry, University of Jordan, 1997-2000. Dent Traumatol, 19:6-11, 2003.


23. Galea H : An investigation of dental injuries treated in an acute care general hospital. J Am Dent Assoc, 109:434-438, 1984.


24. Onetto JE, Flores MT, Garbarino ML : Dental trauma in children and adolescents in Valparaiso, Chile. Endod Dent Traumatol, 10:223-227, 1994.


25. Liew VP, Daly CG : Anterior dental trauma treated afterhours in Newcastle, Australia. Community Dent Oral Epidemiol, 14:362-366, 1986.


26. Assunção LRdS, Ferelle A, Iwakura MLH, et al. : Luxation injuries in primary teeth: a retrospective study in children assisted at an emergency service. Brazilian Oral Research, 25:150-156, 2011.


27. Santos BZ, Cardoso M, Almeida IC : Pulp canal obliteration following trauma to primary incisors: a 9-year clinical study. Pediatr Dent, 33:399-402, 2011.

28. Oginni AO, Adekoya-Sofowora CA, Kolawole KA : Evaluation of radiographs, clinical signs and symptoms associated with pulp canal obliteration: an aid to treatment decision. Dent Traumatol, 25:620-625, 2009.


- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 7,020 View
- 251 Download
- Related articles
-
Retrospective Study of Infants who Visited Pediatric Dentistry2020 May;47(2)




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print