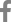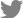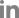|
 |
| J Korean Acad Pediatr Dent > Volume 48(1); 2021 > Article |
|
초록
Short root anomaly는 비정상적으로 짧고 뭉툭한 치근 형태를 가진 드문 질환이다. 대부분 상악 중절치에 대칭적으로 나타나며 영구치에서만 관찰되어 왔다.
이 증례는 9세 여환으로 혼합치열기에 짧은 치근 발달을 주소로 개인병원에서 의뢰되었다. 방사선 사진 및 구강 내 검사에서 법랑질 저형성증과 치내치와 같은 다른 치아이상과 함께 상악 및 하악 전치부와 하악 제 1대구치에서 SRA가 관찰되었다. 5년동안의 장기 추적 관찰을 통해 환아의 모든 치아들은 혼합치열기에서 영구치열기로 변화하였고 모든 영구치에서 전반적인 SRA가 관찰되었다.
교정적 진단을 위해 촬영된 측면 두부 방사선 사진에서 치아 이상과 밀접한 관련이 있는 것으로 보고된 전방과 후방 상돌기 사이의 석회화인 sella turcica bridge 또한 관찰되었다. 이러한 여러 요소들을 통하여 치근 흡수나 치아 상실의 예방과 성공적인 관리 위해 SRA를 조기 진단하는 것은 매우 중요하다.
이 증례 보고에서는 다른 치아이상과 sella turcica bridge와 함께 전악에 걸쳐 나타난 전반적인 SRA를 보이는 환아를 장기적으로 관찰하고 의미있는 결과를 나타내고 있기에 이를 보고하는 바이다.
Abstract
Short root anomaly (SRA) is a rare dental condition with abnormally short and blunt root morphology. It mostly affects maxillary central incisors symmetrically and only has been observed in permanent teeth.
A 9-year-old girl was referred from a local dental clinic for short root development in mixed dentition with no symptoms. Radiographic and intraoral examinations revealed SRA on upper and lower incisors and mandibular first molars along with other dental anomalies such as enamel hypoplasia and dens invaginatus. During long - term follow - up for 5 years, her mixed dentition has changed to permanent dentition and generalized SRA was observed in all permanent teeth. Cephalometric radiograph also revealed the calcification between the anterior and posterior clinoid processes described as a sella turcica bridge which was reported associating with dental anomalies. Early diagnosis of SRA is emphasized for successful management and prevention of root resorption and tooth loss.
This report aimed to present a rare case of generalized SRA along with other dental anomalies and sella turcica bridging in a female patient through long - term follow - up.
Short root anomaly (SRA) is a rare dental anomaly in permanent dentition, which was first discovered by Lind[1] in 1972. SRA is characterized as short and blunt root with pointed or rounded apices, and crown - to - root ratio of 1 : 1 or less[2]. The prevalence of SRA has been reported to be 2.4 % to 2.7 % in Caucasians and 10 % in Mongolians[3]. It mostly affects maxillary central incisors symmetrically and occurs approximately 3 times more in girls than boys[1]. SRA has been caused by familial inherent characteristics rather than root resorption or exogenous disruption[4]. Also, it often accompanied with multiple other dental anomalies such as agenesis, dens invaginatus, supernumerary teeth, microdontia, and taurodontia[5].
Recent studies have reported that the prevalence of dental anomalies in adolescents increases with sella turcica bridging which refers to the calcification of the ligament between the anterior and posterior clinoid processes[6]. Identification of a sella turcica bridge may propose possible appearance of dental anomalies. Since teeth and its surrounding tissues with SRA are clinically normal and asymptomatic, it is difficult to diagnose for teeth with short roots in the mixed dentition[7]. Therefore, the proper early diagnosis of SRA by clues from other anomalies is critical for successful clinical management and prevention of tooth loss.
This report presents a rare case of generalized SRA associated with other dental anomalies and sella turcica bridging in a young female through long - term follow - up.
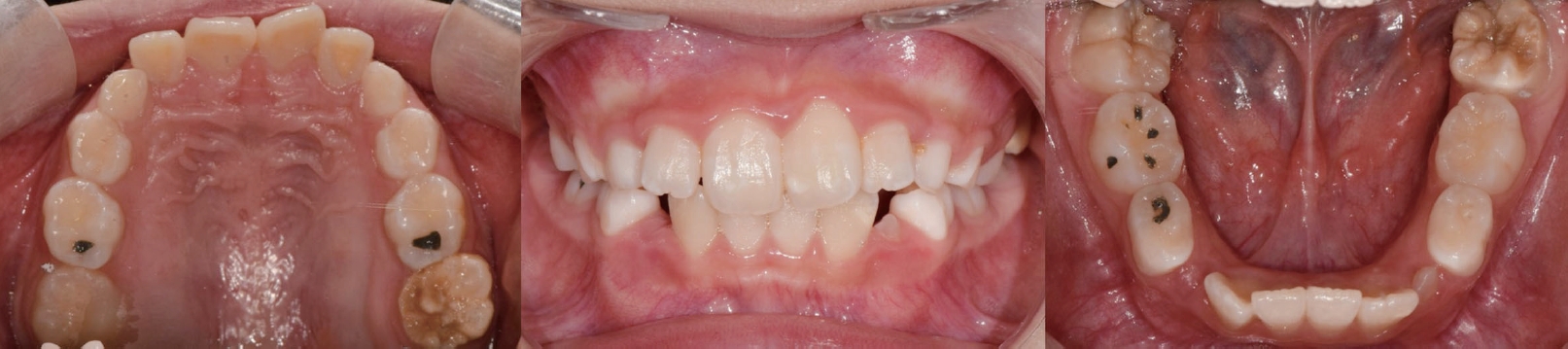
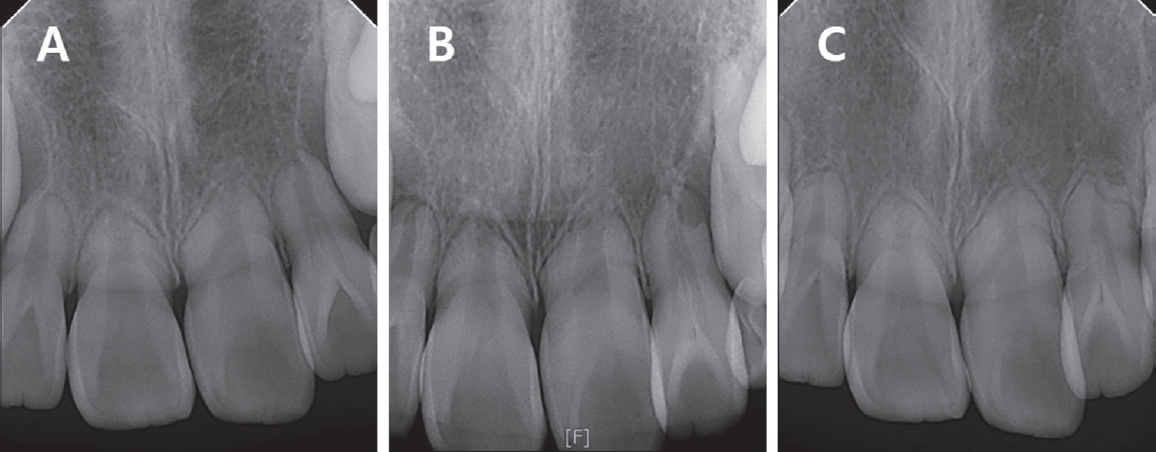
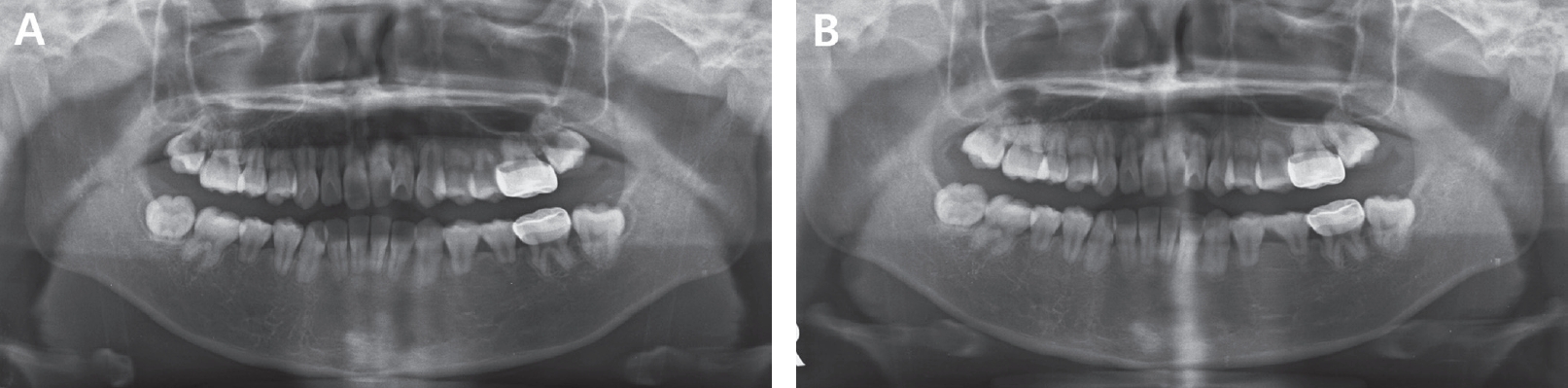
A 9-year-old girl was referred from a local dental clinic for short root development on upper and lower anterior permanent teeth without any symptom or mobility. Her medical history was unremarkable with no history of dental trauma. She was recommended to be examined if there was any systemic disease associated with bone loss by the local dental clinic. Several tests conducted by a pediatrician showed neither any syndromes nor systemic diseases. The first panoramic radiograph and periapical radiographs were taken at her first visit (Fig. 1). Radiographic examination revealed short and blunt tooth roots with rounded apices on maxillary and mandibular incisors and mandibular first molars. Periapical radiographs clearly showed dens invaginatus on left maxillary lateral incisor (Fig. 1). Clinical examination revealed severe enamel hypoplasia on left maxillary and mandibular first molars and mild enamel hypoplasia on both maxillary central incisors and left mandibular lateral incisor. These enamel hypoplasia showed a characteristic of molar incisor hypomineralization. The dental crowns and surrounding oral tissues of maxillary and mandibular incisors appeared within normal limits (Fig. 2). 3 months later, the restorative treatment was performed on left maxillary and mandibular first molars with severe enamel hypoplasia (Fig. 3).
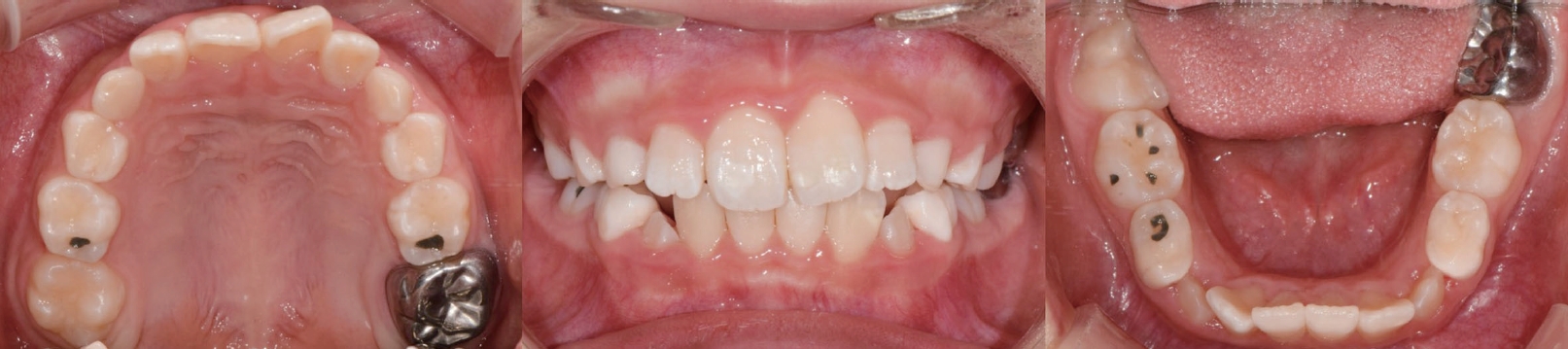
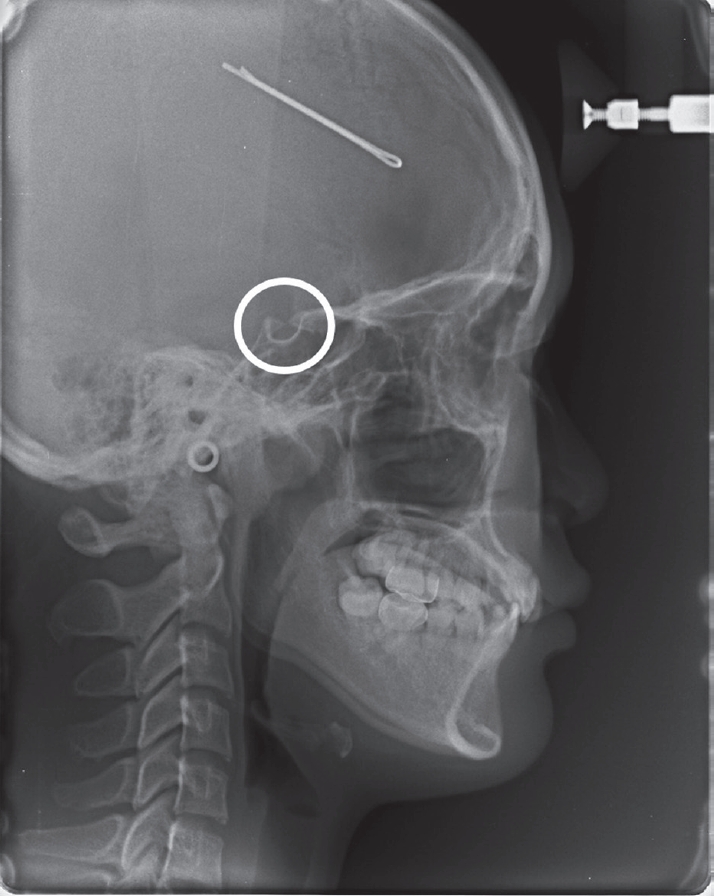
Additional periapical radiographs were taken at the ages of 10 and 11 to periodically observe the left maxillary lateral incisors with dens invaginatus and its degree of root resorption due to a dental follicle of left maxillary canine. The periapical radiograph at the ages of 11 showed root resorption progressed on the left maxillary lateral incisor by the eruption of left maxillary canine (Fig. 4). In consecutive panoramic radiographs at the ages of 9, 12, and 14 (Fig. 1 and 5), it was discovered that the roots of all permanent teeth were abnormally developed exhibiting short and blunt roots. Intraoral examination at the ages of 14 revealed that the dental crowns of all teeth appeared to be normal and there were no symptom or any lesions on apices (Fig. 6). Cephalometric radiograph was taken for orthodontic diagnosis due to mild anterior crowding and it showed partial ossification of the clinoid processes of sella turcica or partial sella turcica bridging (Fig. 7). Orthodontic treatment for mild anterior crowding was not recommended due to the underlying risks of root resorption. In order to follow the root condition and prevent periodontal disease, the patient was strictly kept in regular recall check. The eruption of maxillary and mandibular second molars is recently under observation and their root formations also will be evaluated in the future.
The patient presented in this case showed generalized SRA associated with other dental anomalies such as enamel hypoplasia and dens invaginatus. Generalized SRA is a very rare dental phenomenon affected in almost all the permanent teeth and a challenging anomaly to be diagnosed due to its normal appearance[3]. Short roots can be mainly caused by external root resorption after full root development or congenital disruption of root formation[5]. External root resorption is usually related to systemic diseases, such as bone dysplasias and scleroderma, and considered as an undesirable consequence of orthodontic treatment[4]. Several environmental factors such as trauma, infection, and medical exposure also can cause root resorption[8].
Congenital short root formation is also known to be associated with certain syndromes and systemic conditions[9]. Metabolic diseases, such as idiopathic hypoparathyroidism, pseudohypoparathyroidism, and thalassemia, are as well as related to underdeveloped roots[10]. Teeth with external root resorption appear a different shape of the apical surface compared to teeth with SRA. The apical surface of teeth with resorbed roots shows irregular and gradual shortening while the apical surface in SRA shows smooth and rounded roots without additional resorption[1,11].
In previous studies, a molecular characteristic of the gingival crevicular fluid (GCF) from SRA patients was reported as the activation, complex formation, and fragmentation of matrix metalloproteinase 9 (MMP - 9). This has supported the fact that root shortening in SRA patients was developmentally induced rather than root resorption because MMP - 9 had low collagenolytic resorptive activity while other MMPs, which were mostly detected in GCF of active periodontitis and gingivitis patients, showed high collagenolytic activity[12]. Recent animal studies also disclosed that the nuclear factor Ic (Nfic) gene was significantly associated with development of root formation and odontoblast differentiation[13]. Deficiency of Nfic gene caused the development of short and abnormal roots by disrupting odontoblast differentiation[13,14].
Through consecutive radiographic monitoring for 5 years from mixed dentition to permanent dentition, the present patient has been diagnosed as a generalized SRA without any syndromes or systemic conditions. This made the generalized SRA reported in this case very rare and difficult to be differentially diagnosed from immature permanent teeth at mixed dentition. The radiographic and clinical findings in this case were consistent with generalized SRA rather than external apical root resorption. This generalized SRA was defined as nonsyndromic SRA because the patient’s medical history, clinical examination, and blood tests were all within normal range. Therefore, this evidence suggested that the generalized SRA of the present patient could be caused by genetic inheritance. This condition was also accompanied with enamel hypoplasia on first permanent molars and incisors and dens invaginatus on left maxillary lateral incisor. The genetic theory could be emphasized by these tooth developmental anomalies presented along with SRA.
Besides several dental anomalies, the patients also appeared alteration of sella turcica morphology as known as sella turcica bridging on a cephalometric radiograph obtained for orthodontic analysis. Sella turcica bridging is excessive calcification of interclinoid ligaments of sella turcica and mostly caused by congenital defects[6]. The sella turcica bridge is prevalently associated with craniofacial deviations, syndromes, as well as multiple dental anomalies. This might be considered to be the shared genes and neural crest cells involved in development and differentiation of sella turcica and teeth[15]. According to Leonardi et al .[6], the presence of sella turcica bridging in early life can notify clinicians the possibility of dental anomalies appeared later in life.
Because generalized SRA is clinically not obvious, sequential radiographic assessment is necessary for an accurate diagnosis avoiding misdiagnosis of the SRA as external root resorption[5]. Early treatment of dental caries and prevention of periodontal inflammation are essential to inhibit loss of tooth and maintain general oral health in SRA dentitions. In the present case, the patient has been undergone restorative treatment on first permanent molars severely affected with enamel hypoplasia. She has been also placed under strict periodic observation on progressive root resorption of the left maxillary lateral incisors with dens invaginatus. Since oral prophylaxis and fluoride application have been performed periodically to prevent dental caries and periodontal disease, the patient has been maintaining healthy oral environment and free of caries so far. Also, extractions of the deciduous teeth at appropriate timing were provided for a spontaneous eruption as an interceptive treatment. Clinicians should encourage the SRA patients to avoid exertion of heavy force on teeth with shortened roots and implement strict regular radiographic monitoring on them. Because SRA could be genetically inherent, radiographic examinations of SRA patients’ parents and siblings and investigations on familial occurrence are recommended for proper diagnosis, if possible. Also, it will be helpful to correctly diagnosis SRA if genetic test and gelatin zymography of GCF are conducted. Further researches on prognosis of generalized SRA through long - term follow - up are needed to predict sequelae of any treatment on SRA patients.
SRA is an uncommon dental condition mostly observed in the permanent dentition. The case presented in this report showed generalized SRA along with other dental anomalies and sella turcica bridging, in which etiologic factors were irrelevant with any syndromes or systemic conditions. Early diagnosis through accurate clinical, radiographic and genetic examinations is very important to maintain and improve the oral health of the patients with SRA.
Fig 1.
Panoramic and periapical radiographs of the patient at first examination. The radiograph was obtained when the patient was 9 years old.
References
2. Vishwanath M, Chen PJ, Yadav S, et al. : Orthodontic management of a patient with short root anomaly and impacted teeth. Am J Orthod Dentofacial Orthop, 155:421-431, 2019.


3. Apajalahti S, Arte S, Pirinen S : Short root anomaly in families and its association with other dental anomalies. Eur J Oral Sci, 107:97-101, 1999.


4. Michelogiannakis D, Vastardis H, Tosios KI, et al. : The challenge of managing patients with generalized short root anomaly: A case report. Quintessence Int, 49:673-679, 2018.

5. Marques LS, Generoso R, Pazzini CA, et al. : Short-root anomaly in an orthodontic patient. Am J Orthod Dentofacial Orthop, 138:346-348, 2010.


6. Leonardi R, Barbato E, Caltabiano M, et al. : A sella turcica bridge in subjects with dental anomalies. Eur J Orthod, 28:580-585, 2006.


7. Lee J, Lee J, Ra J, et al. : Orthodontic Treatment of a Child with Short Root Anomaly : a Case Report. J Korean Acad Pediatr Dent, 42:319-326, 2015.

8. Hegde S, Shubha AB, Rao BD, et al. : Extensive idiopathic external apical root resorption on a 13 year old child. J Clin Pediatr Dent, 36:289-292, 2012.


9. Desai RS, Vanaki SS, Nidawani P, et al. : An unusual combination of idiopathic generalized short-root anomaly associated with microdontia, taurodontia, multiple dens invaginatus, obliterated pulp chambers and infected cyst: a case report. J Oral Pathol Med, 35:407-409, 2006.


10. Jensen SB, Illum F, Dupont E : Nature and frequency of dental changes in idiopathic hypoparathyroidism and pseudohypoparathyroidism. Scand J Dent Res, 89:26-37, 1981.


11. Di Domizio P, Orsini G, Piattelli A, et al. : Idiopathic root resorption: report of a case. J Endod, 26:299-300, 2000.


12. Apajalahti S, Sorsa T, Ingman T : Matrix metalloproteinase -2, -8, -9, and -13 in gingival crevicular fluid of short root anomaly patients. Eur J Orthod, 25:365-369, 2003.


13. Park JC, Herr Y, Cho MI, et al. : Nfic gene disruption inhibits differentiation of odontoblasts responsible for root formation and results in formation of short and abnormal roots in mice. J Periodontol, 78:1795-1802, 2007.


- TOOLS
-
METRICS

-
- 0 Crossref
- 0 Scopus
- 3,111 View
- 135 Download
- ORCID iDs
-
Dayeol Yu

https://orcid.org/0000-0003-3232-4352Donghyun Kim

https://orcid.org/0000-0003-2442-3254 - Related articles




 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link Full text via DOI
Full text via DOI Download Citation
Download Citation Print
Print